Separating fact from fiction can be tricky when you have a chronic condition—especially one as misunderstood as diabetes. Here, we debunk 19 diabetes myths that could be sabotaging your health.

Myth: Eating sugar causes diabetes
Fact: Arguably the biggest diabetes myth is that sugar causes diabetes. That said, sugar does seem to play an indirect role. For one thing, eating too much of the sweet stuff can lead to obesity, which is a risk factor for type 2 diabetes, says diabetes expert David Marrero, PhD, director of the University of Arizona Health Sciences Center for Elimination of Border Health Disparities. And research suggests that sugary drinks can increase diabetes risk, even after accounting for weight.
A large study published in 2019 in Diabetes Care found that increasing consumption of sugary beverages—including drinks with added sugar, 100-percent fruit juices, or artificially sweetened drinks—was associated with a 16-18 percent higher risk of type 2 diabetes. These rapidly absorbed sugars may damage cells in the pancreas that secrete insulin.
There are sneaky sources of sugar hiding everywhere, so you’re probably consuming more than you think. Look at nutrition labels and avoid highly processed foods. The World Health Organization recommends adults have no more than six teaspoons (or 24 grams) of sugar a day.

Myth: Thin people don’t get type 2 diabetes
Fact: More than 90 percent of people with diabetes are overweight or obese, according to a study published in 2017 in Diabetes Spectrum. So that means 1o percent of people with diabetes are not overweight or obese. “The risks for developing type 2 diabetes are complex and multiple,” says Emily Nosova, MD, an endocrinologist specializing in diabetes at the Mount Sinai Health System in New York City. “Excess weight and fat distribution—especially visceral fat—certainly play an important role. But several other important factors also contribute to a person’s risk of type 2. Those include genetics, history of medication use, cancer or autoimmune history, and lifestyle habits, such as alcohol intake and smoking.”
If you have multiple risk factors for diabetes, your chances of developing the disease are greater, she adds. Regardless of weight, if you are 45 or older get your blood sugar levels checked every three years—especially if you’re sedentary; have a personal history of gestational diabetes; heart disease; high blood pressure or high cholesterol.

Myth: Exercise is dangerous for people with diabetes
Fact: This couldn’t be further from the truth: Numerous studies show that regular physical activity actually helps lower blood sugar levels and can improve diabetes management. The important thing is to get your doctor’s clearance if you’ve been inactive.
“I advise my patients to start with a manageable daily exercise routine,” says Dr. Nosova. “Come up with a realistic schedule based on work, commitments, sleep, and meal-timing. If daily exercise isn’t feasible, then try not to let more than two days go between exercise. Ideally, the goal is to work your way up to at least 150 minutes of cardiovascular exercise per week as per the American Diabetes Association (ADA) guidelines.”
You should also talk to your doc or a diabetes educator about how and when to test your blood sugar as part of your workout routine. “Blood sugar levels may fluctuate depending on the type of exercise,” adds Dr. Nosova. “Generally, cardiovascular exercise will lower blood sugar while weight training may cause a rise in blood sugars. Another key point: Diabetes medication doses, especially insulin, will likely change with exercise. It’s important to work closely with your diabetes care team to optimize for a safe exercise plan.” (And take extra precaution if you’re working out during the summer.)
To play it safe, especially if you’re new to exercise, keep a diabetes-friendly snack on hand in case you need to bring your blood sugar back up post-workout. Feeling weak or shaky? Your body is telling you to take a break or stop.

Myth: Diabetes has no symptoms; only my doctor can detect it
Fact: There are some early symptoms of type 2 diabetes, but they’re often subtle enough to overlook or ignore. No wonder 20 percent of people with diabetes don’t even know they have it, according to the Centers for Disease Control and Prevention (CDC). Telltale signs: feeling dehydrated even when you’ve been drinking, drinking more fluids than usual, frequent trips to the bathroom, feeling tired and hungry all the time, or losing weight without changes to diet or lifestyle. If you notice any of these symptoms, see your doctor. Diabetes is easily diagnosed with a blood test.

Myth: You shouldn’t get pregnant if you have diabetes
Fact: “People are worried about the risk to themselves and their child, or worry that they can’t become pregnant at all, particularly in those with type 1; but that’s just not true anymore,” says Marrero. “This myth stems from a time when diabetes was poorly controlled and understood.” There’s still a risk of complications, such as preterm birth, if you aren’t vigilant in managing your blood sugar levels. But plenty of women with diabetes become pregnant and have normal pregnancies with proper monitoring, he says. The ADA offers guidance on how to have a healthy pregnancy with diabetes. Here are the best shoes for women with diabetes.
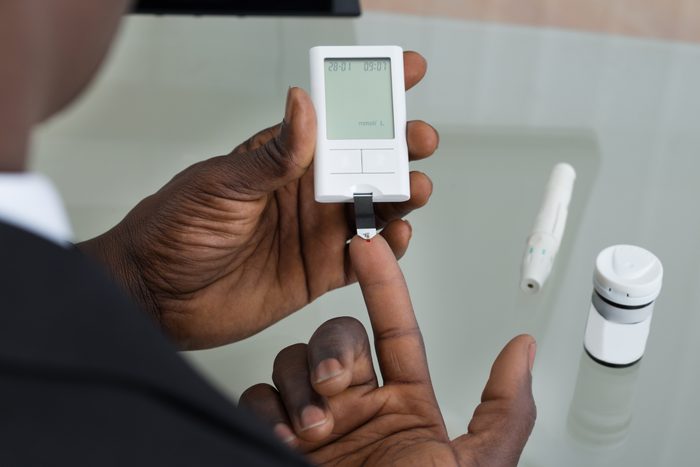
Myth: You’ll always be able to tell if your blood sugar levels are too low or too high
Fact: Initial signs of elevated blood sugar are often so mild that they’re easily overlooked. That’s why it’s important to regularly test and track blood sugar levels (if your doctor recommends it). Not only can this alert you to a dip or spike even before your body sends you signals, it also helps you learn how diet, exercise, stress, and illness affect your levels.
When you have low blood sugar (hypoglycemia), you may experience sweating or shakiness. This can happen if you are taking insulin or other blood sugar-lowering medications. But people who’ve had diabetes for a while often develop something called “hypoglycemia unawareness.” That means they’ve lost the ability to feel these symptoms, says Deena Adimoolam, MD, assistant professor in the department of endocrinology, obesity, and metabolism at the Icahn School of Medicine at Mount Sinai in New York City. Follow your doctor’s recommendation for how often to check blood sugar levels. Call 911 immediately if you have blurred vision, feel confused or sleepy, or experience vomiting. And become familiar with these silent diabetes complications.

Myth: People with diabetes have to follow a strict, no-sugar diet
Fact: Dessert is not off the table—not for people with type 1 diabetes or for people with type 2. With type 2 diabetes, the key is moderation. Limit sweets to a small portion of your overall diet and fill the rest with fiber-packed whole grains, veggies, and lean protein. If you have type 1, it’s a little trickier; you have to adjust your next insulin dose to compensate for sugary carbs.
“It just takes a bit of trial and error to figure out the right insulin dose, but it’s very manageable and learnable,” says Marrero, who has type 1 diabetes. “Using a continuous glucose monitor that will show you when your levels are changing is a great option.”
Myth: If you have diabetes, you’re more likely to catch the coronavirus
Fact: If you have diabetes, you’re no more likely to catch the coronavirus than the general population, according to the ADA. You are, however, likelier to experience complications if you do get Covid-19.
“Among hospitalized patients, those with uncontrolled diabetes—meaning their blood sugars are higher than the recommended goal range—tend to fare worse from coronavirus,” says Dr. Nosova. “The reasons for this aren’t clear but several theories have been posed. Prior respiratory viruses such as MERS have been shown to cause insulin resistance and an associated rise in blood sugars. Medications and treatments used for viruses, including steroids, can also raise blood sugars dramatically. And there is some thought that pancreatic tissue can be injured by the virus, so there’s less insulin available for use in the body.” To stay safe, get up to speed on 12 coronavirus symptoms everyone should watch for.
Myth: There is no cure for diabetes
Fact: This is false-ish, says Eduardo Sanchez, MD, chief medical officer for prevention and chief of the Center for Health Metrics and Evaluation at the American Heart Association (AHA) in Dallas. Type 2 diabetes is the more common form of the disease and is most closely linked to obesity. So for people who are obese, some types of gastric bypass surgery can almost completely reverse symptoms in some people, at least for a while. (It can vary from person to person and symptoms may return later in life.) In fact, one study, published in 2019 in Diabetologia, found that 75 percent of obese people with type 2 who underwent Roux-en-Y gastric bypass surgery experienced diabetes remission after a year.
“The idea of a cure is elusive, but it is not outside of our grasp,” says Dr. Sanchez. “We are not optimizing our efforts to prevent diabetes and there is a tremendous opportunity for hope because we can dramatically improve quality of life and enhance the length of life of people with diabetes through lifestyle changes and medication.”
Myth: There is no way to prevent it
Fact: Prediabetes is a wake-up call that you’re at risk for developing type 2 diabetes. It occurs when your blood sugar (or glucose) is higher than it should be, but not quite at diabetes level—yet.
Around one in three adults in the U.S. have prediabetes, but 84 percent of them don’t know it, according to the CDC. A simple blood test can tell if you have prediabetes and get you on the path to preventing or delaying a diagnosis of type 2 diabetes. “There is evidence that says adopting a healthy lifestyle can lower the risk of developing type 2 diabetes,” Dr. Sanchez says. (These are the best and worst foods to prevent diabetes.)

Myth: All people with diabetes should follow the same diet
Fact: There is no one-size-fits-all diet for people with diabetes in the same way that there is no single diet for people without diabetes, Dr. Sanchez says. There are many styles of eating that can help manage diabetes—from a Mediterranean-style diet that’s rich in vegetables, healthy fats, some grains, and lean proteins to the keto diet, which is low in carbs, moderate in protein, and high in fat. (Learn what the 2-day diet is and how can it help manage diabetes.)

Myth: If you have diabetes, you will develop heart disease
Fact: “We know that heart disease is most likely to shorten the life of someone with diabetes,” says Dr. Sanchez. “We also know what to do to lower this risk and change the trajectory.” This includes adopting a heart-healthy lifestyle and making sure blood pressure, blood cholesterol, and glucose levels remain at healthy levels. There is also a new class of medicine that reduces heart diseases such as GIP-1 agonists and SGLT2 inhibitors. (Learn more about how to make these changes at Know Diabetes by Heart.)

Myth: You will lose a limb
Fact: Just because you have diabetes doesn’t mean you’ll lose a limb, says Maria Elena Rodriguez, RD, diabetes program manager at The Diabetes Alliance of the Mount Sinai Health System in New York City. “Staying well informed about how to manage blood sugar and taking your medications as directed is the best way to prevent complications including the loss of a limb.”
To get ahead of the risk: Schedule a complete foot exam at least annually and check your feet daily. If you have diabetes, even a small cut can have devastating consequences. That’s because the disease causes nerve damage that takes away the feeling in your feet and reduces blood flow to the feet, making it harder to heal. Pamper your feet with these recommended slippers for men with diabetes.
Myth: Everybody with diabetes needs insulin therapy
Fact: Insulin is a hormone made by the pancreas that allows your body to use glucose for energy. When you have diabetes, your body either does not produce insulin (type 1) or your cells are resistant to its effects (type 2). As a result, glucose builds up in your blood and can damage the body. Over time, uncontrolled blood glucose levels can cause serious health problems. People with type 1 diabetes, an autoimmune disease, always need to take insulin to survive; that’s not true for people with type 2 diabetes, the most common type.
“Not everyone with type 2 diabetes will end up needing insulin to control blood sugar,” says Rodriguez. Other medications and lifestyle changes such as weight loss and regular exercise may be enough to manage your diabetes.
Myth: You will go blind
Fact: Uncontrolled high blood sugar can damage blood vessels in the retina—the back wall of your eye. What’s known as diabetic retinopathy is the most common cause of vision loss for people with diabetes. But it often has no symptoms. Losing your eyesight is not inevitable. Prevent blindness by getting a comprehensive dilated eye exam at least once a year, Rodriguez says. Keeping blood sugar under control is the best way to prevent complications like vision loss.

Myth: You will need dialysis
Fact: Dialysis—a treatment that does some of the work usually done by healthy kidneys—is needed when your kidneys can no longer take care of your body’s needs. You need dialysis if you develop end-stage kidney failure, something people with diabetes are at risk for.
Here’s why: When you have diabetes, the blood vessels in your kidneys suffer damage, which means they’ll no longer effectively filter your blood. Left untreated, this can result in kidney failure. But tight blood sugar control can lower the risk of all diabetes complications, including kidney failure, says Rodriguez.
Medications such as SGLT2 and GLP-1 or ACE/ARB can prevent and slow the progression of kidney disease. Note that good blood pressure control also prevents kidney disease.

Myth: You can’t have even a sip of alcohol
Fact: Drinking alcohol if you have diabetes can be okay, but you have to be smart about it. “Alcohol contains empty calories which convert to sugar in the body, and then metabolize as fat,” says Rodriguez. Don’t overdo it, and make sure mixers are sugar-free—think diet soda or seltzer instead of sugary juices. Moderate alcohol consumption means no more than one drink per day for women; no more than two per day for men. (One drink equals a 12-ounce beer, a 5-ounce glass of wine, or 1½ ounces distilled spirits such as vodka.) Don’t drink on an empty stomach, either. Your risk of low blood glucose increases when you haven’t eaten and after drinking.

Myth: Gestational diabetes means you will develop diabetes
Fact: Around 6 to 9 percent of pregnant women in the U.S. experience gestational diabetes—a type of diabetes that can develop during pregnancy in women who don’t already have diabetes. About half of them go on to develop type 2 diabetes, according to the CDC. But that also means 50 percent don’t. “Your body may go back to regulating blood sugar properly after delivery,” says Rodriguez. Make sure your doctor checks your blood sugar during your annual well-check visits so that you can catch any changes early. Check out these sandals recommended for women with diabetes.

Myth: Diabetes means you can never run a marathon
Fact: Exercise, even the kind that requires extreme physical exertion, isn’t off limits if you take the appropriate precautions, suggests a study published in 2018 in Diabetes Technology & Therapeutics. Researchers looked at four ultramarathon runners with type 1 diabetes who took on a 51-mile mountain race. All four avoided severe hypoglycemia by significantly reducing their insulin dose and consuming additional carbohydrates.
Just as with any exercise, “if you are going to exercise for more than an hour, test your blood sugar before and after and make sure to carry snacks with you,” says Rodriguez. Not sure if you should ramp up your exercise? Talk to your doctor or diabetes educator.

