Do you have prediabetes?
If you are a borderline diabetic, it means you have prediabetes. Your blood sugar levels are higher than normal, but not enough to be diagnosed with full-blown type 2 diabetes. Maybe you’ve noticed that you’re losing weight or more tired than normal. Or perhaps you’re thirsty or have vision issues. Here’s a look at some of the more common signs that you could be a borderline diabetic.

You’re really thirsty and are peeing a lot
“Prediabetes is caused when the body is unable to efficiently process blood sugars,” says endocrinologist Dr. Jason Ng, MD, clinical assistant professor of medicine at the University of Pittsburgh. “This happens over time as the body builds up resistance to insulin, the hormone that helps the body control blood sugars.” As you become insulin resistant, the body has to produce more insulin to keep blood sugars at a good level. Eventually it can’t keep up, so blood sugars rise. Prediabetes may take you by surprise, as there often aren’t symptoms—though there are a few subtle cues you can look out for. “A patient may feel slightly more thirsty and have to urinate more over time as well as the sugars increase in their body,” Dr. Ng says.

You’re exhausted
Borderline diabetes could be one of the medical reasons you’re tired all the time. If you’re one of the 88 million Americans (that’s more than 1 in 3) who have prediabetes, according to the Centers for Disease Control and Prevention (CDC), you may notice you’re not feeling up to your normal activity level. “Patients may feel more tired or sluggish,” Dr. Ng says. Blood sugar fluctuations can cause fatigue; plus, other factors that often appear with blood sugar problems could be the culprit, such as depression or obesity, according to a study published in 2012 in Diabetes Educator.
Physical activity is recommended by the American Diabetes Association to help with prediabetes symptoms, but ironically people with the condition may be too tired to exercise. If that’s the case, see your doctor. “Most of prediabetes is diagnosed by lab work at a doctor’s office,” Dr. Ng says. With prediabetes, “fasting sugar is between 100 to 125 mg/dl or a random blood sugar between 140 to 200 mg/dl.”

You’re losing weight
Among the silent diabetes signs you might be missing is weight loss. Although we associate blood sugar problems with being overweight, once you start becoming borderline diabetic you may actually drop pounds. If you’re going to the bathroom more frequently, you’re excreting extra sugar and losing more calories. Diabetes may also keep sugar in your food from reaching your cells. This might leave you “feeling hungry all the time,” says Deena Adimoolam, MD, assistant professor of medicine, endocrinology, diabetes and bone disease at the Icahn School of Medicine at Mount Sinai. So if you’re eating more than usual and still losing weight, talk to your doctor.

You have blurred vision
One of the clear signs you have high blood sugar is actually not seeing clearly. Dr. Adimoolam says that blurred vision is a sign that you’re borderline prediabetic. Why? Diabetic eye disease occurs when high blood sugar causes damage to the blood vessels in the eye, which can leak and swell, leading to vision changes. According to the National Eye Institute, one type of eye damage, diabetic retinopathy, is the leading cause of vision loss among people with diabetes and the leading cause of blindness among adults. A study by The Diabetes Prevention Program (DPP) found that 8 percent of prediabetic participants had diabetic retinopathy. It can be addressed if caught early, so bring up blurry vision to your doctor as soon as you notice it.
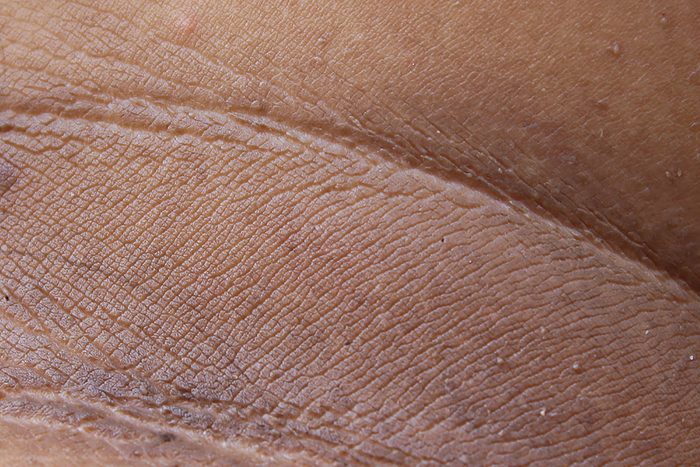
You have dark areas on your skin
One body changes that could signal a bigger problem that you are borderline prediabetic are dark patches on your skin called acanthosis nigricans (AN). According to the American Academy of Dermatology, it could be an early warning sign of prediabetes. The condition usually appears in elbows, armpits, knees, or on the neck, has a velvety texture, and likely occurs because excess insulin causes a rapid growth of cells. It’s also more common in people with obesity—another risk factor for prediabetes. But a study published in the Annals of Family Medicine showed that although patients with AN tend to have multiple risk factors for diabetes, AN itself may also be an independent risk factor for the disease. Because of this, AN’s presence may help doctors detect prediabetes sooner.

You have PCOS
Polycystic ovary syndrome (PCOS) is a disorder where a woman’s hormones are unbalanced. Studies like, one published in the Journal of Clinical Endocrinology and Metabolism in 2017, have shown that PCOS is a risk factor for diabetes.
According to the American Diabetes Association, it’s not known exactly how they are linked, but researchers are looking into the connection between PCOS and insulin. High levels of insulin may contribute to increased production of male hormones called androgens, which is a symptom of PCOS. PCOS is also associated with being overweight, as is prediabetes—but studies have shown that even average-weight women with PCOS are at increased risk of high blood sugar. Also, women with PCOS may be more likely to have gestational diabetes (diabetes while pregnant; more on that later), which also can lead to an increased risk of type 2 diabetes. If you are diagnosed with PCOS, your reproductive endocrinologist may test your glucose level to make sure you’re not borderline prediabetic.

You don’t get good sleep
“When you don’t get enough sleep, less insulin is released in the body,” says sleep expert Richard Shane, PhD, behavioral sleep therapist and creator of the Sleep Easily method. “Sleep deprivation can cause insulin-producing cells to fail to use the insulin efficiently or to stop functioning. Your body also secretes more stress hormones, which interfere with insulin’s ability to be effective.” In one study, duration and quality of sleep was shown to be associated with prediabetes. Another factor could be that we tend to crave calories and junk food for energy when we’re tired—plus, we don’t feel like exercising. This can lead to inactivity and weight gain, other risk factors for prediabetes.

You have a family history of diabetes
Among the medical facts you should know is your family’s health history. “There can be a genetic cause for the development of type 2 diabetes due to certain gene mutations,” Dr. Adimoolam says. “Some people may have a genetic predisposition to developing type 2 diabetes due to presence of certain genes than have been passed down from one generation to the next.” One study in Diabetologia found that a family history of diabetes increased the risk for prediabetes by 26 percent. The National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) says that you’re more likely to develop diabetes if you have a family history of the disease. In addition, “Some data suggests that the risk of type 2 diabetes is five times higher in those with diabetes on both the maternal and paternal sides of the family,” Dr. Adimoolam says.

You’re of a certain age
There are many reasons why you’ll age better than your parents, including that you know age itself is a risk factor for certain conditions—so you’ll take measures to prevent them. Unfortunately, prediabetes is more likely in older people. “The higher your age, the greater risk for development of diabetes,” Dr. Adimoolam says. “This might be related to increased body fat with age, which increases one’s risk for type 2 diabetes.” In addition, Dr. Ng says that high blood pressure and high cholesterol are also risk factors for prediabetes. These are all common conditions as we age, and are also associated with metabolic syndrome, a cluster of disorders that can lead to heart disease and stroke.

You had gestational diabetes
Having had gestational diabetes in the past also puts you at risk for prediabetes now, according to research, including a study in BMC Pregnancy and Childbirth. “Once you have been diagnosed with any form of diabetes, like gestational diabetes, you are at increase risk for developing this again over time, especially with weight gain,” Dr. Adimoolam says. According to the American Diabetes Association, doctors don’t know exactly why gestational diabetes develops, but it could be that pregnancy hormones affect how the body uses insulin. The NIDDK suggests women who’ve had gestational diabetes have their blood glucose tested every three years.

You’re overweight
You can potentially reverse type 2 diabetes if you lose weight—and the same goes for if you are borderline diabetic. “By and large, obesity is the main cause of insulin resistance, as certain fat cells are known to cause and intensify insulin resistance over time,” Dr. Ng says. And it’s not just how much you weigh, but where your weight is located on your body. “Waist size is typically proportional to centralized, or abdominal, obesity,” Dr. Adimoolam says. “The more centralized abdominal fat, the higher one’s insulin resistance, and the greater the increased risk for the development of type 2 diabetes.” Genetics may also play a role here, as certain body types with more abdominal fat (“apple-shaped”) can run in families and certain ethnic groups, she says.

You have an unhealthy lifestyle
Whether your are borderline prediabetic or not, there are many science-based reasons to start working out. “Lack of exercise may promote weight gain, which is a risk factor for type 2 diabetes,” Dr. Adimoolam says. A study from Johns Hopkins published in the Journal of General Internal Medicine showed that people with prediabetes who dropped 10 percent of their body weight dramatically reduced their risk of diabetes—but every little bit helps.
Dr. Ng suggests losing even 5 to 7 percent of your body weight, quitting smoking, and adopting a borderline diabetic diet. “Interventions that typically reduce weight include increased exercise, especially aerobic exercise, 150 minutes or more per week, and eating a balanced, low-fat diet that is not heavy on carbs,” he says. “Prediabetes is often thought of as a ‘warning sign,’ which is why lifestyle intervention is so important.”
Ultimately, the message is that prediabetes is not irreversible. “Prediabetes is the stage before one develops type 2 diabetes, and in most cases is preventable,” Dr. Adimoolam says. “You may not need medications to treat prediabetes if you are able to change your lifestyle, with the goal for treatment focusing on diet changes and exercise.”
