
Breast cancer treatments have progressed lightyears from the old days of one-size-fits-all therapy. Julie Gralow, MD, chief medical officer and executive vice president of the American Society for Clinical Oncology (ASCO), says increased molecular and genetic knowledge have paved the way for drugs and procedures that are now highly individualized to the specific cancer and the specific individual. They can find out who needs more treatment, and who needs less.
As a result, many breast cancers that were once considered deadly have evolved into chronic conditions with patients living years or even decades after diagnosis. According to the American Cancer Society, breast cancer deaths have reduced 43% since 1989.
Here’s what’s happening in the world of breast cancer treatment.

“Smart bomb” drugs
“Smart-bomb” drugs are engineered to deliver medication straight to tumor cells. By far the biggest breakthrough of the past year was the August approval of the drug trastuzumab deruxtecan or T-DXd (brand name Enhertu), one of a new class of drugs known as antibody conjugate drugs (ADC). The trastuzumab (Herceptin) component—an antibody trained to hone in on the HER2 receptor—carries deruxtecan, a chemotherapy agent, directly to the cancer cell.
Enhertu is the first medication for patients with inoperative or metastatic “HER2-low” breast cancer. These are tumors which express small amounts of the HER2 protein, known to accelerate tumor growth. Clinical trial results released at ASCO’s 2022 annual meeting reported a doubling of progression-free survival in women who took Enhertu versus chemotherapy alone…an achievement which garnered a standing ovation. The approval has already changed practice, says Azadeh Nasrazadani, MD, PhD, assistant professor of breast Medical Oncology at The University of Texas MD Anderson Cancer Center in Houston, TX.
What Are the Best Foods to Fight Cancer? Here’s What’s in a Cancer Dietitian’s Fridge
A new subtype of breast cancer
The approval of Enhertu also marks a new way of classifying breast cancer. Previously, breast tumors were distinguished by whether or not they expressed the HER2 protein: HER2-positive or HER2-negative. Herceptin has been the go-to drug for HER2-positive tumors for decades. Now it appears that it will work on sort of “cross-type” tumors that were previously considered HER2-negative and therefore not candidates for Herceptin.
“The real breakthrough is that Enhertu worked in tumors not considered HER2-positive,” says Daniel Stover, MD, a medical oncologist with The Ohio State University Comprehensive Cancer Center-The James. “This is mind-blowing because doctors have spent the last 15 years defining specific subtypes of breast cancer and specific treatments for specific subtypes. This is a drug that can be used across multiple subtypes.” It’s likely that other drugs, such as the ADC sacituzumab govitecan (Trodelvy) will also work across subtypes, he adds.
8 Signs of Breast Cancer You Might Be Ignoring (Besides a Lump)

More targeted drugs, more drug combinations
Even some of the most effective drugs for breast cancer lose their edge over time as cancer cells learn to outsmart them. This is especially true in metastatic settings. “Cancer cells inevitably develop resistance to each therapy,” says Dr. Nasrazadani. “This necessitates the development of novel agents that target different pathways. It’s a very active area of research.” It’s also resulted to the approval of several new drugs, such as alpelisib (Piqray). Dozens of other drugs are in various phases of clinical trials, giving oncologists and patients many more options.
The ability to develop targeted drugs rests on advances in technology that can pinpoint the molecular and genetic characteristics of tumors. “It’s helpful to have data on the underlying aberrations and pathways that are promoting aggressive cancers,” says Dr. Nasrazadani. “More sophisticated sequencing assays helps us see if an agent is already available and to see more patterns about where drug development needs to go.”
Here’s Who Is at Greatest Risk for Developing Cancer from Drinking Alcohol
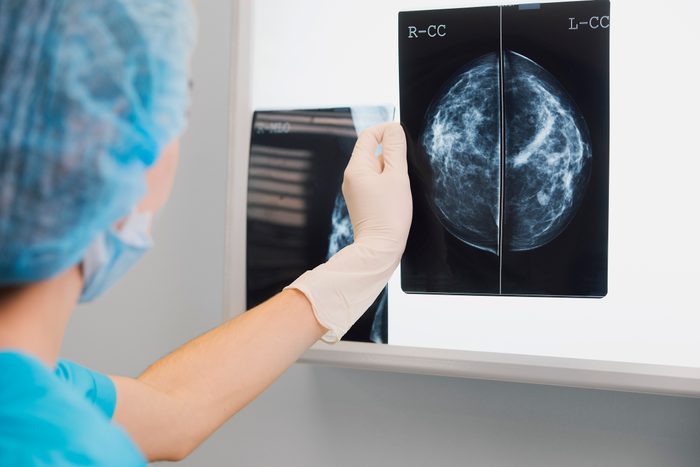
“Right-sized” treatment
Oncologists continue to find ways to cut back unnecessary treatment and still get good results. “We have less and less surgery, less radiation, less chemo, less everything,” says Paul Baron, MD, chief of breast surgery and director of the breast cancer program at Lenox Hill Hospital.
But there are other patients who would still benefit from bigger treatment guns, leading to a “right-sized” approach. “A big part of what we’ve been focusing on in the last few years is optimizing treatment, so figuring out which tumors benefit from more aggressive treatment and which benefit from less,” says Dr. Gralow.
Breast Cancer Treatment: 12 Things Oncologists Wish Patients Knew
“Neoadjuvant” therapy
One strategy is administering drugs before surgery (neoadjuvant therapy) then monitoring to see how the cancer responds before adding more treatments. “This often can lead to a smaller surgery,” says Dr. Stover. You can also tailor what additional medication is needed based on how the cancer responds.”
Another example is a trial featured at ASCO 2022 which determined a group of women aged 55 and over who don’t need radiation therapy after a lumpectomy which, until now, had been common practice.

Liquid biopsies
Instead of the conventional needle biopsies, liquid biopsies involve drawing blood from a patient to see if there are any circulating tumor cells or circulating tumor DNA. More cells and more DNA circulating in the blood means that the cancer is still there. Liquid biopsies can also be used to gauge response to treatment.
“We’re doing better job of detecting cancer cells in circulation. There’s accumulating data that certain thresholds indicate a worse prognosis, but in isolation we don’t have sufficient data to learn how to use this in clinical decision making,” says Dr. Nasrazadani.
The technology “isn’t ready for prime time,” says Dr. Baron. “But it’s an exciting idea.”
PARP inhibitors for BRCA mutations
According to the Centers for Disease Control and Prevention, about one in 500 women with breast cancer have an inherited gene mutation known as BRCA 1 or 2 which greatly increases the odds of developing breast (and ovarian) cancer. The mutation interferes with a cell’s ability to repair itself. Drugs known as PARP inhibitors may be able to help.
Although the class of drugs have been around, researchers have more recently recognized their potential for treatment BRCA tumors, says Dr. Gralow, adding that they’ll likely be found to benefit even more people in the future. And And unlike many other therapies (including Enhertu, which is given by infusion), PARP inhibitors such as olaparib (Lynparza) are available in pill form.
5 Surprising Facts You Didn’t Know About Breast- and Ovarian-Cancer Genes

Prioritizing quality of life
Alternative treatments that patients have sworn by for decades now have evidence to support their effectiveness, so much that new practice guidelines from ASCO and the Society for Integrative Oncology now recommend the use of acupuncture for cancer pain, as well as massage for reducing pain and improving quality of life for people with advanced cancer receiving hospice or palliative care.
Palliative care which, unlike end-of-life hospice care, provides medical care for people living with severe illness. “We have all of these patients with metastatic breast cancer surviving for long periods, and palliative care is about quality of life,” says Dr. Gralow. “We’re focusing on quality of life no matter what the stage.”

Eliminating disparities in breast cancer care
Despite many advances in treatment, screening and diagnosis, disparities remain. For instance, Black women are 41% more likely to die from breast cancer than white women, making it the leading cause of death in this group, according to the American Cancer Society. They’re also more likely to be diagnosed with aggressive and hard-to-treat tumors.
But there are initiatives in the works. Epidemiologists at Boston University have developed the Black Women’s Health Study Breast Cancer Risk Calculator to help estimate a Black woman’s odds of developing breast cancer and when to start screening. “Instead of a single strategy for screening for all women, it’s becoming tailored in parallel with treatment,” notes Dr. Stover. “The [standard] screening guidelines may not be right for everyone.”
Racism in Healthcare: What It’s Like Giving Birth As a Black Woman
Representation in clinical trials
There are also efforts underway to recruit different racial and ethnic groups into clinical trials. “There has been a sea change in that we’re now ensuring that representation in studies is compatible with what is represented both in the U.S. and the world,” says Dr. Stover. “We’re finding ways to ensure that everyone has the same opportunity to get good outcomes.”
For more wellness updates, follow The Healthy on Facebook, Instagram, and Twitter. Keep reading:
