Gender differences in common health conditions
Men and women can be affected by the same health conditions but in different ways. Symptoms may be similar, but how these conditions manifest themselves in the body and the type of treatment needed can vary based on gender. Both sexes are prone to specific diseases, but for some conditions, such as heart disease, which affects more men at an earlier age than women, health experts remain unclear as to why.
Read on down below as our medical experts explain some of the factors that link gender and health. (Plus, take a look at the signs you’re healthy from every type of doctor.)
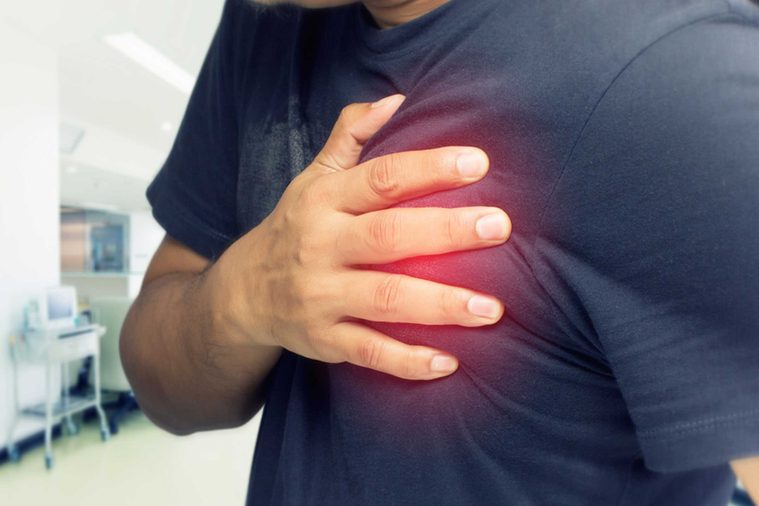
Heart disease
Heart disease is the leading cause of death for both men and women in the U.S., but men are at a higher risk at an earlier age. On average, women develop heart disease about a decade later due to the protective effects of the female hormone estrogen. After menopause, the risk of heart disease can go up in women. Heart attack symptoms in women may include shortness of breath, nausea, jaw, neck or back pain, and fatigue rather than classic chest pain. The traditional risk factors for heart disease, such as family history, are generally the same for both genders.
“Ironically, however, women have a higher mortality from heart disease than men due to both underdiagnosis and undertreatment,” says Poulina Uddin, MD, a cardiologist at the Scripps Women’s Heart Center in San Diego. Women are also more likely than men to develop small vessel disease, a condition where blockages occur in the tiny vessels within the heart muscle rather than in the large, surface arteries. “Postmenopausal women, in particular, are subject to a sudden and unusual change in the shape of the heart muscle known as Takotsubo cardiomyopathy that occurs in response to severe emotional stress,” says Mehran Movassaghi, MD, urologist and men’s health specialist at Providence Saint John’s Health Center in Santa Monica. “Also called ‘broken heart syndrome,’ the condition is characterized by chest pain and changes in the heart’s electrical activity that mimic a heart attack.” These are the heart disease risk factors you might now know about.
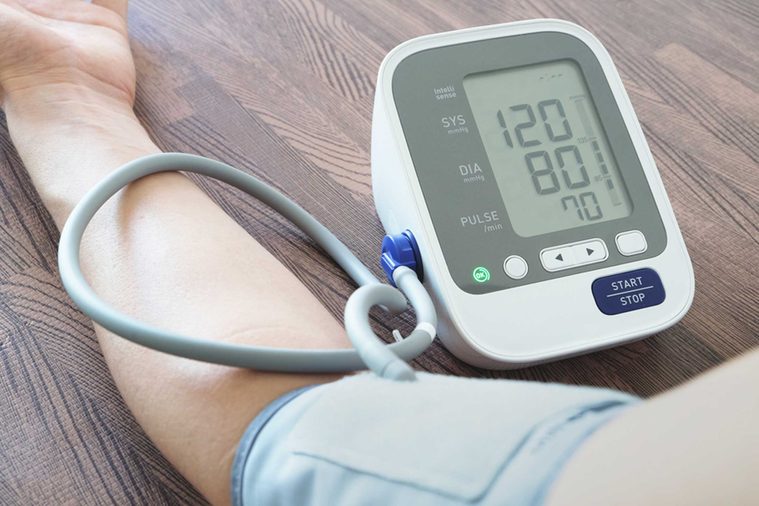
Hypertension
Hypertension, also known as high blood pressure, affects around 85 million people each year. This number is growing, according to the World Health Organization, which points the blame at processed foods and their high levels of salt. In general, the risk of hypertension goes up as people age. However, up until age 45, the risk of hypertension tends to be higher in men than women. The risk is about the same for men and women who are in their 50s and 60s. At 65 or older, the hypertension risk is much higher in women compared with men, according to the American Heart Association. While hypertension is more common in young men than young women, a 2015 study published in the journal of Biodemography and Social Biology showed serious gender disparities when it comes to awareness of hypertension risks. In that study, 12% of young adult women had hypertension compared with 27% of men the same age, but only 32% of women and 25% of men knew they had hypertension. The findings suggest that regular medical visits are critical for improving hypertension awareness among both men and women and encourage healthcare providers not to assume that women are in the clear.

Breast cancer
Most women are well aware of their risks of breast cancer: About 1 in 8 U.S. women (12 percent) will develop invasive breast cancer over the course of her lifetime, according to the American Cancer Society. But men get breast cancer too, and they typically receive a much worse diagnosis than women. “Any woman living in the U.S. has been told a thousand times that she needs to have breast examinations and mammograms,” says Lee Loewinger, MD, a cardiologist at Brooklyn Cardiovascular Care, PLLC, in New York. “However, there is very little education for males about this cancer, so men tend to be less proactive about getting a breast lump examined.” When it is diagnosed in men, the cancer is much more likely to be more advanced, more dangerous, and more difficult to treat. Adding to these issues, Dr. Loewinger points out that males have less breast tissue than females, and male breast cancer is more frequently found under or near the nipple, which makes it easier to miss on exam.

Stroke
While many of the risk factors for stroke are the same for both genders, including a family history of stroke, high blood pressure, and high cholesterol, some risk factors are unique to women. These include taking birth control pills, being pregnant, using hormone replacement therapy (HRT), having frequent migraine headaches, and having a thick waist, a common trait in postmenopausal women. These reasons may substantiate why about 55,000 more women have a stroke each year than men, explains Dr. Movassaghi. “Another possible explanation is women’s longer average life span, since advancing age is a key element in stroke risk.” Symptoms of stroke are often different, too.
As Thomas C. Royer, MD, co-author of Breaking Out of the Health Care Abyss: Transformational Tips for Agents of Change, points out, men often showcase classic complaints of numbness and weakness of an extremity, difficulty walking, double vision, and sensory abnormalities, while women often complain of generalized weakness, altered mental status and fever, and hence, often have a “missed-diagnosis” until the stroke is full-blown. These are the surprising health risks men need to watch out for.

Diabetes complications
This disease, which affects approximately 30.3 million Americans (9.4 percent of the population), tends to be more severe in women than men. Diabetes, which impacts how the body processes blood sugar, can increase the risk of complications like heart disease, kidney disease, and vision problems, among other problems. “Researchers speculate that HDL, or ‘good,’ cholesterol, which is normally higher in women than men, may be behind the gender disparity,” says Dr. Movassaghi. “When you get diabetes, the high triglycerides (blood fats) drive down HDL levels in women—and the combination of high triglycerides and low HDL adds up to a greater risk of heart disease.”
Researchers are trying to determine whether sex hormones, estrogen and testosterone, play a role in why women with diabetes are more vulnerable to kidney disease than diabetic men. “Studies have indeed found that lower estrogen levels are associated with kidney disease, but it’s not known whether there’s a cause-effect relationship or exactly how the lack of estrogen may contribute to kidney disease,” Dr. Movassaghi explains. “If there is a sex hormone connection, perhaps women with diabetes could improve their kidney health if the balance between testosterone and estrogen were restored with hormone therapy.” He agrees, however, that more research is needed to validate such an approach. Here are 9 diabetes myths you should ignore.

Hair loss
Both genders experience hair loss. However, men do have a higher prevalence of hair loss and experience patterns of baldness differently. “Male-pattern hair loss usually begins earlier in life and men lose from the front and vertex of the scalp,” explains Jerome Garden, MD, the director of the Physicians Laser and Dermatology Institute in Chicago. This leads to a receding hairline and a bald spot on top. “Female-pattern hair loss usually begins after age 30 and is a more subtle, diffuse hair loss with preservation of the frontal hairline,” Dr. Garden adds.
He explains that these differences are likely the result of gender hormones—testosterone is the main drive of hair loss in men, while estrogen has a protective factor against hair loss in women. Women, however, are more likely to seek out treatment for hair loss, despite more men experiencing the condition. Unfortunately, Dr. Garden points out that the treatments for female hair loss are less than for men. “Both genders can use minoxidil over-the-counter (brand name: Rogaine), which can help some patients, but the prescription medicine for hair loss, finasteride (brand name: Propecia), is only approved for men.” Other less-used treatment options that can help both genders are lasers, surgical hair transplants, and wigs.
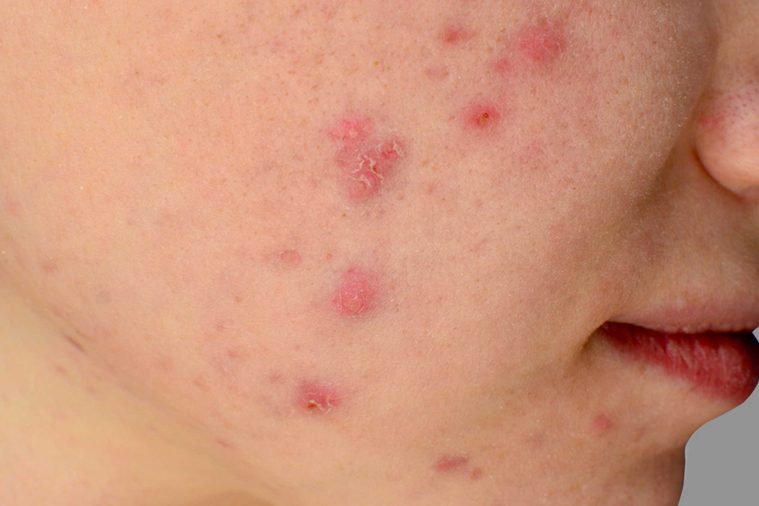
Acne
While we tend to assume both genders experience this annoying skin condition equally, especially upon hitting puberty, men tend to have it worse and it’s more difficult to treat in men than women. “This is likely due to the increased testosterone in men and the increased size of sebaceous (oil) glands in men, which results in oilier skin,” explains Dr. Garden. “However, women tend to seek out physician treatment for acne more than men.” Ironically, however, the type of acne that tends to remain in one’s adult years tends to affect women more often and is a frequent reason for a woman to visit their dermatologist’s office. “During their 30s, over 25 percent of women still experience acne, while only 12 percent of men do,” Dr. Garden says. “This adult female acne can be difficult to treat and generally deserves a more hormone-centric approach to treatment options.” Check out Dr. Pimple Popper’s best advice for fighting acne.
Autoimmune disorders
Of the 50 million Americans with autoimmune diseases, an astonishing 75 percent of them are women, according to the American Autoimmune Related Diseases Association. These disorders, including systemic lupus erythematosus, rheumatoid arthritis, Hashimoto’s thyroiditis, multiple sclerosis, and primary biliary cirrhosis, cause the body’s immune system to attack its own organs. Lupus, in particular, is primarily a women’s disease, affecting about nine women for every one man. However, according to Michael Guma, DO, director of Rheumatology Riverside Medical Group in Northern New Jersey, men tend to have a more aggressive disease when they are diagnosed with lupus, though large-scale studies are needed to fully substantiate this observation.
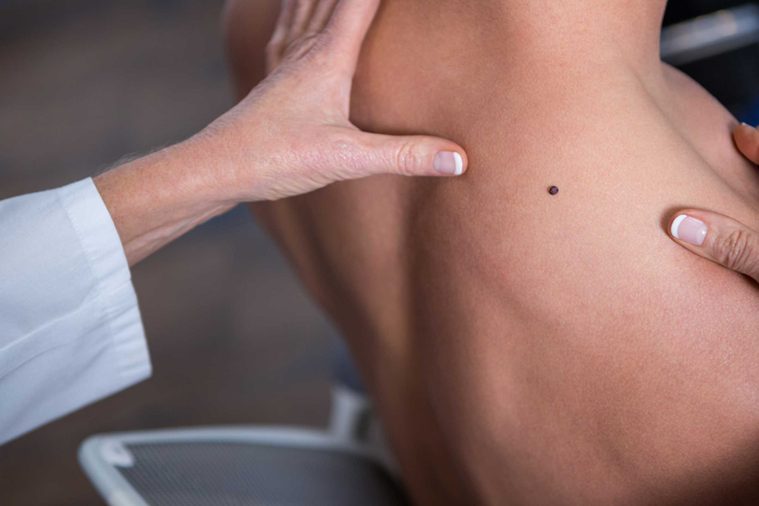
Skin cancer
Approximately one in every five Americans will get some form of skin cancer in their lifetime, according to Skin Cancer Foundation, and men are two times more likely to get it than women. “This is likely due to increased sun exposure in men, as they tend to have higher rates of outdoor jobs,” notes Dr. Garden. “Additionally, men are less likely to be vigilant about using sunscreen or seeking shade.” Women tend to be more proactive when it comes to scheduling skin check-ups and regularly noticing skin changes, such as a changing mole. The locations for skin cancers are different as well. “Men tend to get more skin cancers on their heads and ears, likely due to having less hair to protect this skin, as well as their backs, since they are more likely to be outside without a shirt,” Dr. Garden says. “Women are more likely to get melanoma on their legs, likely due to wearing skirts.” Age is another factor, as women younger than 40 are twice as likely as men to get melanoma, possibly as a result of recreational sun tanning.

Osteoporosis
This bone-weakening disease affects about 54 million Americans, most typically those over the age of 50, the National Osteoporosis Foundation reports. Women, in particular, are at a greater risk than men, with one in two women affected compared to only one in four men. “The female hormone, estrogens, tends to have a protective effect on bone density,” explains Dr. Guma. “As a woman reaches menopause, and her levels of estrogen plummet, her rate of bone loss increases significantly.” This can result in increased chance of fractures over the course of her life. Additionally, Dr. Guma points out that women have smaller and thinner bones than men to begin with, which also puts them at risk for the condition. Plus, the 30 things that can help boost your bone density.

Depression
Mental health conditions can also differ in their impact on the sexes. Depression, for example, is twice as common in women than in men. “This results, in part, from the hormonal and genetic differences that contribute to the onset of depression,” explains Dr. Guma. “Women may spend more time ruminating about negative thoughts, which has been known to worsen depression.” Anxiety is another depression-related mental illness that tends to be more common in women. When it comes to seeking out help, however, women are more likely than men to speak to a mental health professional, which may statistically explain why more women are diagnosed.
“The diagnosis of depression is often harder to diagnose in men, as men tend to find something to distract them and occupy their thoughts,” Dr. Guma says. “In some cases, they may resort to risky behaviors such as unsafe sex, gambling and smoking.” Symptoms of depression can be unique for men compared to women as well. In men, depression can present with anger and irritability more often than in women, Dr. Guma points out, and men are more likely to abuse alcohol or another substance while depressed. Here are the silent signs your body might be in big trouble.

Multiple sclerosis
Much is still unknown about this chronic and unpredictable disease that attacks the central nervous system, although women are two to three times more likely to develop multiple sclerosis (MS) than men. Like many other conditions that plague more women than men, MS tends to take a more aggressive course in men. “Men usually have fewer relapses and usually have motor difficulties including trouble walking,” explains Dr. Royer. “Women, on the other hand, usually present with more sensory challenges, including visual impairment, numbness and tingling in extremities and vague muscle symptoms.” In both genders, however, early diagnosis, because of the vague symptoms, does not often occur on the first several visits to the physician. (Here are some signs of MS.)
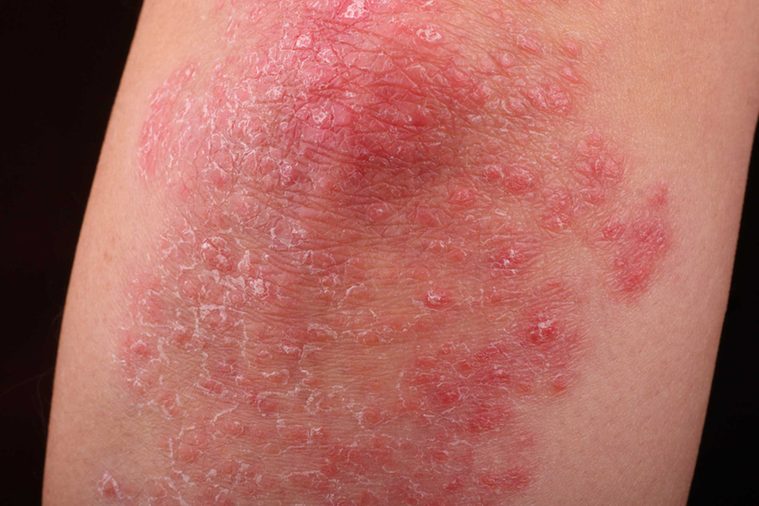
Psoriasis
This chronic skin condition affects over 100 million people worldwide according to the National Psoriasis Foundation. Though there’s no indication that psoriasis is more common in men or women, nor are there obvious differences in physical symptoms. However, John Zibert, PhD, a psoriasis expert and chief medical officer at LEO Innovation Lab in Copenhagen, says “women often show lower levels of self-confidence, feel greater loss of control and, most importantly, experience significantly higher levels of stress. “Given the importance of appearance to women’s self-esteem and confidence levels, they may feel more emotionally vulnerable compared to men, however, related psychological problems across all genders of people living with psoriasis can affect everyday social activities and work, which can lead to embarrassment, anxiety and even depression.” Next, check out these serious diseases that strike women more than men.
