Here’s What Happens When You Have a Silent Stroke
Updated: Jun. 10, 2021
Silent strokes don't cause any obvious symptoms, but over time, they may lead to permanent brain damage or a major stroke. Here's what you need to know about how to prevent silent strokes.
It’s not that uncommon to have an MRI to check out one health problem, say recurrent headaches, and then find out you have another entirely different problem—evidence of a stroke you never knew you had.
Is it even possible to have a stroke and not know it? Yes, and not only is it possible, it can have long-term consequences. They’re known as silent strokes.
A stroke occurs when the oxygen supply to part of the brain is cut off. The most common cause is a blockage, usually a blood clot, in a blood vessel that normally carries oxygen and nutrients to your brain. However, if a weakened blood vessel bursts, it can also disrupt blood flow and result in the death of brain cells and loss of function. Symptoms include face drooping, slurred speech and arm weakness, according to the American Stroke Association. (If you’re at risk for a stroke, this acronym—FAST—could save your life.) Rapid treatment can help lower the risk of stroke-related brain damage, so stroke symptoms are a medical emergency.
What is a silent stroke?
However, some strokes don’t cause any symptoms at all. In fact, in some cases you wouldn’t even know you had one unless you had an MRI or brain scan for an unrelated reason such as headaches, trouble thinking, or dizziness, says Rohan Arora, MD, director of the Stroke Program at Northwell Health’s Long Island Jewish in Forest Hills, Queens, New York. Still, the effects of these silent strokes, known medically as silent cerebral infarctions, can add up and cause lasting brain damage and erode your memory. Silent strokes also increase your risk for having a major stroke.
Silent strokes are much more common than strokes that cause symptoms. In fact, as many as 11 million Americans may have a silent stroke each year, while 800,000 suffer traditional strokes with symptoms, according to the American Heart Association (AHA) and American Stroke Association. These strokes tend to become more common with age, and about one in four people over age 80 have had one or more, according to the AHA.
“As the name suggests, individuals who have silent strokes do not typically have or present to the doctor with stroke symptoms such as sudden drooping of face, slurred speech, balance problems, or paralysis,” says Dr. Arora. (Do you know the silent signs of stroke in women?)
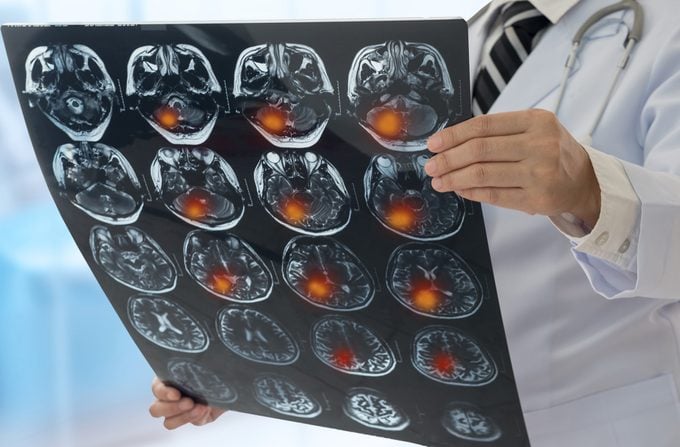
During a silent stroke, a tiny blood clot blocks blood flow to a small area of your brain, and this small area of brain tissue dies permanently, explains Deepak L. Bhatt, MD, MPH, executive director of Interventional Cardiovascular Programs at Brigham and Women’s Hospital in Boston. Silent strokes appear as white spots on an MRI, with the spot the result of blockage-related scar tissue or tiny areas of bleeding.
Even though they are silent, these strokes still have serious and lasting consequences, Dr. Bhatt stresses. “Having silent strokes can lead to damage of the brain, and you can develop vascular dementia over the course of a decade,” he says. (Marked by decline in thinking skills, vascular dementia is the second most common cause of dementia after Alzheimer’s disease, according to the Alzheimer’s Association.) “The brain just doesn’t work as well as it once did.”
Silent strokes typically don’t have signs but sometimes there may be subtle symptoms. “If your right hand is clumsy all of a sudden, it’s probably not lack of sleep,” Dr. Bhatt explains. “If you have trouble moving your mouth or grabbing onto something, it’s never normal. It may go away and you will be relieved, but it could have been a silent stroke.”
Silent strokes are even more subtle than silent heart attacks, he adds. “When someone is told by their doctor they had a silent heart attack, they may look back and recall a time where they felt short of breath for a week.” he says. But “it is unlikely that you will have paralysis of leg or half of face and not realize it.”
Are you at risk for silent strokes?
Silent strokes may be particularly common in older people after they undergo elective surgery, and these strokes double their risk of cognitive decline in the year after the surgery according to a study in the August 2019 issue of the medical journal The Lancet.
In this study, one in 14 people 65 or older who had elective, non-cardiac surgery had a silent stroke as shown on MRI. Participants were followed for one year after their surgery to assess their thinking and memory skills. Those individuals who had a silent stroke after surgery were more likely to experience cognitive decline, major stroke, or another serious event during that time, compared with their counterparts who did not show evidence of a silent stroke on MRI.
What’s the difference between a silent stroke and a TIA?
Silent strokes are not the same as mini-strokes or so-called transient ischemic attacks (TIA), Dr. Bhatt adds. A TIA is a stroke that doesn’t cause lasting disability, because the symptoms are fleeting—but there are symptoms, he says. “Symptoms such as weak arm or leg are gone in 24 hours,” he explains.
A TIA is considered a medical emergency and suggests that a major stroke is imminent. “These are a warning sign that must be heeded,” says Dr. Bhatt. The risks for silent strokes, major strokes, and TIAs are the same, he says, and prevention is the best way to get ahead of any long-term consequences.
“Silent strokes become important if a person has stroke risk factors such as atrial fibrillation (irregular heartbeat), high blood pressure, high blood sugar, or high cholesterol, or family history of stroke and heart attack,” adds Dr. Arora.
Atrial fibrillation (also called AFib or AF) is the most common type of irregular heartbeat and, when untreated, is associated with a fivefold increased risk for stroke, according to the American Stroke Association. “Blood thinners can help people with AFib prevent stroke,” Dr. Bhatt says.”If you are not on blood thinners and have AF, you tend to have more silent strokes from little blood clots forming and killing off small parts of the brain.”
In a 2008 study in the journal Stroke, about 10% of middle-aged people without any stroke symptoms had signs of a silent stroke on MRI, and the risk of having one was more than double in those who had atrial fibrillation.
The symptoms of atrial fibrillation include a fluttering sensation of the heart and a heartbeat that is too fast or uneven, chest pain, dizziness, shortness of breath, and feeling light headed or fatigued. (Although the symptoms may not be obvious or could be mistaken for other problems.) Afib is more common in people over 60 as well as those with sleep apnea, hyperthyroidism, diabetes, high blood pressure, asthma, or heart disease, or who are binge drinking.
How are silent strokes treated?
While the damage due to silent strokes can’t be reversed, rehabilitation therapy can help people improve memory and speech. If you’ve had a silent stroke, it’s important to take steps to prevent future strokes of any type, silent or otherwise. That would include quitting smoking, and getting blood sugar, high cholesterol, and high blood pressure under control with diet, exercise, and medication, if necessary.
High blood pressure is a major risk factor for stroke.”When high blood pressure isn’t well controlled, it is associated with more silent strokes and that damage can add up with time,” Dr. Bhatt says. (Following these guidelines for your diet could cut your risk of stroke by 27 percent.)
Diabetes and high levels of cholesterol are also important stroke risk factors, he says. Eating a healthy diet, getting regular physical activity, maintaining a normal weight, and not smoking or drinking excessive amounts of alcohol all work together to control and lower risk for stroke. What’s more, talk to your doctor to make sure you are doing all you can to treat atrial fibrillation.


















