Tips for living with diabetes
Making necessary lifestyle changes is essential for anyone who has just been diagnosed with diabetes, whether you have type 1 or type 2 diabetes. First you need to nail down the basics, like medication.
If you’ve been diagnosed with type 1 diabetes, an autoimmune condition, you will have to track your blood sugar closely and take insulin to survive. If you have type 2, which is far more common, you may be able to control your blood sugar with diet, exercise, weight loss, oral medications, or insulin, if necessary.
In fact, transforming your life to gain control of your blood sugar can help you live well with diabetes. Here are some important life-saving changes you can make.
Be first on line for your flu shot
Any infection, including the flu, can wreak havoc on blood sugar levels and diabetes control, according to Joseph A. Aloi, MD, the section chief of endocrinology and metabolism at Wake Forest Baptist Medical Center in Winston-Salem, North Carolina.
“If you’re living with diabetes, infections can lead to more complications, and if you are hospitalized, your hospital stay will be longer than people without diabetes, so the key is to prevent infections in the first place.”
People living with diabetes should get the flu shot and get it early, he adds. Flu season in the United States can begin as early as October and last as late as May. Also, talk to your doctor about shots for pneumonia and hepatitis B prevention.
“Wash your hands. Wash your hands. Wash your hands,” adds Davida F. Kruger, a nurse and diabetes expert at Henry Ford Hospital in Detroit, and the author of The Diabetes Travel Guide. “If you want to stay healthy, carry hand sanitizer with you wherever you go in case you can’t access a sink.” (If you’re working on prevention, learn 12 surprising habits that can increase the risk of type 2 diabetes.)
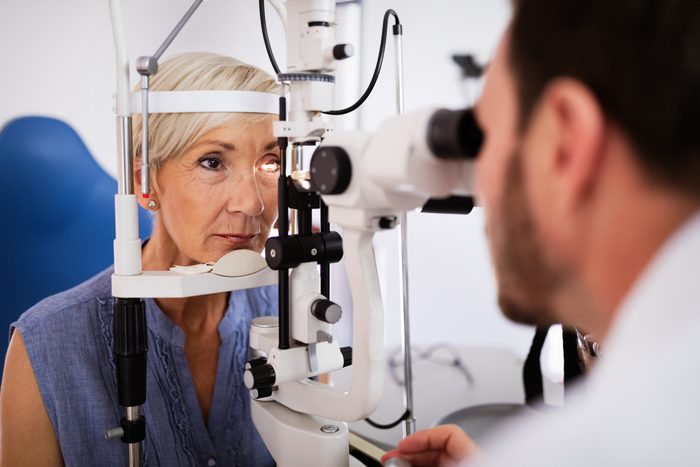
Get regular eye exams
See your eye doctor yearly for a comprehensive dilated eye exam. “If we catch eye changes early, we can prevent further damage,” Dr. Aloi says. “Diabetes is still the leading cause of adult blindness and it is largely preventable.”
Unfortunately, this message doesn’t seem to be getting through. Some 58 percent of people with diabetes did not have regular follow-up eye exams, according to research presented at the 2016 annual meeting of the American Academy of Ophthalmology in Chicago. These vision screens can catch diabetic retinopathy, which is caused by changes in the blood vessels of the retina and often has no symptoms. Other diabetes-related eye diseases that can be spotted during a yearly eye exam include macular edema (the buildup of fluid in the macula, a small area in the retina), cataracts (clouding of the lens), and glaucoma (a disease affecting the main nerve in the eye).

Be prepared for hypoglycemia
Blood sugar dips happen, so people living with diabetes should be prepared. Hypoglycemia, or a drop in blood sugar, can happen if you are taking insulin or other types of medication that can accidentally lower blood sugar too much.
“Keep a small cake icing tube in your pocket or bag in case you experience low blood sugar,” Dr. Aloi says. “Cake icing is discreet and doesn’t go bad.” Glucose tabs can also help if your blood sugar dips, he says. Other options for treating hypoglycemia include four ounces (1/2 cup) of juice or regular soda, 1 tablespoon sugar, honey, or corn syrup, or 8 ounces of non-fat or low-fat milk, according to the American Diabetes Association.
Signs of dropping blood sugar include sweating, hunger, and confusion. Catching and treating low blood sugar before it drops too steeply can save your life and prevent a diabetic coma. “If low blood sugar happens frequently, see your doctor to make sure you are on the optimum treatment regimen,” Dr. Aloi says. (Here are some helpful hints for eating breakfast as a diabetic to keep your blood sugar levels stable throughout the day.)

Take a walk
Regular exercise is an important way of managing type 2 diabetes and controlling weight, but it doesn’t have to be vigorous or joint- pounding to count. Just getting up off the couch and standing every so often or taking a walk can also improve blood sugar control, according to a study in Diabetologia.
“A 15-minute walk in the morning and a 10-minute walk during your lunch break will help with diabetes control,” Dr. Aloi says. “Aim for 25 minutes of moderate aerobic activity five days a week, and build from there,” he adds. Be mindful of which shoes you wear and follow this foot care advice for people with diabetes.
The American Diabetes Association recommends at least 150 minutes of moderate aerobic exercise per week and two sessions of resistance exercise, as a combination of aerobic and resistance training can improve blood sugar levels as well as other markers of diabetes disease activity, according to a study in the July 2015 issue of the Journal of Physical Therapy Science.
As a bonus, this same physical activity program improved heart disease risk factors, and diabetes is a major risk factor for heart disease.

Fill up on fiber
“You want to eat fewer carbs and more fiber to slow the absorption of carbs,” Dr. Aloi says. Here’s a trick for people living with diabetes: “Sprinkle some Benefiber, a 100 percent natural fiber supplement, on rice to slow the absorption of the carbs, so they have less of an impact on your blood sugar,” Aloi says. “It’s tasteless and just blends in.”
A 2000 study in the New England Journal of Medicine found that people with type 2 diabetes who ate 50 grams of fiber a day were able to control their blood glucose better than those who ate far less.

Be on the lookout for surprising causes of high blood sugar
Some “healthy” foods such as bananas can rapidly push blood sugar up, according to Deborah Malkoff-Cohen, RD, a nutritionist and certified diabetes educator and insulin pump trainer in private practice in New York City.
“A banana has as many carbs as two slices of bread,” she says. Other surprising foods that can spike blood sugar include flavored Greek yogurt, ketchup, and barbecue sauce. However, the reaction to any particular food can be individual; you can test your blood sugar after eating a specific food to see how you react.
“Look at carbs and sugar on food labels, and if they are close in number, don’t eat that food,” she says. (Here are 12 more rules to follow to keep your blood sugar steady.)
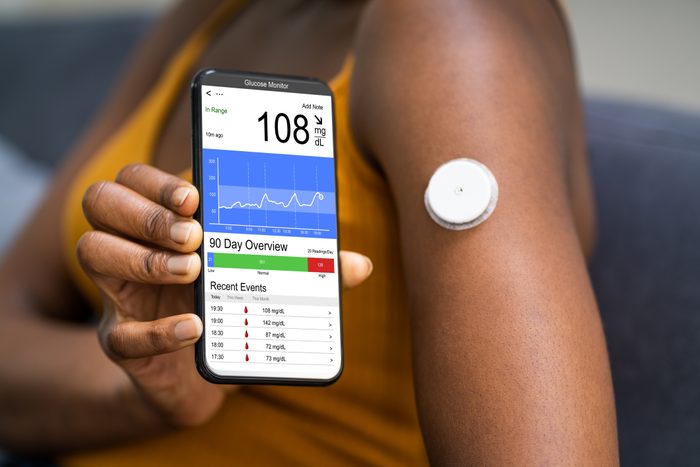
Use apps and other technology to manage diabetes
Apps can be a huge help for people living with diabetes when it comes to health tracking. “Find an app that helps tracks your diet, activity, and blood sugar,” Dr. Aloi says. Many even allow you to scan the bar codes of foods to find out their carb content.
“You can share all of this information with your doctor so that he or she has a better handle on how well your diabetes is controlled and can make any needed adjustments to your treatment.” He recommends MyFitnessPal, but there are many others that also do the trick.

Be kind to your kidneys
When your blood sugar is too high for too long, it taxes your kidneys, making them work extra hard. Over time, your kidneys will begin to leak protein, setting the stage for kidney disease and kidney failure. Diabetes is actually the leading cause of chronic kidney disease and kidney failure in the United States, according to the National Institute of Diabetes and Digestive and Kidney Diseases.
The best way to prevent this is to get a yearly screening for estimated glomerular filtration rate (eGFR) and urine albumin, Malkoff-Cohen says. Keeping blood pressure under control also helps slow the development of kidney disease. And since high blood pressure also ups risk for heart disease, this is a win-win for your health and well-being. (Here’s more on the risks of diabetes and high blood pressure.)
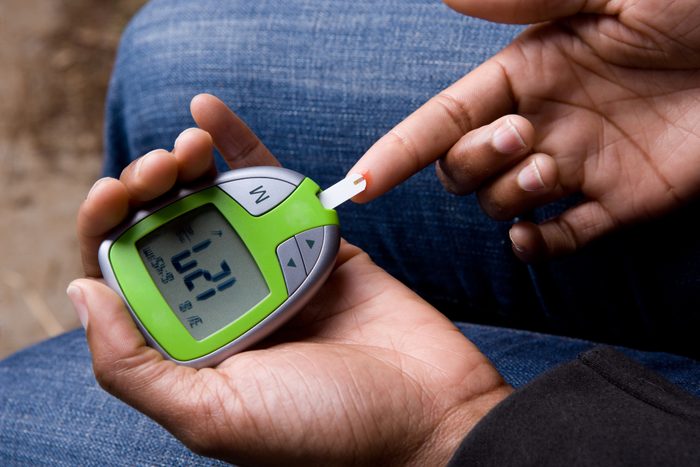
Know your numbers
How often should you check your blood sugar? There is no one-size-fits-all answer to this question, Malkoff-Cohen says. If you have type 1, you often need to test your blood sugar multiple times a day; if you have type 2, it’s usually less often, and sometimes not at all. It can depend on your blood sugar control and medication, so check with your doctor.
You should also see your doctor every three months for blood work that will give you a better idea of your blood sugar control (A1C) over time, Malkoff-Cohen says. If you do check your blood sugar, a common way to do so is by pricking your finger to obtain a drop of blood, putting it on a test strip, and using a blood glucose meter to check it.
If you’re living with diabetes and your blood sugar is out of control, a continuous glucose monitor can help, she says. It tracks your blood sugar levels 24-7, collecting readings automatically every 5 minutes. (Watch out for these other clear signs you could have high blood sugar.)
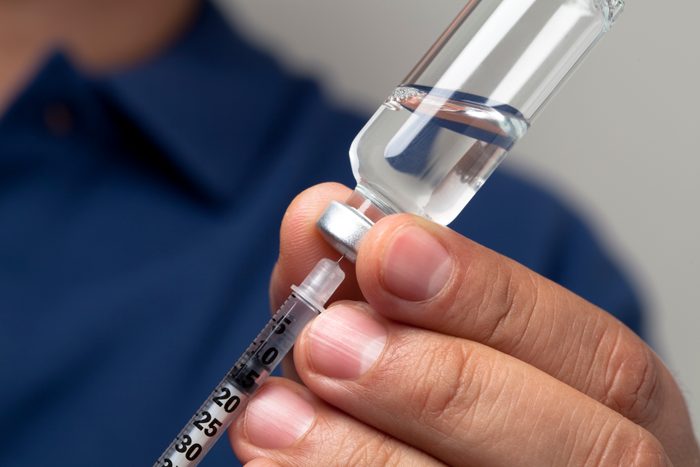
Mind the expiration dates on insulin
If you’re using insulin injections to control your diabetes, pay attention to the expiration dates, Malkoff-Cohen says. Using expired insulin can jeopardize your health and diabetes control, as it is less potent. Insulin is tasked with keeping blood sugar levels normal, so when it’s not doing its job, glucose levels build up and can cause health problems.
“Always read the fine print,” she says. There are typically two dates to check: Unopened and opened. “The moment you open a bottle or pen of insulin from the refrigerator, it should be discarded exactly 28 days later,” Malkoff-Cohen says. (Don’t miss these 9 ways you could help reverse diabetes.)

Put your best feet forward
“If you’re living with diabetes, you need really good foot care, including a yearly exam from a podiatrist,” Kruger says. Diabetic foot ulcers can occur in approximately 15 percent of patients with diabetes, and 6 percent of those who develop a foot ulcer will be hospitalized due to infection or other ulcer-related complications, according to the American Podiatric Medical Association. Here’s foot care advice for people with diabetes.
People with diabetes may lose feeling in their feet due to nerve damage, so if they do develop a blister from poor-fitting shoes and they don’t know it, it can turn into something bigger.
Don’t go barefoot, and always keep feet protected to reduce the risk of cuts and scrapes, which can lead to complications, the APMA states. Plus, try these 15 things diabetes doctors do to keep their own blood sugar under control.

