
What’s behind your pelvic pain?
While you may assume that all pelvic pain is caused by gynecologic disease, it can be more complex than that and causes vary. “Pain in the pelvis can originate from the urinary tract, reproductive organs, pelvic floor muscles, bones and joints of the pelvis, digestive tract, lower back, or the nervous system,” says Sarah Hwang, MD, director of Women’s Health Rehabilitation at Shirley Ryan AbilityLab and Assistant Professor of Physical Medicine and Rehabilitation and Obstetrics and Gynecology at Northwestern Feinberg School of Medicine. Learn the 15 things no one tells you about this source of pelvic pain.

Pelvic pain is tough to pinpoint
Not all pelvic pain is straightforward. The pain can start off sharp and occasional and then become constant and achy. Or it can change location, originating on the right side and moving to both sides, explains Dr. Hwang. All of this information is important for your doctor to know. Jot down notes about the timing, location, severity, sharpness, and activities, like if you were having sex or going to the bathroom when it happened.

Pelvic pain is incredibly common
One study of women seeking care for conditions like pain, infertility, menstrual problems, or tubal sterilization noted that 30 percent of women reported chronic pain, including those who didn’t have any pelvic disorders. “Our study suggests that many reproductive-age women are experiencing but not reporting some form of pelvic pain,” study author Karen Schliep, PhD said in a press release. The authors note that women should speak up if they’re in pain, as it can be a sign that more tests (many of which are non-invasive) need to be done.
Mild discomfort may be period cramps
If you’re a woman, you may be all too familiar with uncomfortable cramping around the time of your period, as your uterus contracts to shed the uterine lining, and this can be a source of temporary pelvic pain. However, if cramps are interfering with daily activities, your doctor needs to rule out a medical cause (some are included on this list). Read on for 8 period issues that may indicate a health problem.
Pain with your period may be endometriosis
It’s important not to brush off all period cramps as “normal,” especially if the pain is not limited to the pelvic area. When the tissue that lines the uterus starts to grow outside of the uterus, that’s called endometriosis—a condition that’s characterized by pelvic pain but can also include pain in other areas of the body at the time of menstruation. “Women with endometriosis often describe the pain as severe period cramps that occur around the time of their periods,” says Dr. Hwang. There’s more you need to know about this widely misdiagnosed condition.

Chronic, crampy pain may be IBS
If you’ve been plagued with pelvic pain for at least six months, one possible cause is irritable bowel syndrome, which can feel like crampy pain. In one study, 40 percent of women reporting pelvic pain also had IBS. If you have abdominal pain plus changes in bowel movements like diarrhea, constipation, or bloating, make an appointment with your doctor. Check out these 9 signs of IBS everyone should watch out for.

Pain going to the bathroom may be pelvic floor dysfunction
Pelvic floor dysfunction is a term that means you’re unable to correctly contract and relax these muscles during a bowel movement, according to the Cleveland Clinic. The result is problems pooping or fecal or urine incontinence. “This pain is typically seen throughout the month (not just for women during their periods), and typically worsens during intercourse,” says Dr. Hwang. You may also notice that you have to go to the bathroom more frequently or feel pain when you go, she notes. Learn more about your pelvic floor here.

Sharp pain and bloating may be ovarian cancer
Before you worry, know this: About one percent of women who have symptoms like pelvic pain have ovarian cancer, according to a 2010 study in the Journal of the National Cancer Institute. However, if you experience bloating, feeling full quickly, and experience frequent urination; along with pelvic pain, these may be signs of ovarian cancer, which is the fifth most deadly cancer in women. Read this harrowing story of a woman who discovered the sharp pain on the left side of her abdomen was ovarian cancer.
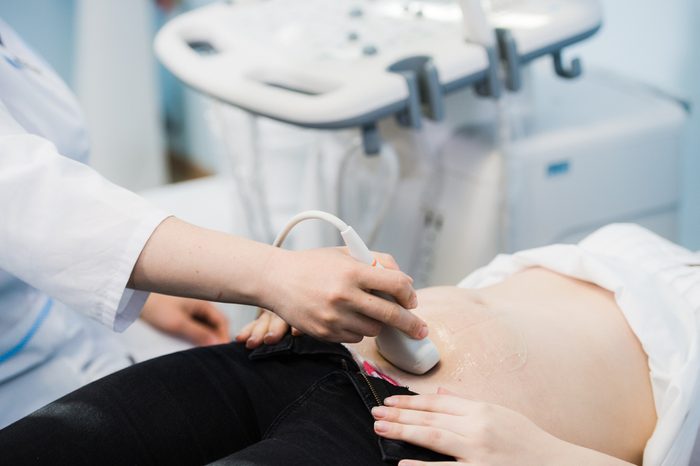
Pressure and bleeding may be uterine fibroids
These noncancerous growths in the uterus often cause no symptoms, according to the Mayo Clinic. But when they do, it may include pelvic pain and pressure, along with heavy and long-lasting periods, problems urinating, and constipation. An ultrasound is often enough to make a diagnosis; if they’re causing significant discomfort, your doctor may prescribe medications to shrink fibroids.
Abrupt pain may be an ovarian cyst
Did the agony seem to appear out of nowhere? “Women with ovarian cyst describe a more sudden onset of severe pain,” says Dr. Hwang. These cysts don’t always lead to issues; in fact, many disappear on their own, says the Mayo Clinic. A cyst that’s especially large can trigger bloating, abdominal fullness—and produce a dull or sharp ache on one side in your lower abdomen, the clinic notes.

Burning or sharp pain may be a bladder problem
A condition called interstitial cystitis (painful bladder syndrome) produces a burning or sharp pain in the bladder or urethra, reports the US Department of Health and Human Services. The pain may be worse when you urinate and can come and go for weeks or months. A spasm in pelvic floor muscles may also cause discomfort. The condition can flare during your period, during sex, or as a result of stress. Lifestyle changes to avoid triggers may bring relief.
Sudden-shock pain may be a nerve issue
If your pain has a severe, zing-like quality, your doctor may consider a nerve condition like pudendal nerve entrapment. The pudendal nerve carries signals to the pelvic floor muscles, perineum, skin of the penis or vulva, and the rectum, and dysfunction can cause pain to whip through this region. Physical therapy with an expert in pelvic floor disorders may be the first-line suggested treatment if your doctor suspects a nerve issue.

When to seek help
There’s no reason to brush off pelvic pain. After all, it may be an important distress signal about an underlying health issue. “Seek medical advice if the pain doesn’t go away or becomes constant, and—most importantly—if it starts to affect your everyday life,” says Dr. Hwang.
