8 Causes of Calf Pain
Updated: Mar. 30, 2022
Calf pain can come from a range of different causes. Here's what to know so you can prevent it, spot it, and treat it.
Calf pain 101
When someone says they have calf pain, that typically means they’re experiencing aches or discomfort on the back of the lower leg, says Naimish Baxi, MD, assistant attending physiatrist at the Hospital for Special Surgery in New York City.
While people experience pain in the calf for many reasons, we asked experts to break down some of the most common calf pain causes. From overuse injuries to more serious health issues, here’s what can lead to discomfort in the lower leg, how to recognize when it’s time to see a doctor, plus the anatomy of the calf.
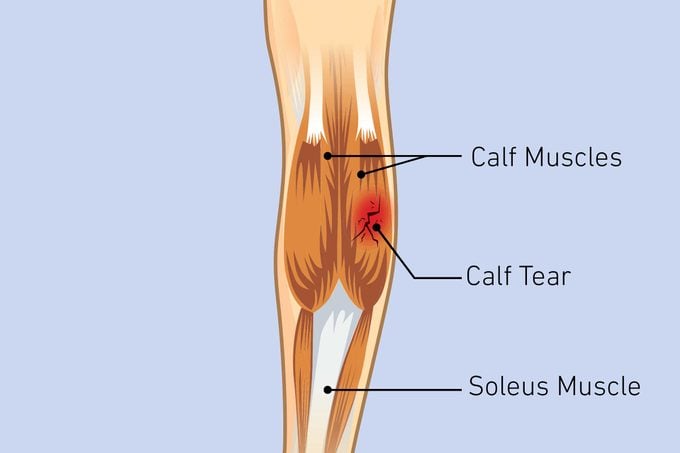
The muscles of the calf
Two main muscles make up what most people refer to as the calf—the gastrocnemius and the soleus, also known as your plantar flexors, Dr. Baxi explains. The muscles’ primary job is to plantarflex the ankle joint or bend the ankle downward, away from the body (what some people call pointing your toes). You perform this motion in everyday movements like walking, running, and jumping. Some people also consider the Achilles tendon, and the muscle fibers around it, as part of the calf, Dr. Baxi says. The muscles on the back of the upper leg, namely the hamstrings, while a different muscle group, can also affect how your calves feel, as can the feet.
Now that you have the anatomy down, here are the reasons you might experience calf pain.
Common reasons for calf pain
 Muscle cramps
Muscle cramps
Muscle cramps—you might know them as charley horses can definitely cause pain in the calf. Typically, these occur because your muscles get too overworked too quickly, says Dr. Baxi, which is why you might see some pro athletes get sidelined for cramping. “The muscles will tighten up and spasm and then not work the way you want them to,” he explains.
Many times, muscle cramps can also stem from dehydration, says physical therapist Colleen Louw, PT, spokesperson for the American Physical Therapy Association and co-owner and lead physical therapist at Ortho Spine and Pain Clinic in Iowa. So, make sure you’re drinking plenty of water throughout the day and especially around physical activity. (Here are the sneaky causes of dehydration.)
You’ll know you have a muscle cramp versus another type of pain if it lasts for just a few seconds or minutes, Dr. Baxi says. Often, these cramps resolve on their own.
 Overuse injury
Overuse injury
If you’re running often or for long distances, you’re at a greater risk for overuse injuries, like Achilles tendinopathy, which can cause calf pain. According to at least one scientific review in the Montenegrin Journal of Sports and Science Medicine, this is one of the most common injuries for runners,
Plantar fasciitis is another common overuse injury. Though it mostly causes pain in the foot, it can also lead to some discomfort in the calf (they’re all connected, after all, says Dr. Baxi). People who often do plyometric moves like jumping exercises also have an increased risk of these overuse injuries, Dr. Baxi adds.
Overuse injuries are more cause-and-effect, meaning you experience pain as you kick up your training volume, says Louw. This is especially true for people who run on their toes, instead of striking at the midfoot or heel, as this gait puts more strain on the calf muscle. (Here are the signs you’re working out too much.)
“Any time you’re overusing your muscles and not giving them enough time for restoration, they can become fatigued or weakened,” Louw says. “You then compromise the tissues, and sometimes the tendons can fail, because they’re too stressed for too long.” This may also raise your risk of a calf tear—a rip in the muscle fibers.
To avoid overuse injuries, you not only want to give yourself enough rest time between workouts, but you also want to make sure you warm up properly before a workout and cool down after, too, according to both Louw and Dr. Baxi. (Is stretching before a workout essential?)
Dr. Baxi says it’s particularly important to stretch after your workouts. Focus on static stretches (in which you hold a pose for about 30 to 60 seconds), like touching your toes. Another good option: Stand about a foot-length away from the wall, facing it. Then, try to get your knee to touch the wall, while still keeping your heel on the floor. This stretches the Achilles and the muscle fibers that surround it, Dr. Baxi says. You also want to make sure you have enough strength in your lower body to carry you through runs and plyometrics. For more ideas, check out these other calf stretches everyone needs.
Sciatica
Louw says calf pain can also come from back issues such as spinal stenosis—pressure placed on the spinal cord’s nerves, particularly those that travel to your muscles. This pain is known as sciatica and can lead to pain showing up in both calves. “When someone has calf pain, I always check to see if they have a history of back issues,” Louw explains. Looking at the health history of the back often gives clues into whether this pressure on the spine is what’s leading to calf pain. The pressure also tends to build up over time. (Here are the sciatica symptoms anyone with back pain should know.)
“If you stand too much or sit too much, you lose space between the spine and compromise blood flow to the nerves in the low back as gravity pulls on us all day,” Louw explains. To combat that pain—before spinal stenosis becomes a serious issue—you want to make sure you move more. Louw says that turning to swimming will help unload the spine and promote blood flow, but even just moving from standing to sitting more often (and adding in walks throughout the day) may help alleviate the pain. You can even start with just two to five minutes of movement every 20 minutes, she says. Pointing and flexing your toes or pumping your ankles will also help with that blood flow. “To function well, nerves need movement, space, and blood,” Louw adds.
Research in the Yoseni Medical Journal also found that lumbar spinal stenosis can lead to leg pain and increase the risk of nocturnal leg cramps. While factors like more exercise and frequent stretching helped to alleviate pain in those with lumbar spinal stenosis, according to the study, surgery was the best option for stopping the nocturnal leg cramps.
Blood clots
Known technically as deep vein thrombosis, this condition often starts as a clump of blood deep in the calf. It can then travel up through the body and lead to a blockage in the arteries of the lungs, leading to a life-threatening pulmonary embolism, Dr. Baxi explains. If someone goes to the doctor complaining of calf pain, this is the first condition they’d aim to rule out, he adds.
If you experience calf pain from a blood clot, you might also experience redness, swelling, and a warm sensation on the calf, Louw explains. Usually, this pain is unilateral (on only one leg), and it signals you should go to the doctor immediately.
Diabetic neuropathy
Louw mentions that people who have diabetes may also experience calf pain. High blood glucose levels and high levels of fat in the blood (both a result of diabetes) can cause nerve damage—known as diabetic neuropathy, according to the National Institute of Diabetes and Digestive and Kidney Diseases, and lead to discomfort in the calves. Peripheral neuropathy, in particular, can affect the feet and legs, as well as the hands and arms, and trigger pain. About one-third to one-half of those living with diabetes will have this condition.
Baker’s cyst
Calf pain can be a secondary issue to a Baker’s cyst, which often forms after an ACL or meniscus injury at the knee, or from conditions like arthritis. These problems lead to fluid build-up in the knee joint which can accumulate, thicken, and form a cystic structure on the back of the knee, Dr. Baxi says. This cyst can sometimes pierce out of the knee joint and settle into the gastrocnemius muscle head (one of the muscles of the calf), which is why you’d experience calf pain.
Doctors typically spot this condition with a thorough exam, which would involve looking and touching the area of concern, and testing to see if it feels tender or inhibits the range of motion.
Varicose veins
Varicose veins are enlarged veins that are purple or blue in color and seen right beneath your skin. They typically affect your legs and feet, so they may be a cause of calf pain. Symptoms include muscle cramps, as well as swelling in the calves. Warm weather may aggravate them as blood vessels dilate in higher temperatures. Long periods of sitting may also worsen calf pain from varicose veins because being in one position for a long time puts extra pressure on the veins, per the American Society of Dermatological Surgery. Elevate and stretch your legs for pain relief and consider investing in compression socks to help with swelling, too. (Check out the best compression socks that experts recommend.)
Compartment syndrome
This potentially dangerous condition causes pressure to build up in the connective tissue that contains the muscle. Compartment syndrome can happen after a serious injury to the calf muscle or the bone. The symptoms can be severe pain that doesn’t respond to pain killers or ice, numbness, and unusual bulging in or around the calf. For severe cases, you may need emergency surgery.
When to see a doctor for calf pain
If you experience persistent pain that lasts for hours or days, that should be alarming enough for you to get checked out, Dr. Baxi says. Also, if the pain feels so severe that it affects other areas of your life, that’s always a sign to see a professional.
For those who experience pain that’s not so severe, but have other comorbidities, like an increased risk of blood clots, it’s also smart to see a doc. “That might not cause debilitating pain, but in the context of other health issues, it’s probably time to get checked out,” Dr. Baxi says.
Of course, visible swelling, bleeding, or bruising—especially where a tendon, like the Achilles, attaches to the bone—are also signs you need medical attention, along with problems like weakness or an inability to move a joint, like the ankle, Dr. Baxi says. Finally, if the pain comes episodically, say every hour, that means it’s time to ring a doc, too.
Now that you know the causes of calf pain, check out these proven remedies for fast pain relief and the best moves to end knee pain.