
Lifestyle factors aren’t enough
For years, cardiologists have pointed to high blood pressure, cigarette smoking, family history, and high cholesterol as the key clues that someone may be developing heart disease—the leading cause of death in the United States. Now, however, research published in 2017 in the journal Circulation found that a combination of five simple heart tests is more effective in predicting cardiovascular disease than looking at lifestyle factors alone. After studying a group of healthy individuals for more than 10 years, the researchers found that those who scored poorly on all five tests were 20 times more likely to develop heart disease than those with good results. Here’s what you need to know about these heart tests.
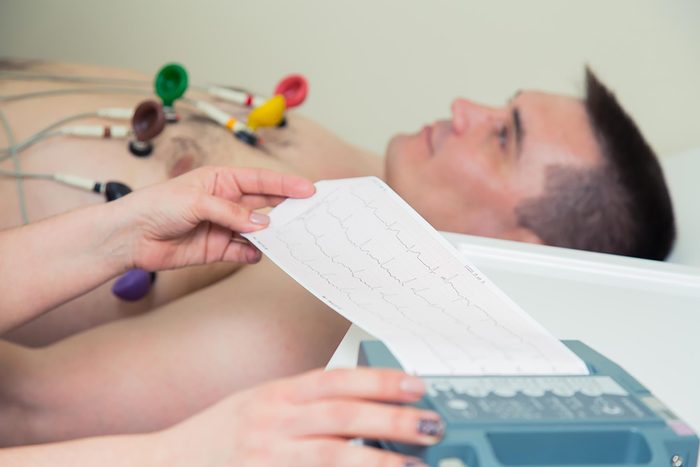
Electrocardiogram
A standard 12-lead electrocardiogram, also known as an EKG, is one of the standard heart tests used to measure the electrical activity of the heart muscle. It’s non-invasive, painless, and quick—it usually only takes five to 10 minutes—and it’s considered one of the best ways to assess heart disease risk. During an EKG, your doctor will place 10 small electrodes on your limbs and chest that measure your heart’s electrical activity and will detect any abnormal rhythms and patterns that are commonly associated with heart attacks, arrhythmia, and other dangerous cardiovascular conditions.
Andrew M. Freeman, MD, director of cardiovascular prevention and wellness at National Jewish Health and co-chair of the American College of Cardiology’s nutrition and lifestyle workgroup, says an EKG is typically used as a baseline test for new patients or for anyone showing symptoms of heart disease. While the average person doesn’t need to undergo the procedure very often, those who smoke, have high cholesterol, or have a family history of heart disease should consult with their doctor to see how often they should get tested. Here are doctor-recommended tips for a healthy recovery after a heart attack.
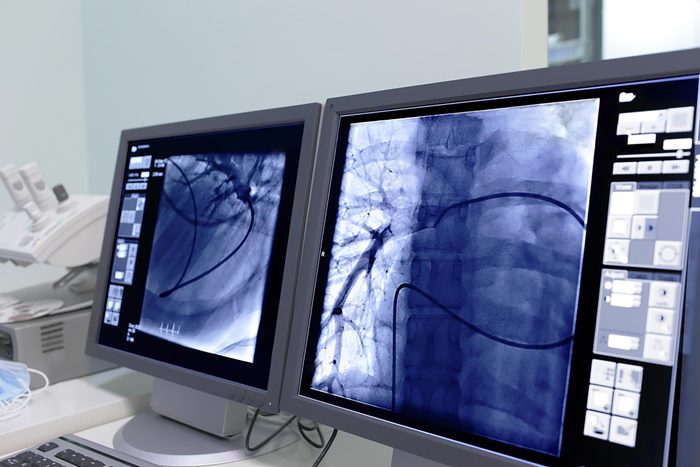
Coronary calcium scan
If your doctor suspects you may be at risk for developing heart disease, they might perform a coronary calcium scan. This low-radiation CT scan reveals the amount of calcium built up in your coronary arteries. “When we see calcium in the coronaries, it means that there’s some degree of atherosclerosis—sludge in the pipes that supply the coronaries,” Dr. Freeman says.
In general, lower levels of calcium in the arteries are linked with better heart health, he says, while high levels may indicate an increased risk of heart attack or other cardiovascular events. People with high cholesterol, high blood pressure, a family history of early heart disease, or other traditional heart disease risks may need to undergo the scan more frequently. Dr. Freeman also warns that men, especially those over the age of 70, are more likely to experience coronary calcium buildup.
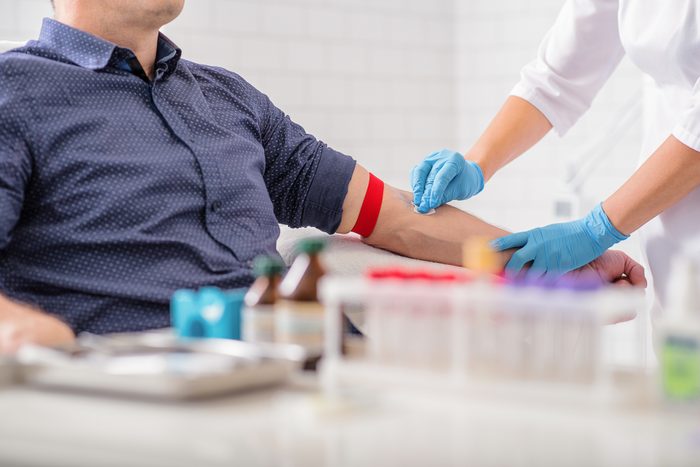
Blood test for C-reactive protein
The first of three blood tests used to assess heart disease risk measures the amount of C-reactive protein, or CRP, in your bloodstream. CRP rises with increased inflammation in the body, which Dr. Freeman says is an underlying condition of many health problems, including heart disease. While there is no evidence that inflammation directly causes heart disease, he explains that the two are closely correlated because higher levels of inflammation are typically associated with cardiovascular issues.
A CRP test can indicate you need to take preventative measures to block heart disease before it starts; Dr. Freeman recommends eating a plant-based diet, exercising, relieving stress, and forming close connections and relationships with others. (Here are the 50 best foods for your heart.)
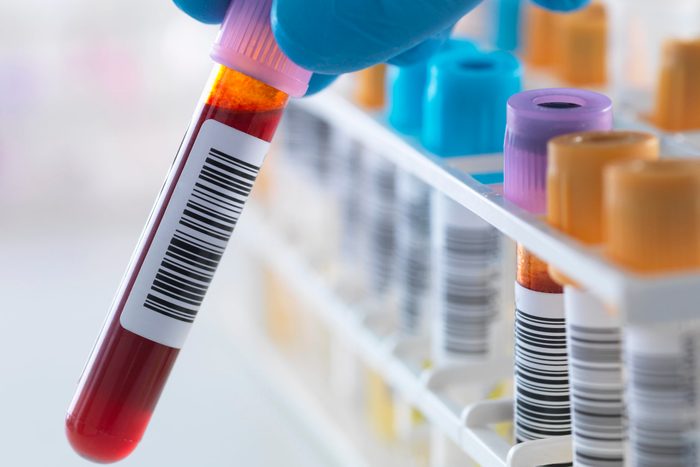
An NT-proBNP blood test
Your cardiologist may also test your blood for a chemical known as NT-proBNP. BNP, or brain natriuretic peptide, is a hormone released by both your brain and your heart in response to cardiovascular stress. As Dr. Freeman explains, a blood test that shows a high level of BNP is a red flag that your heart muscle has stiffened and may not relax as well it once did; often, this can be due to a lack of regular activity. Officially known as diastolic dysfunction, this condition can be an early predictor of heart failure. With some simple lifestyle changes, you can decrease the amount of stress you place on your heart, starting with eating a healthy diet, working out regularly, and quitting smoking. (Check out these 44 ways cardiologists keep their hearts in good shape.)
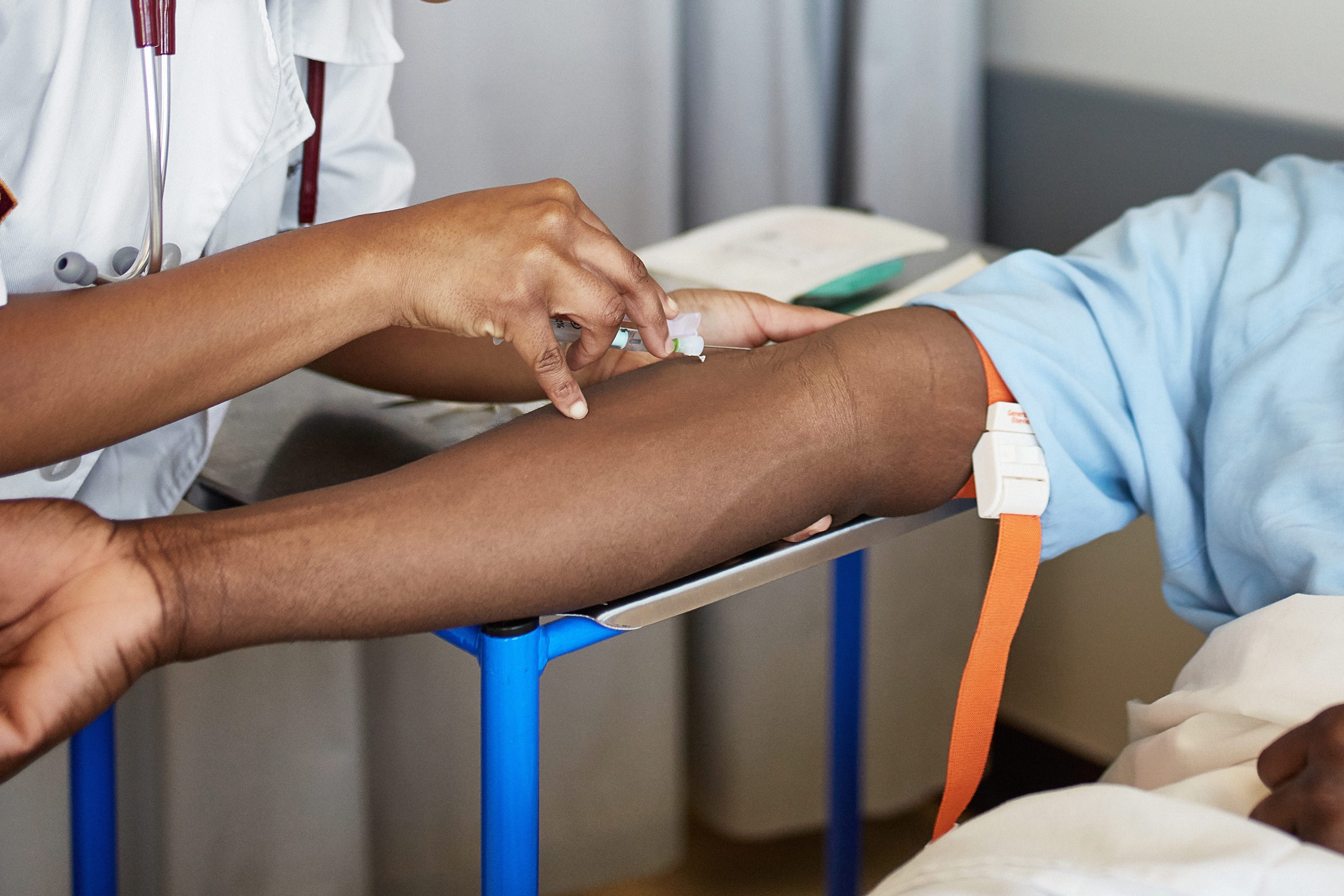
A high-sensitivity blood test for troponin T
The final heart test mentioned in the study used to assess heart disease risk is a highly sensitive blood test that measures your levels of a protein known as troponin T. Troponin T is released when your heart faces significant stress or gets damaged. A typical troponin test can only pick up on large quantities of the protein, released during dire and taxing events for your heart, such as running a marathon or having a heart attack. However, the new version can detect much lower levels of troponin T, and identifying the smaller quantities of troponin allows doctors to begin treating heart damage early, rather than waiting for a heart attack or stroke to let you know something’s wrong.