Insulin Injections: What Diabetes Doctors Want You to Know
Updated: Aug. 22, 2020
About six million Americans use insulin injections, according to the American Diabetes Association. Learning how to take it correctly, watch for hypoglycemia, and stay safe while on-the-go can ensure you feel your best.
The primary factor behind diabetes is that your body may not make enough insulin (type 1 diabetes) or it fails to respond to the insulin your pancreas releases, which is known as insulin resistance (type 2 diabetes).
Insulin basically acts like a key to unlock cells in your muscles, fat, and liver and drive in glucose from your bloodstream where it can provide energy for your body, explains the Hormone Health Network, an educational arm of the Endocrine Society. Without insulin, blood sugar rises to toxic levels in the bloodstream.
If you have type 1, you need insulin injections daily to survive. People with type 2 can overcome insulin resistance and control their blood sugar with a combination of diet, exercise, and oral medication, but they often need to take insulin too. (Learn more about the differences between type 1 and 2 diabetes.)
Being able to replace insulin in the body has been one of the great medical advances of all time. “For many patients, insulin is huge in getting blood sugars under control and preventing long-term complications,” says Anthony Pick, MD, an endocrinologist at Northwestern Medicine Lake Forest Hospital in Lake Forest, Illinois.
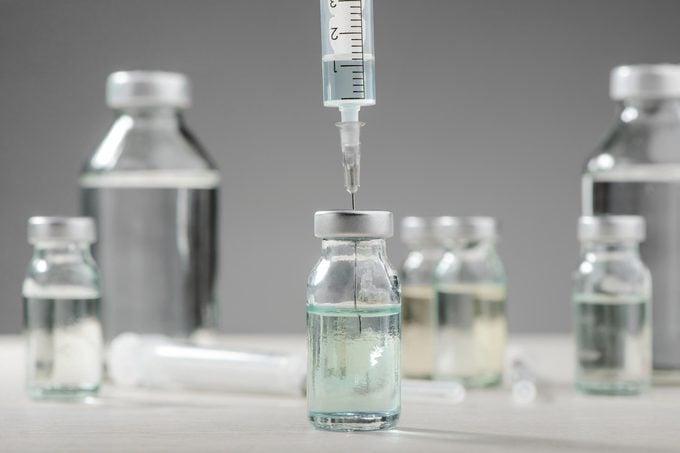
There are various types of insulin
Depending on your lifestyle and how advanced your insulin deficiency is, your doctor may advise one of the five types of insulin injections, according to the American Diabetes Association (ADA). They all take a different amount of time to reach the bloodstream, reach a peak, and remain effective. These include, per the ADA:
Rapid-acting insulin: Works in 15 minutes, peaks in one hour, lasts up to four hours
Regular/short-acting insulin: Works in 30 minutes, peaks in two to three hours, lasts up to six hours
Intermediate-acting insulin: Works in two to four hours, peaks in four to 12 hours, lasts 12 to 18 hours
Long-acting: Works in several hours, lasts 24+ hours
Ultra long-acting: Works in six hours, no peak, lasts 36 hours

You’ll most likely need to give yourself an injection
Insulin is a large protein molecule, says Dr. Pick: “If you took it orally, your body would just digest it.” While there is a rapid-acting inhaled insulin available, most people take it via insulin injection, and some take it through an insulin infusion pump.
Needing insulin isn’t “a bad sign”
If you have type 1 diabetes, you need insulin to keep you alive. If you have type 2 diabetes, your life may not depend on insulin, says Dr. Pick, but you could need it for better blood glucose control. “Many people associate needing insulin with complications,” he says. Patients often remember a family member who went on insulin injections and then suffered from severe diabetes-related complications like blindness. But that’s not the insulin’s fault, explains Dr. Pick; these symptoms are usually a result of poorly controlling the disease and allowing it to advance.
Be sure to rotate injection sites
Insulin injections need to go into a layer of fat. Your options include the stomach, back of the arm, lower back, love handles, and the outer part of the leg, says Sheri Setser-Legg, a certified diabetes educator (CDE) at the University of Kentucky Barnstable Brown Diabetes Center in Lexington, Kentucky. You’ll likely find your favorite spot, she says. Still, it’s important to alternate. “Because it is an injection, over time you run the risk of developing scar tissue if it’s done in the exact same spot every time, and that will affect the absorption of insulin,” she says. Your healthcare team can suggest a rotation pattern that might work for you.
The injection is not that bad
It’s not unusual to be worried about the idea of giving yourself injections regularly. And while it’s not exactly fun, “99 percent of the time, the anticipation of an insulin injection was worse than the act of doing it,” says Setser-Legg. It’s important to keep this perspective because you need to get used to giving yourself the insulin injection rather than relying on someone else to do it for you. It’s what ensures your independence with your medical care, she says.
Hone your technique
Once you’ve been using insulin for a while, you may let the best practices slip by the wayside. “We encourage a sterile technique. This is something that’s going into your body,” explains Setser-Legg. Even if you’ve been using insulin for years, remember to play it safe by cleaning the area with rubbing alcohol and letting it dry before the injection, she says.
Talk about a travel plan
There’s no reason you have to stay home if you’re on insulin. But, there are a few things you should talk to your doctor about before you go. The Centers for Disease Control and Prevention (CDC) advises travelers to discuss how to adjust insulin dosing based on your new time zone, find a local pharmacy in case you need more, and bring diabetes supplies in your carry-on if you’re traveling by plane to protect the insulin from extreme temperatures ( and yes, you can take your meds through security). Just in case you get stuck at your destination, bring extra.
Watch the heat
Both insulin and other equipment (like a pump or monitor) can degrade in the heat. For that reason, the CDC offers this rule: Never store diabetes supplies in a hot car or in direct sunlight. Meaning: When you get to the beach, take your meds with you in a cooler. And, review these ways summer can change the way you manage your diabetes.
Know the symptoms of hypoglycemia
If you’re on insulin therapy, it’s important to know how to spot hypoglycemia, a condition where you have very low blood sugar, says Setser-Legg. Those include shakiness, dizziness, weakness, sweating, and blurry vision, but can vary depending on the person. “If you have hypoglycemia, you’ll know it,” she says. Check your blood sugar. If it’s 70 milligrams per deciliter (mg/dL) or below, it should be treated by consuming 15 grams of fast-acting carbs. Good sources include a half cup of juice or glucose tablets, says Setser-Legg. She recommends staying prepared by carrying fast-acting carbs with you at all times.
Weight gain on insulin isn’t inevitable
Because insulin has been associated with weight gain, some patients are hesitant to use it, says Dr. Pick. While it’s true that some people with poorly controlled diabetes will gain weight, you can decrease this risk by following healthy lifestyle habits (good nutrition, regular exercise) and proper insulin dosing. “Lowering your intake of simple carbs can decrease the amount of insulin needed meal-to-meal, and that will also minimize weight gain. This is true in both type 1 and type 2 diabetes,” he says. It’s not just exercising that matters—but what type you’re doing: This workout may help normalize blood sugar levels in as little as two weeks.
New technology makes insulin even easier
Smart insulin pens are now available to streamline insulin dosing, says Dr. Pick. The device company Companion Medical manufactures an FDA-cleared smartpen called the InPen. It uses a reusable injector pen that calculates your doses and keeps track of injection data and is suited for patients who need to inject insulin multiple times a day, according to the company. It’s designed to be paired with a smartphone app that can track and calculate doses and share the data with your healthcare team, including family members.
You can still live your life
Don’t think that you’re limited now that you’re on insulin. Says Setser-Legg: “We have patients who are athletes, rock climbers, and skydivers. If you know how your insulin works, how to treat low blood sugar, and how to take insulin appropriately, there’s no reason you can’t do any activity you want to do.” (These are the type 2 diabetes symptoms that you may miss.)

















