What Is Post-Inflammatory Erythema? These Post-Acne Red Spots Aren’t Scars
Updated: Apr. 12, 2021
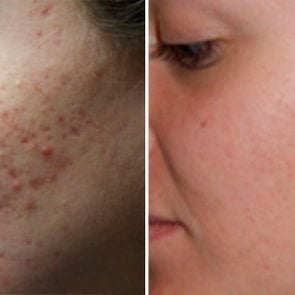
Post-inflammatory erythema is the red or pink spot that forms after a pimple is gone. Here's are the treatments that can help you get rid of these post-acne red spots.
The aftermath of acne
Finding a skin care and treatment routine that limits acne breakouts is a challenge, and it can take lots of trial and error to get it right. Once you do have yours down-pat and acne is under control, it can feel like you hit the complexion jackpot.
That said, many people will still have acne scars and lingering marks that are reminders of pimples past.
One type of mark you may not realize you have is post-inflammatory erythema (PIE).
Here’s what dermatologists want you to know about how these marks form, why they’re not “true” acne scars, and the best ways to prevent and treat them.
What is post-inflammatory erythema (PIE)?
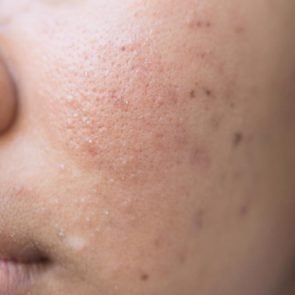
Post-inflammatory erythema is the red or pink spot left over after an acne spot fades away. It’s flush with the skin, so there’s no acne bump. (Erythema means a reddening of the skin.)
According to board-certified dermatologist Morgan Rabach, MD, of LMMedical in New York City, it’s more likely to occur in lighter skin tones, although it can happen to anyone.
“It’s caused by dilated blood vessels on the area of the pimple,” she says.
Damage to the capillaries (small blood vessels near the skin’s surface) results in these red spots. The term PIE is relatively new in the world of dermatology and only dates back to 2013, according to the Journal of Clinical and Aesthetic Dermatology. So there’s currently only limited research on the condition.
According to board-certified dermatologist Zain Husain, MD, founder of NJ Dermatology and Aesthetics Center, these hyperpigmented flat lesions do not “blanch” when touched.
A mark that blanches—the skin gets lighter after applying pressure because of the temporary obstruction of blood flow—isn’t PIE.
Is PIE an acne scar?
A true acne scar alters the collagen in the skin beneath the epidermis (the outermost layer of the skin), so Dr. Rabach would not consider PIE a true scar.
Dr. Husain agrees and explains that no scar tissue forms in the dermis (the skin layer under the epidermis) of the skin with PIE, another reason it’s not considered a true acne scar.
Still, some treatments for true acne scars overlap with PIE treatments. (We’ll get to those later.)
How to prevent PIE
Dr. Husain says his biggest tip for avoiding PIE is to treat the underlying process. That is, prevent acne in the first place.
Of course, avoiding acne is usually the goal, but it’s a sentiment worth repeating. It may be easier to avoid acne than it is to treat PIE. And never forget the golden rule: don’t pick your pimples.
UV radiation can exacerbate PIE, says Dr. Husain, so protect your skin by wearing a broad-spectrum sunscreen.
Dr. Rabach says topical antioxidants (think vitamins A, C, and B3) are another great way to prevent PIE. Niacinamide (vitamin B3), in particular, may help fight redness.
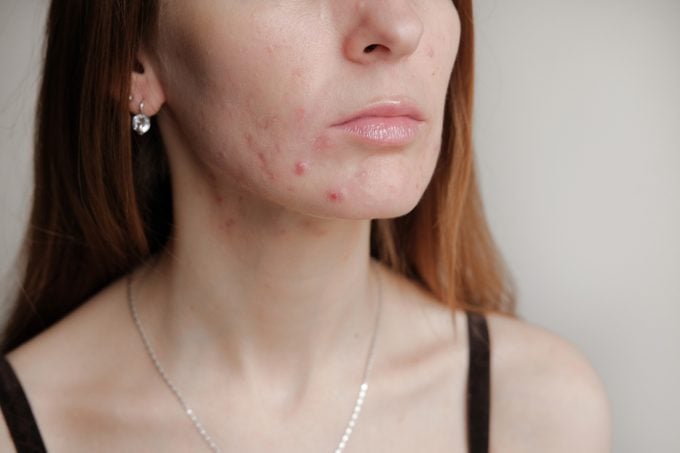
Treatments for PIE
Although PIE usually resolves over time, some topical and in-office treatment options help speed up the process. Here’s what you need to know.
Creams, serums, and other topicals
Antioxidants aren’t only for prevention. They can help treat PIE, too. Dr. Rabach recommends vitamin C to help repair damaged skin.
A study in the Journal of Cosmetic Dermatology found that a 5 percent vitamin C concentrate treated broken capillaries and decreased erythema. The researchers had 30 women between the ages of 30 and 60 apply the concentrate once a day. Erythema dropped by 9 percent after two weeks, 16 percent after four weeks, and 21 percent after six weeks using vitamin C.
There are other serums and creams that address PIE. Dr. Husain also recommends retinoids, hydroquinone, kojic acid, tranexamic acid, alpha and beta hydroxy acids, niacinamide, and steroids. (These products are also some of the best ones for hormonal acne scars.)
Another potentially good option is azelaic acid, an antioxidant known to reduce facial redness associated with rosacea. Although they are different skin conditions, rosacea and PIE are similar in that they cause redness due to blood vessels in the face.
So some experts theorize that skin care products that help improve rosacea may work similarly to help improve PIE. As of now that’s just a theory, and more research is needed to see if it pans out.
Sunscreen
There are a lot of reasons you should be wearing sunscreen daily.
If you have PIE, add this to your list: It can prevent additional discoloration.
Both sunscreen and physical blockers work, though the latter may be more helpful. The zinc found in most physical blockers has some anti-inflammatory properties, says Dr. Rabach. (Here’s what to look for in a sunscreen.)
Lasers
Getting a laser treatment at your dermatologist’s office may help heal PIE. Dr. Rabachs says lasers (mostly pulse dye lasers) target dilated capillaries.
A small study of 33 people in the Indian Dermatology Online Journal found that intense pulsed light therapy is a safe and effective way to treat PIE. So is an Nd:YAG laser, which is often used for tattoo removal, according to a small 2020 study in the journal Medical Lasers.
Lasers work by targeting damaged blood vessels deep under the skin and can reduce inflammation and discoloration, Dr. Husain says.
Before you drop cash on laser therapy, know that it may take several treatments before you start to notice results. (Did you know laser or light therapy also works for rosacea?)
Another small study in the Journal of Cosmetic and Laser Therapy compared fractional laser and pulsed dye laser for treating PIE on 12 Korean people. They did a “split-face study,” meaning one side of the face receive treatment with either a fractional laser or a pulsed dye laser (PDL). The other side of the face served as a control, receiving no laser therapy. The people did three treatments at four-week intervals.
Both lasers improved PIE. However, the people assessed their own skin and saw more improvement with the fractional laser. About 92 percent of participants who got the fractional laser treatment said their improvement was good or excellent, compared with 75 percent who got PDL treatment.
Other in-office options
An additional option is fractional microneedling. Research published in Advances in Dermatology and Venereology compared 25 people with PIE who had two fractional microneedling radiofrequency treatment sessions at four-week intervals with a control group of 27 people with PIE who used topicals or antibiotics.
They found that PIE improved in all 25 people who had the needling procedure, compared with just five of the 27 control group participants.
An additional in-office procedure is chemical peels, including salicylic acid and glycolic acid peels, which help reset skin and decrease inflammation, Dr. Rabach says.
The difference between PIE and PIH
Post-inflammatory hypo- or hyperpigmentation (PIH) is another mark left over from acne, but it’s different from PIE.
PIE is due to dilation and proliferation of blood vessels in the skin, Dr. Husain says. But with PIH, inflammation leads to a dark spot, or discoloration. “The melanin dropped into the dermis then stays as a brown spot that is leftover even after the acne has healed,” says Dr. Rabach.
Simply put, PIH is darkening of the skin, while PIE is reddening of the skin. And you can have both at the same time.
PIH often occurs in people with darker skin tones but, like PIE, it can happen in anyone. (Here’s the difference between melasma, sun spots, and other skin spots.)
The bottom line
Researchers and dermatologists are still learning more about PIE. In-office treatments like lasers, microneedling, and chemical peels may help reduce these marks. So can topicals like antioxidants, retinoids, hydroquinone, and more.
To prevent this post-acne mark, focus on treating and preventing acne. Always wear sunscreen and never pick at your skin.
PIE usually resolves over time. Meeting with a dermatologist, if possible, can help you find the right course of action for your skin.
Next, check out what you need to know about acne scar treatment.