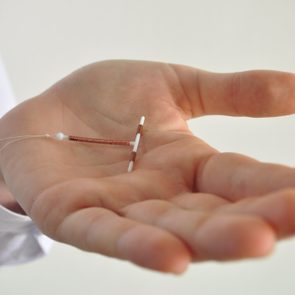
Can a Menstrual Cup Displace an IUD? A Doctor Says It’s a “Growing” Concern
Updated: Jul. 06, 2022
Some advances in women's health are brilliantly streamlining our lives...but one woman's story brings a hardly discussed—though increasingly common—issue into the spotlight.
By Johanna B., as told to Charlotte Hilton Andersen
Menstrual cups and IUDs don’t always make the perfect pair

My menstrual cup was my holy grail period product. It’s a cup that’s about the size of a shot glass, made out of flexible medical-grade silicone, that makes a tight seal in the vaginal canal and is designed to catch about an ounce of endometrium—that’s the blood cells and tissue the body releases during menstruation—per wear. Its capacity meant I only had to change it twice a day, washing the cup before I reinserted it. After years of using non-eco-friendly tampons and bulky, uncomfortable pads to deal with my periods, the simplicity of a menstrual cup was mind-blowing. (That’s not to mention all the money I saved because it’s reusable, potentially for years.)
Sure, there was a bit of a learning curve figuring out how to insert and remove it—not going to lie, it took a few glasses of wine and an hour to remove it the first time. But after a bit of practice, it was a breeze to use and a game-changer for my routine. I’m a mom of three and a nurse who’s very physically active. Now I could swim and bike and hit the gym without worrying about leaks or changing a tampon midway through.
I told every female friend I had about it. I handed them out as birthday gifts and stocking stuffers. My only regret was not getting one sooner.
Unfortunately, there was something I didn’t know. My other favorite feminine product was a copper intrauterine device (IUD) that I used for birth control. My doctor inserted it into my cervix, where it could sit safely to prevent pregnancy for up to 10 years.
I loved my IUD. For one thing, some research has shown that IUDs may reduce the risk of cervical cancer. But I also loved how easy it made my birth control routine: I didn’t have to do any maintenance, remember schedules or doses, or deal with artificial hormones. My body hates the hormones in birth control pills.
The Best Menstrual Cups for More Affordable, Sustainable (and Cleaner!) Periods
Pregnancy panic
My husband, our three kids, and I had been cooped up for months during the pandemic when in December of 2021, my in-laws surprised us by taking the kids to see a holiday show. With a free afternoon, my husband gave me a look suggesting we should take advantage of the empty house. It was during my cycle so I stepped into the bathroom to remove my menstrual cup, grasping the “stem” on the bottom and giving it a gentle pull. For a moment, I felt a painful spasm—but the cup came out normally, so I thought nothing of it and slipped into the bedroom.
As it was getting interesting, my husband suddenly jerked back and said something had “pricked” him down there. I’d heard that some men could feel the “strings” that are in place to facilitate a doctor’s removal of an IUD, so I cautiously wondered if maybe that’s what it was. I readjusted my body, and invited him to try again slowly. He did…and this time, I could feel that something was definitely wrong.
When I examined, I could actually feel something poking out of my cervix. As I felt around, trying to figure out what was happening, the IUD slowly slid the rest of the way out.
Immediate panic set in. Besides hoping neither of us had been injured, we definitely did not want to have another baby.
I called the emergency line to my doctor’s office, and she called me back right away. She said as long as I wasn’t in serious pain, had uncontrolled bleeding, or felt like the IUD was “stuck” in a dislodged position, IUD expulsion wasn’t an emergency. But, she said, it was possible that my menstrual cup had dislodged my IUD. Her theory was that either I hadn’t properly broken the suction before pulling on the cup, or I’d accidentally pinched the strings along with pinching the cup—either of which could partially or fully dislodge an IUD.
A women’s health doctor calls this “a growing problem”
Could I end up pregnant from my menstrual cup dislodging my IUD? “It’s certainly possible,” my doctor replied ominously.
After my experience, I was deeply unsettled. I chatted with some of the women I’d raved about my cup with and learned that I wasn’t the only one who’d been combining these two devices. “With more women choosing intrauterine devices (IUDs) for birth control, there has been a growing problem of IUDs being accidentally dislodged,” says Christine Greves, MD, an OB/GYN at Orlando Health. Menstrual cups aren’t the only reason IUDs can get moved out of place or expelled from the cervix, including improper insertion, uterine fibroids, a tilted uterus, abnormalities in the cervix, and trauma to the cervix or vagina, she says—adding that menstrual cups should be added to that list.
How common is IUD expulsion? Research suggests it’s more common than most of us realize. Women who used a menstrual cup saw four times an increased risk of IUD displacement, according to a 2020 study published in Obstetrics & Gynecology. Researchers found that after two years, about 17 percent of cup users experienced IUD expulsion, compared with just five percent of non-users.
Ways to help prevent your IUD from being displaced
This is something that warrants more discussion. Dr. Greves suggests women’s health professionals should teach IUD users how to regularly check their device’s placement, and to watch out for possible signs that it may have become displaced. Symptoms of IUD displacement or expulsion can include sharp or dull pain deep inside the vagina, cramping, unusual bleeding, an inability to feel the strings with your fingers, or a feeling that something is in your vagina. However, Dr. Greves reports, some women may experience no symptoms at all.
A close call
Thankfully, I didn’t get pregnant…but for a few weeks, I was worried. (My husband and I have sometimes joked that all we had to do was wash our underwear together, and we’d find ourselves expecting.) The incident spurred us to have a serious talk about family planning, and my doctor recommended not using the menstrual cup and IUD together in the future. I didn’t want to give up the cup—nor did I want to go back on the pill—so two months after our scare, my husband went in for a vasectomy.
Sign up for The Healthy newsletter for important conversations about sexual health, relationships, and much more. Also follow us on Facebook and Instagram—and, keep reading:
- The Best Menstrual Cups to Try Instead of Tampons
- 6 Signs You Should Consider Switching From Birth Control Pills to an IUD
- Craving Sugar? A Dietitian Says You May Need More of This Surprising Nutrient
- Doctors Say Knowing About This Vaccine Could Cut Your Cancer Risk Significantly
- Dietitians Explain Just How Long It Takes Vitamin D to Work in Your Body