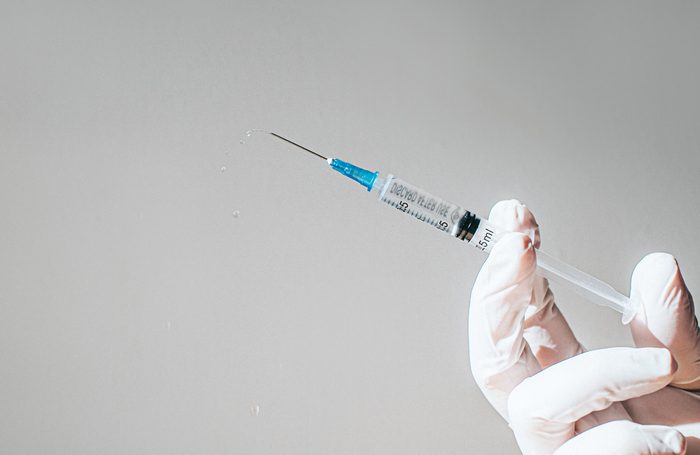
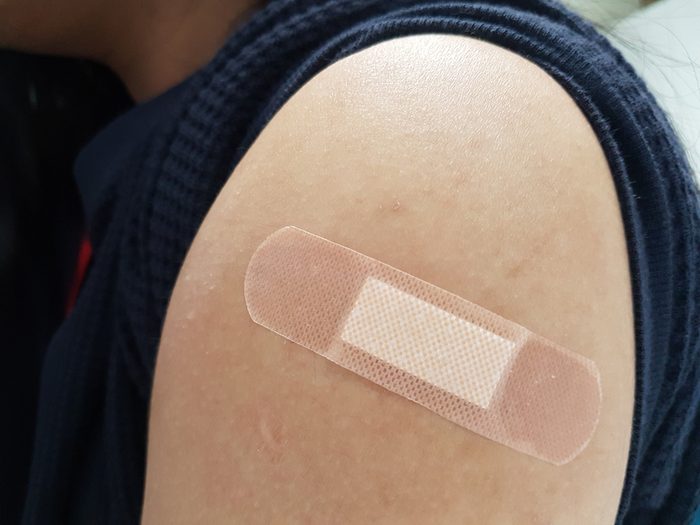
Important vaccine facts
Efforts to develop a vaccine for Covid-19 are happening at warp speed, says Kathyrn M. Edwards, MD, a spokesperson for the Infectious Diseases Society of America (IDSA). There are currently more than 100 vaccine candidates in some stage of development, eight of them already in clinical trials. (Read about this family physician’s Covid-19 vaccine trial experience.)
There are still a lot of questions about potential vaccines, such as when they will be released (if we’re supremely lucky maybe later in 2020, or even in a year or more) or even if antibodies that are normally what make vaccines effective will be protective against this new virus and for how long, says Richard Kuhn, PhD, The Trent and Judith Anderson Distinguished Professor in Science at Purdue University.
While we’re waiting for those answers, don’t forget that there are dozens of effective vaccines for other diseases already out there. And for those, we do have a lot of answers.

Good hygiene can’t replace vaccines
Increased medical care, better nutrition, and cleaner and less crowded living conditions have certainly had an impact on the spread and treatment of infectious diseases over the years. But the World Health Organization (WHO) reports that vaccines have played an even more important role in the drastic reduction of disease. If there’s no vaccine for a disease (as is the case with Covid-19), then all we have is hygiene, says Dr. Edwards, who is also a professor of pediatrics at Vanderbilt University in Nashville. And for some highly contagious diseases like measles, hygiene may not be enough. While Covid-19 may infect three to four people, measles can infect 15 to 20. That said, you still need to focus on hygiene.
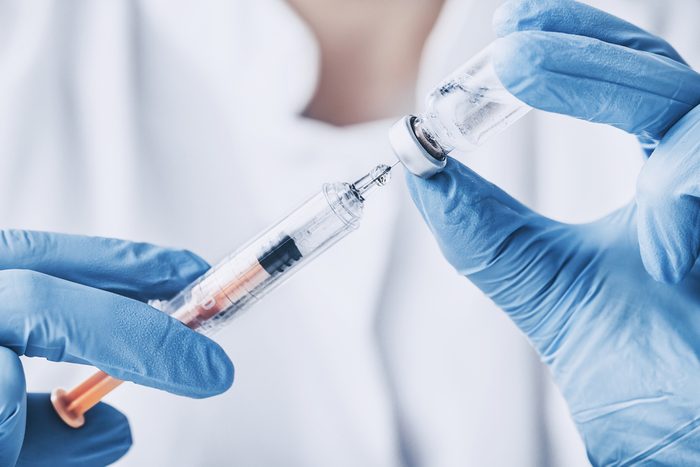
You still need the vaccine even if you haven’t heard of the disease
As an example of this, the WHO points to Haemophilus influenzae type b (Hib), a type of bacteria that can cause brain and blood infections, including meningitis. Due to the vaccine, the disease is now mostly a footnote. (Before the vaccine, 20,000 young children got the infection and 1,000 died each year; now, cases have dropped to about 50 per year, according to the Centers for Disease Control and Prevention.) Numerous other viruses that most of us are thankfully unaware of could come back with potentially deadly results if we stopped vaccinating, the agency says. (By the way, Hib is not related to the influenza virus.)

Even if you’ve been vaccinated, you can still get sick
“No vaccine is 100 percent effective,” says Dr. Edwards, although some (like measles) come very close. In a major outbreak, says WHO, immunized people can become infected, though not at the same rate as people who have not been immunized.
The other issue is that up to 5 percent of people may not respond to a vaccine, according to the CDC. That’s why some vaccinations require additional boosters. It’s also possible that the vaccine and the infection crossed paths so to speak. In other words, some people are infected just before or after receiving the vaccine and develop symptoms because the immune response hasn’t had time to kick in. (It can take the body a couple of weeks to react to the vaccine and create protective antibodies.)
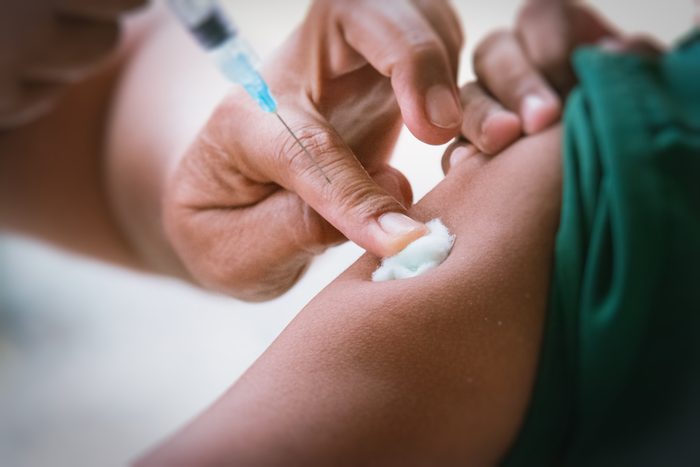
Vaccines don’t cause disease
Even though vaccines contain bits and pieces of the same bacteria or viruses that causes disease, the vaccine itself is not going to make you sick from the disease. That’s because vaccines are usually made from inactivated (killed) organisms or “live attenuated,” meaning the germ is greatly weakened. Live attenuated vaccines give you really robust protection but they can be dangerous to some people, such as those with compromised immune systems. Inactivated vaccines don’t give you as much protection, meaning you may need more than one dose. They are, however, safer for more people. There are two other vaccine types as well. Subunit, recombinant, polysaccharide, and conjugate vaccines use particles of an organism while toxoid vaccines use a toxic substance produced by the germ—not a version of the germ itself. (Check out the reasons why parents—not just children—need to be up-to-date on their vaccines.)
Sometimes you need more than one shot
The CDC reports that when people get a second shot (or a booster) of a vaccine, the protection may reach nearly 100 percent effectiveness. Some vaccines require a third shot. In adults, the Td (tetanus, diphtheria) vaccine requires a booster every 10 years. Other adult vaccines that require extra doses are hepatitis A (two doses given six to 18 months apart), hepatitis B (three doses over six months), and human papillomavirus (also three doses over six months). The recommended vaccination schedule for children is complicated and several vaccines require multiple doses including DTaP (diphtheria, tetanus, and pertussis), polio, MMR (measles, mumps, rubella) and chickenpox. Of course, the flu vaccine needs to be repeated annually.
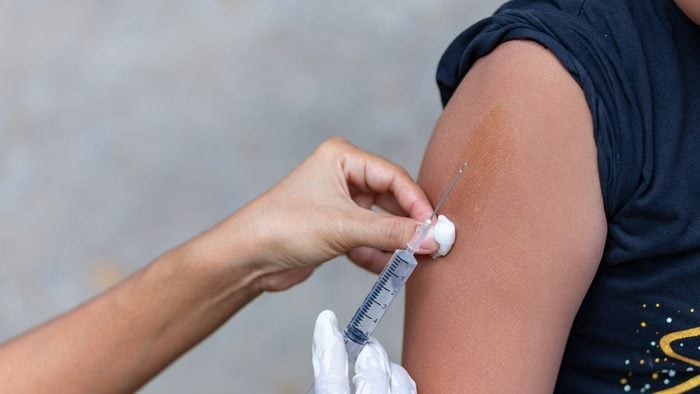
Some vaccines contain preservatives
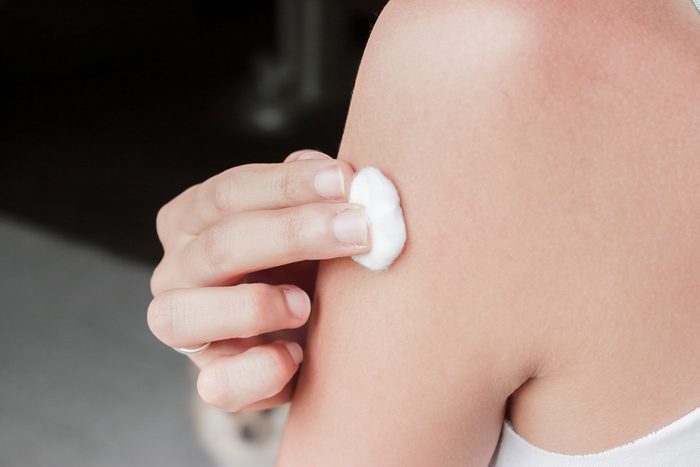
Vaccine-preventable diseases like measles, mumps, and even HPV can be fatal, but the vaccines that prevent the disease are not. The CDC notes that only some vaccines contain trace amounts of preservatives and other ingredients like formaldehyde, mercury, and aluminum—and in those cases, the levels are not nearly enough to be harmful. They also report that the human body is exposed to higher levels of these chemicals from the environment than you would get from vaccines. Some vaccines may give you a minor illness. “The only vaccines that would be capable of giving the disease are live vaccines, an example is the measles vaccine,” says Dr. Edwards. “Some people seven to 10 days after the vaccine get a fever and rash. That’s weakened measles.” Healthy people shouldn’t have any problem with this, although immunocompromised people need to talk to their healthcare provider.

You don’t have to worry about the mercury in vaccines
Some vaccines do use a preservative called thimerosal, which contains ethylmercury, but there’s been no evidence showing it can cause harm in the low doses you’d find in an immunization. The compound is used as a preservative in multi-dose vaccines to prevent them from getting contaminated, says Dr. Edwards. The name can be easily confused with methylmercury, which is not found in vaccines. Methylmercury can damage the central nervous system—but again, it’s not found in vaccines. It is, however, found in fish from air pollution that settles in water. The body gets rid of ethylmercury way faster than methylmercury, making it less likely to do damage . Even so, ethylmercury was taken out of childhood vaccines in 2001 to ease any concerns.

You’re helping everyone when you get vaccinated
Vaccinations contribute to a healthier community. People with weakened immune systems—and those for whom a vaccine may not be as effective or even recommended—can be in danger if they run into someone who is sick. When everyone keeps up with vaccinations, we prevent outbreaks that could have numerous fatalities. “We know that if we have a population that is vaccinated, then it reduces the ability of the virus to spread,” says Dr. Edwards. “If everyone around us vaccinated, we can really cut down remarkably the spread of the infection.” That’s called herd immunity. Here’s what you should know about Covid-19 herd immunity.

There is no such thing as “hot lots”
Some people believe that certain batches of vaccines—known as “hot lots”—are responsible for more side effects than normal batches of vaccines. There was a suggestion that certain lots were linked with more fever than others in the 1990s, says Dr. Edwards. But since then, “there doesn’t seem to have been any particular association.” Adverse events and possible side effects are reported to the CDC after every vaccine in introduced, but this doesn’t mean that the virus caused them, the WHO points out. And because lots vary in size from a few hundred thousand to several millions, it’s like comparing apples to oranges. Larger lots will be associated with more adverse effects because more people get them.
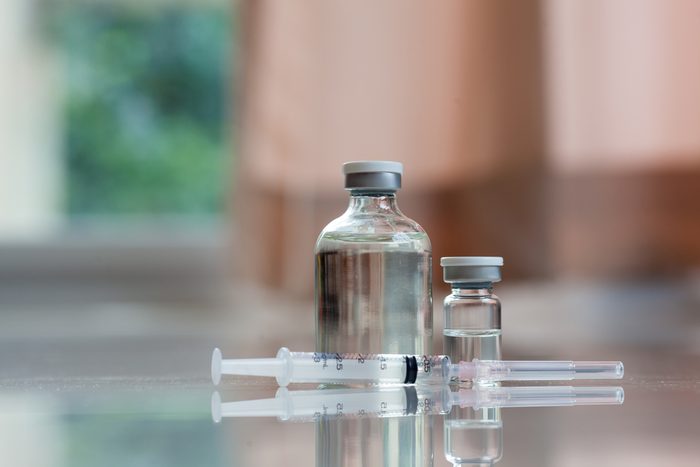
You still need vaccines—even for rare diseases
William Schaffner, MD, an infectious diseases expert at Vanderbilt University School of Medicine, suggests that a person living in rural Maine, for example, may wonder why they should vaccinate a child for a disease that only exists in Afghanistan or Pakistan. “Someday your child will travel. We know that when we have a substantial amount of parents holding back from getting their children immunized, diseases can be reimported into the United States. ” In other words, they can be at risk even if they don’t travel. He points to the 2014-2015 measles outbreak in California’s Disneyland as evidence that children can also enter the United States from other countries and spread diseases to unvaccinated Americans.
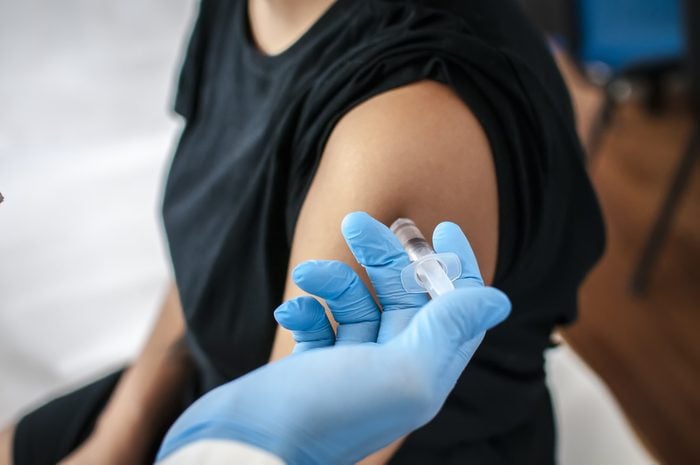
Vaccine combination shots won’t overload the immune system
The WHO assures people that combo vaccines as well as giving more than one vaccine at the same time for different diseases have no adverse health effects. The organization notes that vaccines don’t burden a child’s immune system more than common illnesses like strep throat and upper respiratory infections. Even new foods introduce new bacteria into the body, says the WHO. There have been plenty of studies on the issue and none have found an increased risk of problems. Indeed, there are advantages to combining vaccines in one injection, namely fewer visits to the doctor and fewer jabs.
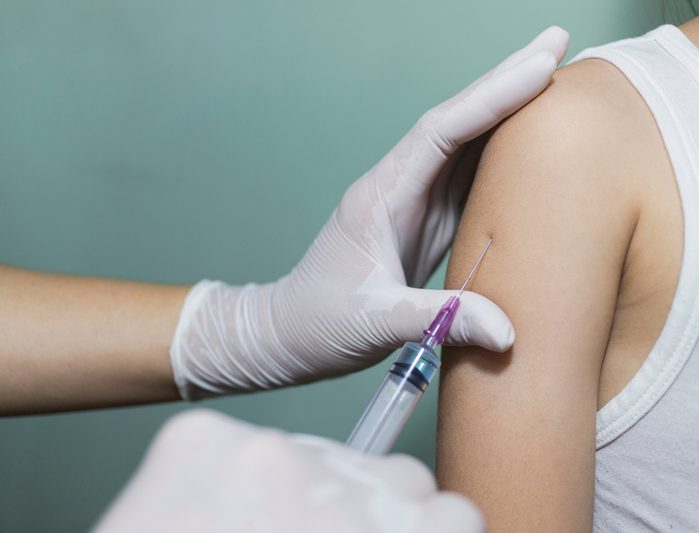
Kids don’t see the HPV vaccine as a green light for unprotected sex
The human papillomavirus vaccine protects against the human papillomavirus (HPV), the most common sexually transmitted disease in the U.S. Some types of HPV can cause genital warts and others are the main cause of cervical and other cancers. (There are more than 100 types of HPV, some more dangerous than others.) Vaccines can protect against most of the cancer-causing HPV types. Some parents are resistant to the idea of their children getting the shots because they worry their kids will see it as permission to have sex—unprotected. Several studies have busted this myth, including one published in 2019. The researchers found no link between sexual behavior and getting the HPV vaccine: Participants did not start having sex earlier because of the vaccine, nor did they take on more sexual partners. Kids are smarter than that, says Dr. Schaffner. (The vaccine is recommended for adolescent boys and girls, and can be given as early as age nine, because it’s thought to be most effective if someone has not yet been exposed to HPV.)
Boys need the HPV vaccine, too
The HPV vaccine is not only for girls, confirms Dr. Schaffner. “The vaccine was originally touted as preventing cancer of the cervix, and while that is wonderfully true, it also prevents head, neck, and anal cancers,” which are not gender-specific, he says. The vaccine can also prevent vaginal cancer. The CDC recommends that both boys and girls get the HPV vaccine around age 11 or 12. The vaccine requires two doses, the second six months to a year after the first. Although kids can get the vaccine as young as nine, if you defer too long, three doses may be needed. (Here are HPV myths you shouldn’t believe.)

The HPV vaccine works really well
The HPV vaccine was first recommended in 2006. In the decade after it was introduced, HPV infections dropped by 86 percent in females aged 14 to 19 and 71 percent among women in their early 20s. What’s more, fewer cases of genital warts and precancerous cervical lesions have been noted in other countries. Protection from the vaccine also seems to be long-lasting with studies so far going out to 10 years. Even with the vaccine, experts still recommend that women get screened for cervical cancer starting at age 21 until they’re 65. The vaccine is also safe, with few side effects noted even though 120 million doses have been given.
You can still get the vaccine even if you’ve had HPV
While women who contract the virus before getting vaccinated won’t gain all the benefits that women who’ve never had it get, it’s still worth signing up, says Dr. Schaffner. That’s because the vaccine covers nine different strains of HPV and it’s not likely you’ve had all the strains, according to the Children’s Hospital of Philadelphia. Once you’ve been immunized, you’re not likely to pass on the strains you’ve been protected against, but you can pass on strains that aren’t included in the vaccine. Individuals under the age of 15 should get two doses of the vaccine while those who are older should get three doses.

The HPV vaccine won’t cause infertility
But having cervical cancer, which the HPV vaccine prevents, can cause infertility, says the CDC. That’s because treatment usually involves removing your cervix and uterus along with chemotherapy and/or radiation. Millions and millions of doses of available HPV vaccines have been given since 2006 and there’s been no evidence that this vaccine causes primary ovarian insufficiency (POI) or “premature menopause.” The primary cause of infertility is not ovulating, says the National Institute of Child Health and Human Development but this is usually because of age, polycystic ovary syndrome, hormonal conditions, lifestyle factors like nutrition and weight, as well as POI. Experts don’t completely understand what drives POI.

Natural immunity is not better than vaccine-acquired immunity
Some people believe that the immunity gained through getting a virus is better than a vaccination. “That’s a disturbing notion,” says Dr. Schaffner, “and it must come from people who have had no exposure to diseases that can be prevented through vaccination. Their assumption must be that the disease is trivial.” Schaffner says that this dangerous idea has become more common because we have eliminated so many diseases with vaccines that people don’t have experience with how traumatic and fatal viruses can be. Even though immunity from a disease may be higher than a vaccine (in measles, it is 100 percent versus 98-99 percent, respectively), you still have to get the disease, says Dr. Edwards. And that’s way worse than the vaccine.
Measles—preventable through vaccination—is still an issue
Before the measles vaccine became available in 1963, three to four million people in the U.S. were infected each year, says the CDC. This resulted in 400 to 500 deaths and 48,000 hospitalizations. In 2000, the disease was declared eliminated—proof of the success of the vaccine. Unfortunately, measles has made a comeback in the U.S., largely among unvaccinated people. People traveling from other parts of the world can also import the disease. In 2019, there were 1,282 cases of measles in the U.S., up from 375 the year before. (And in 2010, 2012, and 2016 there were under 100 cases each year.)
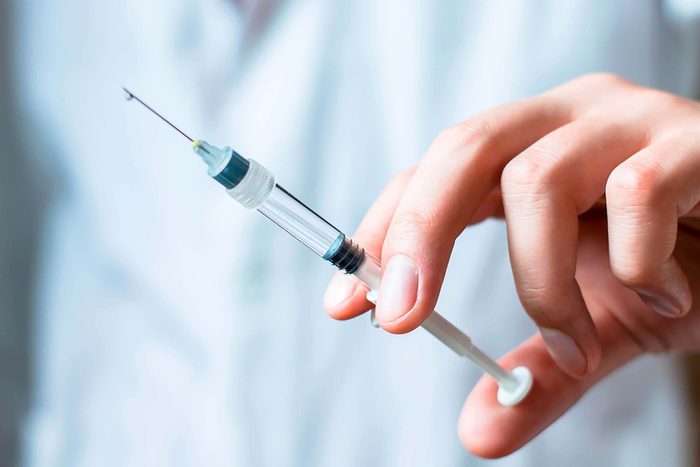
Flu shots won’t give you the flu
Low-grade fever, headaches, and muscle aches are common side effects of the influenza vaccine. But this vaccine cannot give you the actual flu, reassures the CDC. That’s because flu shots are made with inactivated (killed) viruses, says Dr. Kuhn. “I hear some people say ‘I got the flu shot and I got the flu’ but the flu vaccine is by definition incapable of causing disease,” he adds. “It may be you didn’t get it in time or didn’t mount a good immune response.” This is really important to understand when a Covid-19 vaccine is finally developed. It will likely be an inactivated vaccine or a subunit which contains no infectious material. “It will have no chance of inducing illness,” says Dr. Kuhn. (Make sure not to make one of these common flu shot mistakes.)
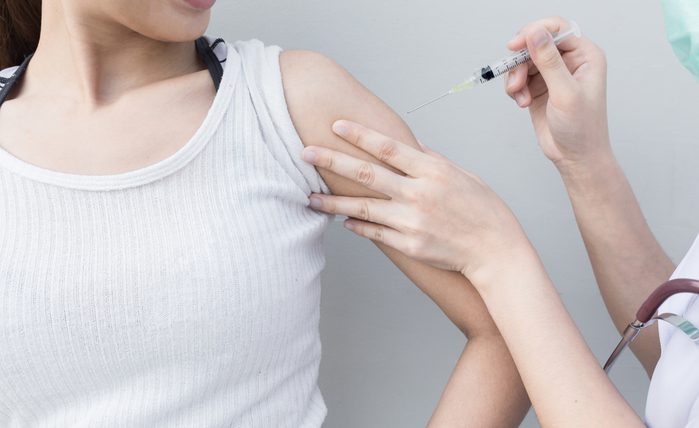
The flu shot isn’t a sure bet
It’s possible, though less likely, to still contract the flu despite getting the vaccine. Sometimes the actual bugs circulating are different from the ones scientists predicted and that are included in the annual vaccine. Other times, a person’s immune system simply did not respond to the vaccine as well as it should. Several factors can affect immune response to the annual shot, including genetic make-up, any preexisting immunity and underlying health conditions, according to an article in Human Vaccines & Immunotherapeutics. Age is also a factor, with older people responding less well to standard-dose vaccines. Then there’s the vaccination itself, which varies in effectiveness from year to year. On the other hand, we know that even if you do get sick, it should be less severe, says Dr. Edwards. Flu shots can reduce hospitalizations and deaths, even if they don’t prevent every symptom.
Don’t skip the flu shot just because you’re healthy
It’s true that children ages 6 months to 4 years, people 65 or older, pregnant women, and anyone with a disease that compromises their immune system should definitely get a flu shot. But just because you don’t fall into one of those categories doesn’t mean you should skip vaccination. Flu shots are now recommended for everyone 6 months or older, every year, except in certain rare cases. “Herd immunity is an important concept,” says Dr. Schaffner. “A vaccine not only protects the person vaccinated, but it also protects the community.” That includes those who can’t get flu shots, including babies under six months of age and those with severe, life threatening allergies to vaccine components.
The flu vaccine won’t make you vulnerable to other viral illnesses
Although there have been reports that the flu vaccine might increase a person’s risk of contracting other respiratory illnesses, this is not the case. “The current flu vaccine is an inactivated influenza virus that is incapable of causing any flu-like disease since there is no live virus involved,” says Dr. Kuhn. Of course, plenty of other viruses are circulating at the same time as the flu so you do have a chance of contracting other illnesses, just not because of the flu vaccine.

You’d be surprised how late you can still get the flu vaccine
It’s ideal to get your flu shot as soon as possible after its early fall release; the CDC recommends getting it by the end of October. (In North America, flu season generally starts in October and peaks from December to February, although it can last until May.) But the group also stresses that a flu vaccine in November and even late in the season can be beneficial. Although it may not ever be too late to get the flu vaccine, it can be too early. The CDC states that getting the vaccine in July and August (if it’s available) may not provide protection throughout the season, especially among older adults. Flu shots typically take about two weeks to stimulate the antibodies in the body that protect you from the infection.

Pregnant women don’t need a doctor’s approval to get the flu vaccine
The CDC encourages women who are pregnant or will be pregnant in flu season to get a flu shot, especially because they are more susceptible to complications, severe reactions, and hospitalizations from the flu. Women concerned about trace amounts of the mercury-based preservative thimerosal can take heed: Thimerosal-free flu vaccines are available at many doctor’s offices and pharmacies. “The flu shot is fine for pregnant women because it doesn’t contain live virus,” says Dr. Kuhn.

Don’t skip the flu shot because you think you’ve already had the flu
Just like pregnant women, anyone over the age of 6 months is still encouraged by health officials to get their flu shot. Ideally, you should get the shot by the end of October, says the CDC. That gives it a little time (about two weeks) to take effect before flu season really kicks in. But it may be worth your while to get a shot even if you think you’ve already been infected. Every year several strains of flu virus circulate. “Sometimes at the beginning of the year, we will have one strain then, as the year goes on, another comes on,” says Dr. Edwards. “If you haven’t been vaccinated it can still be recommended because another strain may come later.” Flu vaccines protect against more than one strain of the influenza virus.
Only certain people should avoid vaccines
The CDC and the FDA warn that anyone who is severely allergic to vaccines should skip immunization. However, if you have an egg allergy, it’s still recommended that you get a flu shot, according to the CDC. There are also groups of people who should avoid live vaccines. “If it’s a live vaccine and you’re immunocompromised, you should not get the vaccine,” says Dr. Kuhn. “Most live viruses are not advocated for women who are pregnant.” Examples of live vaccines are measles/mumps/rubella (MMR), smallpox and chickenpox. Fortunately, most vaccine reactions are mild, such as redness around the injection site. Only rarely do you see serious reactions.

The flu vaccine won’t prevent the stomach flu
Illnesses that cause vomiting and diarrhea are often referred to as the “stomach flu,” but this is a misconception, according to the CDC. Any number of bacteria, parasites, and even viruses can cause severe GI symptoms, but rarely the influenza virus. The flu is a respiratory illness so the primary flu symptoms are fever, chills, aches, fatigue, sore throat, and runny nose. The so-called stomach flu is actually called gastroenteritis. The most common causes are norovirus (infamous on cruise ships) and rotavirus. They are also notoriously easy to pick up and they spread rapidly in close quarters. (There is no vaccine for norovirus, although there is a rotavirus vaccine for infants.)
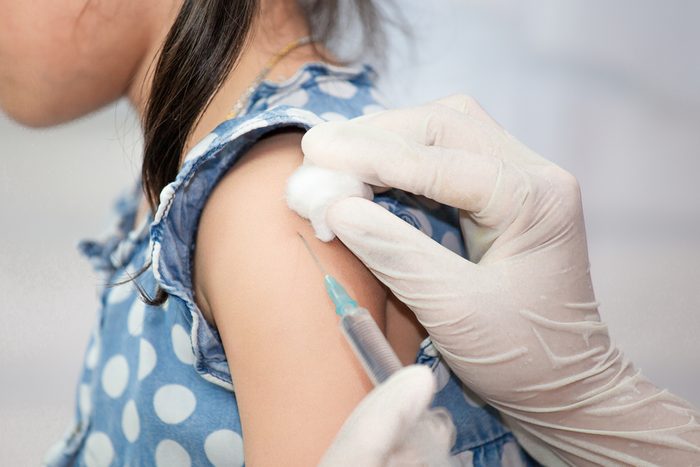
Vaccines definitely do not cause autism
One of the leading arguments of the anti-vaccination movement is that vaccines—particularly the measles vaccine—causes autism in children. “This has been totally discredited,” says Dr. Schaffner. According to the CDC, there is no link between vaccines and autism; their experts point to nine separate CDC-funded or conducted studies since 2003 that have disproven the supposed connection between the preservative called thimerosal—found in trace amounts in some vaccines—and autism. The vaccines for measles, mumps, and rubella have all been cleared of any connection to the condition. Even Autism Speaks, one of the leading autism advocacy organizations in the United States, takes this stance.
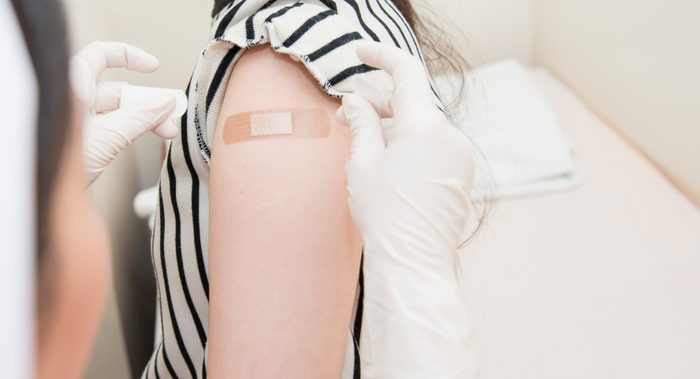
Adults need vaccines, too
Regardless of age, almost everyone needs vaccines—and that includes adults, says the CDC. Some childhood vaccines can wear off; also, American adults who might be exposed to new viruses via foreign travel are strongly advised to get vaccinated. Although travel is not advisable right now during the Covid-19 pandemic, when you do decide to travel again, seek your doctor’s opinion on what vaccines are right for you. This will depend on where you go. However, vaccines are your best protection against dozens of diseases, such as hepatitis A and B, chickenpox, measles, rubella, and tetanus. Here’s a guide to adult vaccines.
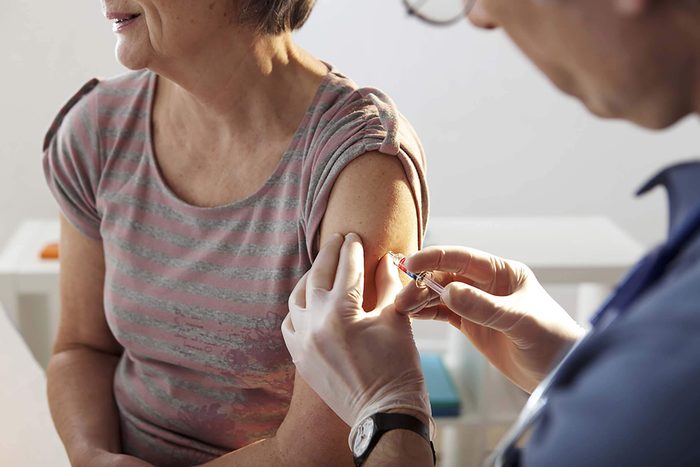
If you’re over 50, be sure to get this vaccine
According to a CDC advisory committee, people over the age of 50 should add the shingles vaccination to their health to-do list. Shingrix is the preferred vaccine, although another one (Zostavax) is also available. Approximately one in three people in the United States will develop the infection at some point, which is a reactivation of the same virus that causes chickenpox. Symptoms for shingles include severe pain, itching and tingling preceding a rash, which usually occurs as one band around one side of the body. You may also have a fever, headache and chills. Make sure you know these other symptoms of shingles as well.
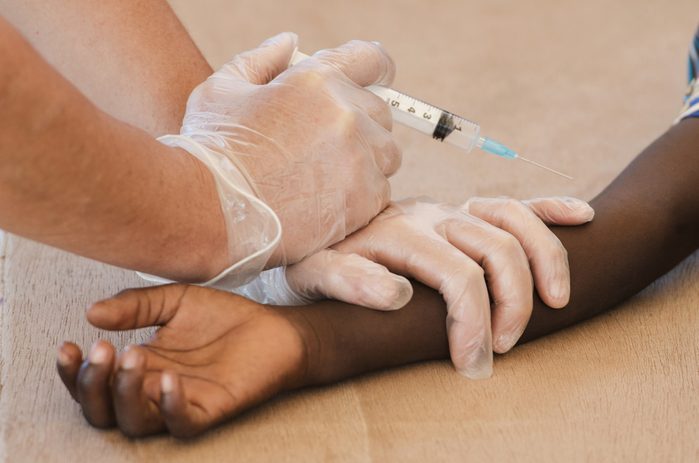
Vaccines are more effective than people realize
No vaccine is foolproof, but the FDA’s regulations stipulate that the shot be safe and effective: The agency won’t approve a vaccine that doesn’t work well. “Depending on which vaccine we’re talking about there is a range of effectiveness,” says Dr. Edwards. “The most effective is probably measles which has 95 percent effectiveness, 98 to 99 percent effectiveness after the second dose.” Chickenpox is over 90 percent and DTP about 85 percent, she adds. Even the flu vaccine—which is developed each year based on projections of which viruses will be circulating—is anywhere from 50 to 75 percent effective, says Dr. Edward.
Don’t listen to people who say vaccines are a scam
“This is a dangerous belief,” says Dr. Schaffner. One reason measles was almost eradicated in the Western hemisphere is that nearly everyone was vaccinated, he says. “I find that skeptical people have a hard time explaining this phenomenon.” Misconceptions about vaccines include the fact that infectious diseases were on the wane even before vaccines came along and that you don’t need to get vaccinated because infectious diseases are declining in the U.S. The truth is that rates of these illnesses are declining precisely because we have had successful vaccinations. Make sure you’re aware of these common myths about vaccines.
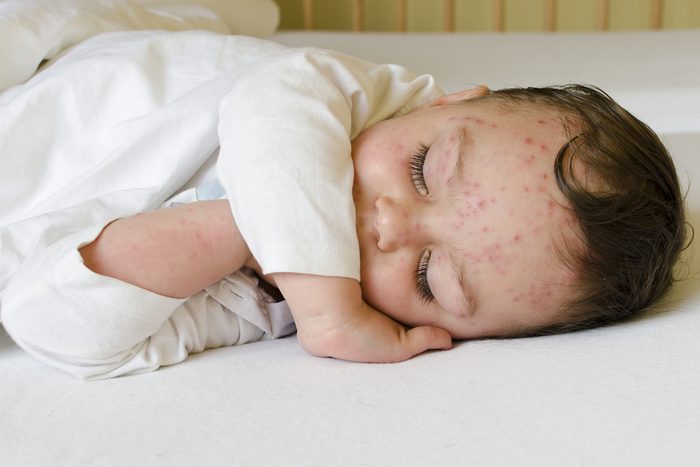
Don’t forget about the chickenpox vaccine
Although most adults feel like chickenpox wasn’t that bad if they got it as a child, it still makes sense to get your children vaccinated. Why? In addition to the irritating and painful blisters and sores (pox), it can cause pneumonia and brain damage. According to the CDC, before the vaccine was available, the varicella virus was responsible for about four million cases, 11,000 hospitalizations and more than 100 deaths each year. All children should get 2 doses of chickenpox vaccine starting at age one. Some teens and adults may also need this vaccine if they didn’t get two doses of the vaccine or chickenpox disease when they were younger.
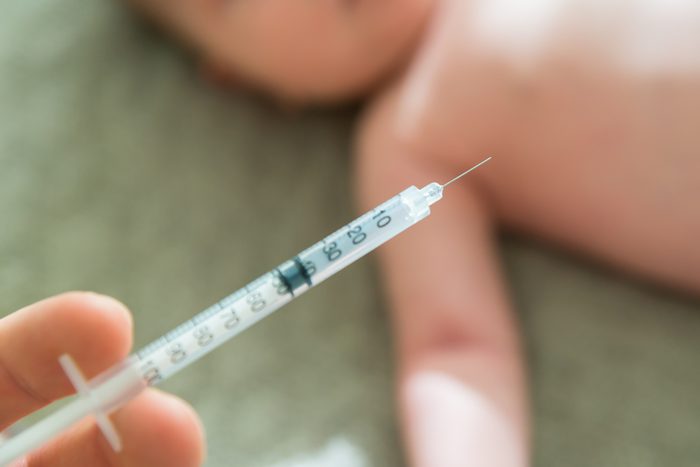
Don’t wait to vaccinate infants
A newborn’s immune system is still developing, says the CDC. Which is why it’s important that your child get vaccines on the recommended schedule. Delaying means increasing the risk of infection. Recommendations are based on what science says about how young immune systems react to antigens at particular times. Vaccinating early and giving your child’s immune system time to ramp up means a smaller window of time they might be exposed to an infectious illness. Not to mention the risk that if your child does get sick, he or she will pass on a potentially dangerous illness to someone else.
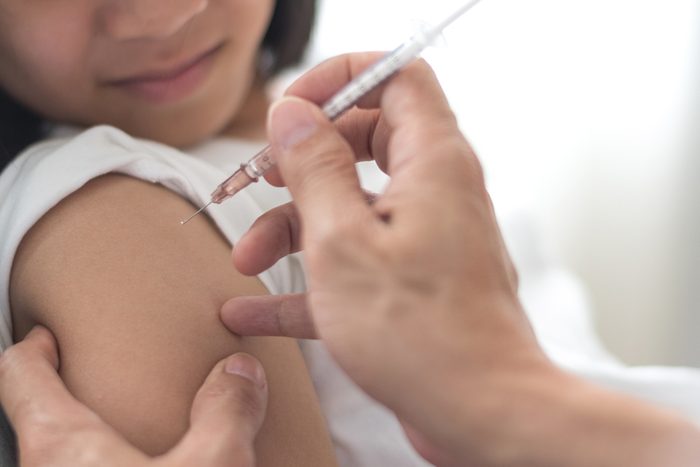
You’re not more likely to get sick from the vaccine than the virus
Vaccines come from either killed or weakened germs, or just specific proteins from them, which won’t cause serious illness. To help the body recognize and fight the disease in the future, the immune system will have the same response it would to a real infection, says Eileen Yamada, MD, a public health medical officer with the California Department of Public Health Immunization Branch. Usually the most you’ll get are minor symptoms like a brief fever that’s way less dangerous than anything you’d pick up from your environment. Vaccines also don’t cause long-term health complications, as decades of actually giving vaccines have demonstrated.

The FDA is a vaccine watchdog
The FDA states that vaccines—like all products it regulates—”undergo a rigorous review of laboratory and clinical data to ensure the safety, efficacy, purity, and potency.” “The FDA has really vaccines to ones that are super safe so they don’t allow much in the way of side effects,” says Dr. Kuhn. “The good side of that is you’ve got something that shouldn’t make you in any way sick.” And even if you get a small rash or pain, it’s a good thing, Dr. Kuhn adds, “because it reflects you’re getting a strong immune response. Once vaccines have been approved and have been out for a few years usually very safe.”

The FDA’s vaccine-monitoring efforts are ongoing
The CDC and the FDA maintain a Vaccine Adverse Event Reporting System (VAERS) which acts as an “early warning system” in case problems arise. “People need to understand that there is careful recording after each dose is administered,” Dr. Edwards explains. “When doctors and nurses give vaccines, they are required to record the lot, the kind of vaccine and where it was given so if there were any clusters of reactions those could be looked at.” There’s also a large system of HMOs (health maintenance organizations) that look for reactions after vaccines, he says. “We take this very, very seriously,” says Dr. Edwards.
Vaccines are working wonders
According to the WHO, two to three million lives are saved every year thanks to vaccines. Now the world is hoping a vaccine (or vaccines) will work wonders in preventing and controlling Covid-19. “If there is an effective vaccine that protects individuals, then vaccination of an individual will protect them from coming down with the disease that is caused by Covid-19,” says Dr. Kuhn. ‘Death will no longer be a potential outcome of infection and we will be able to get back to our regular routines.”
Most parents are vaccinating their children
Despite periodic outbreaks of vaccine-preventable diseases, media reports of parents refusing to vaccinate their children and fears about vaccine safety, a recent CDC report shows that vaccination rates are still high in the United States, with more than 90 percent of children being vaccinated against measles, mumps, and rubella (MMR), poliovirus, hepatitis B, and varicella. The authors of the report postulated that lack of access to healthcare and vaccines, including the Vaccines for Children (VFC) program, accounted for some of the gap. But there’s another reason. “We’ve done such a good job of eliminating most of infectious disease that people no longer fear them,” says Dr. Edwards. “We’re fickle people. Out of sight and out of mind.”
Vaccines may one day make it possible to not need vaccines
Vaccines may one day make it possible to not need vaccines
“When we eradicated smallpox we stopped vaccinating against smallpox,” explains Dr. Schaffner. When mass vaccination programs work the way they’re supposed to—everyone gets the shot—it can lead to the eradication of a disease. Before the vaccine, smallpox killed three out of every 10 people, according to the CDC. The last case of naturally acquired smallpox came and went in 1977: A hospital cook in Somalia who shared a vehicle with two smallpox patients. He recovered. North America saw its last case of smallpox in 1952, Europe in 1953, South America in 1971, Asia in 1975 and, finally, Africa in 1977. Next, find out the 55 rampant health myths that need to die.