What is psoriasis?
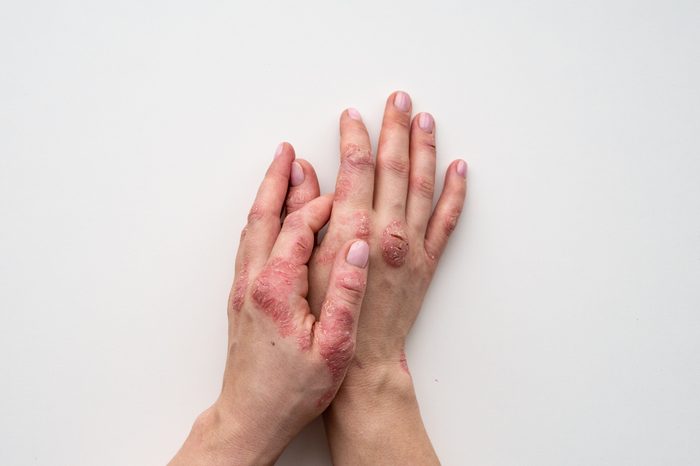
This very common skin condition is characterized by plaques—thick, scaly, itchy, red or silvery rashes that occur from cells building up rapidly on the surface of the skin. The trouble starts with the immune system: Overactive immune cells trigger inflammation in the skin, leading to the plaques. Psoriatic diseases, which include psoriasis and psoriatic arthritis, are some of the most common skin diseases, affecting up to three percent of the population, according to the National Psoriasis Foundation. This has serious implications—even though it’s often seen as a “skin” problem, it’s not just about appearances. Nearly two-thirds of people with psoriasis say it affects their everyday life, including causing chronic pain, embarrassment, and depression.
How do you find the right treatment?
This is why finding the right treatment for each individual is so important, says Cheryl Lee Eberting, MD, a board-certified dermatologist and CEO and founder of the healthcare site Azova. This can be trickier than it seems, however, as the treatment will depend on the type of psoriasis, the severity of the illness, the amount of body surface area affected, and the person’s overall health and lifestyle, she explains. “Mild cases can usually be controlled with topical treatments while severe cases usually require some sort of systemic immune suppression,” she says, adding that what works for one person may not work for someone else and it often takes a lot of trial and error.

Start with lifestyle interventions
After you’ve got a diagnosis but before you even think about medical treatments, you need to take a look at your lifestyle, Dr. Eberting says. “I always recommend lifestyle changes in addition to medical treatment because psoriasis is associated with obesity, type 2 diabetes, hypertension, coronary artery disease, and stroke,” she explains. “These diseases are all pro-inflammatory diseases and lifestyle modifications including weight loss, eliminating high glycemic [high-carbohydrate] foods, and eating anti-inflammatory foods can really make a difference in the treatment of psoriasis and other inflammatory diseases.” Examples of high-glycemic foods include white bread, white rice, cookies, crackers, and anything with a lot of sugar. Anti-inflammatory foods include healthy choices like fish, nuts, and green leafy vegetables.
You’ve got more options than ever
There are many ways to treat psoriatic diseases, including oral medications, systemic treatments, phototherapy, topical ointments, biologic or biosimilar injections or infusions, and a wide range of homeopathic or alternative options—or a combination of any of these. Here’s what you need to know about the newest psoriasis treatments. To help you figure out which options may be best for you, we talked to five people with different types of psoriasis about the best treatment for them and how they discovered it.

“I use a different topical cream for each body part”
Austin, Texas native Rebekah Jasso Jensen, 37, was officially diagnosed with plaque psoriasis in her early 20’s but last summer had an acute outbreak of guttate psoriasis, a type where the patches look like teardrops. “My main symptoms are plaque psoriasis on my right leg, scalp and it presents itself in the genitalia area, which no one wants to talk about but is fairly common,” she says.
In her quest to get relief for both types of psoriasis, she’s tried a lot of things, including oily creams on her scalp that required her to wear a shower cap for long periods of time. “I was in college so that was super embarrassing, definitely not a glamorous or relaxing beauty treatment!” she says.
Eventually, she settled on a regimen of different topical medications. “I use a topical steroid cream for my skin and a topical steroid liquid for my scalp plus hydrocortisone butyrate cream for my genital area,” she says. However, she cautions that she has had to learn to only use the topicals during an active outbreak as using them daily can cause them to lose their effectiveness. “Basically I use it until the symptoms go away—which can be days, weeks or months—then I stop and don’t use it again until it starts coming back.” (Check out more expert tips for managing genital psoriasis.)

What to know about topicals
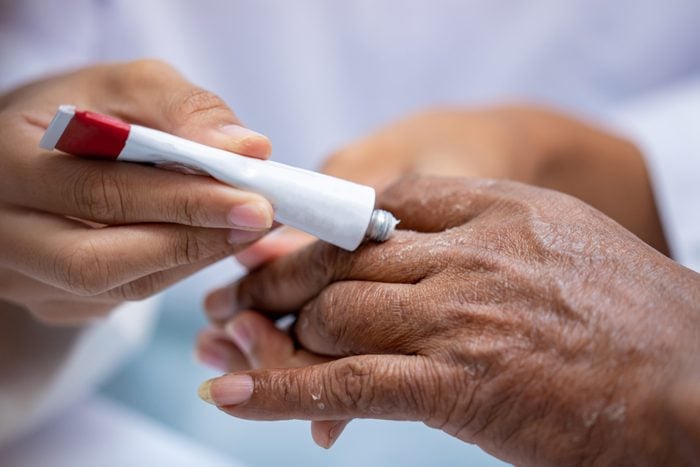
“I always prefer something topical over something systemic when it is feasible,” Dr. Eberting says. “Topical steroids, short contact retinoids, and Dovonex are the most effective and widely-used topical treatments.”
When using any medication but particularly topical oils or creams, it’s important to follow your doctor’s orders exactly, she says. “One of the most common mistakes that patients make when treating their psoriasis is under treatment,” she says. “For example, it is common for the instructions on the steroid tube to say to use it for only two weeks but this length of time is almost always too short when treating psoriasis.” A doctor who specializes in psoriasis can help you navigate this confusing territory, she says.
“I take a biologic medication”
Fifteen years ago Joel White, of Austin, Texas, started experiencing some strange skin symptoms. “I would get bad plaques, maybe a quarter-inch thick or more on my elbows, and when I would sit at my old chair, the arms turned white from the plaques just rubbing into them,” he says. “My elbows would crack and bleed all the time. It was miserable.” Even though he also had symptoms on his scalp, ears, and legs, it took until 2018 to get a proper diagnosis of plaque psoriasis, inverse psoriasis, and psoriatic arthritis. (Because men are less likely to get psoriasis, it often takes them longer to get a diagnosis, just one of the things all men need to know about psoriasis.)
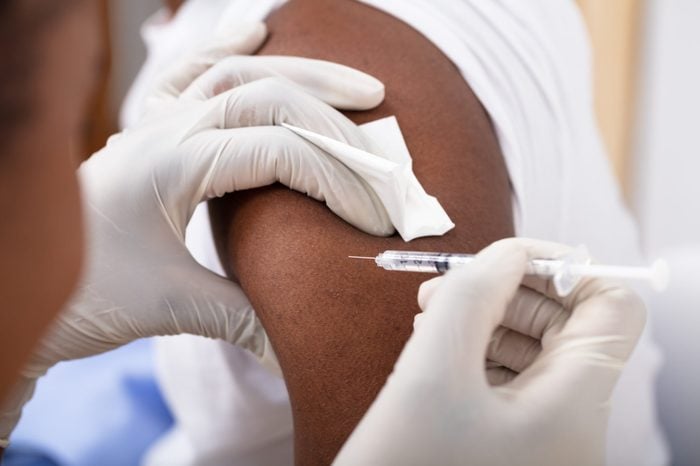
He’s tried many treatments over the years including dandruff shampoos; topical, injected, and oral steroids; and a myriad of different creams and lotions. While some were helpful—he says coal tar shampoo helps reduce itching—he wasn’t getting significant relief. Finally, last year his doctor convinced him to try Cosentyx, a biologic medication. Biologics are a relatively new type of medication that work by targeting specific inflammatory mediators of the immune system and are typically administered through an injection or infusion.
“I was a little hesitant at first to switch to a biologic and an injectable one at that but it has been really amazing, I am almost completely clear,” he says. “I itch very rarely, most of my plaques are gone. Where the worst of the plaques were, the skin had changed color, and after almost a year on it, the color is getting back to normal.”
What to know about biologics
“If your psoriasis is associated with joint pain and arthritis, it is important to get that under control as quickly as possible to avoid long-term joint problems,” Dr. Eberting says. “In this case, it is reasonable to use some form of systemic immune suppression. This can come in the form of methotrexate, acitretin, prednisone, or many of the newer biologic drugs.”
However, she notes that all of these medications come with risks and side effects so it’s important to discuss any concerns with your doctor and to report any new symptoms right away. While injecting himself has been easier than he anticipated, White says he does experience a major side effect—for several hours after his dose he feels like he has a terrible flu, with hot and cold flashes, stomach upset, and sweating. “It is not a good time at all, but then the next day I feel fine and it’s great,” he says. “For the results, it’s totally worth it.”

“I eat a Paleo diet”
“I watched my mom struggle with psoriasis as I was growing up so when my own scalp erupted in dry, flaky patches that itched uncontrollably, I knew immediately what it was,” says Chrissa Benson, 34, of Washington, DC. What she didn’t know, however, was how to deal with it and the unpredictable psoriasis flare-ups hurt her self-esteem and even disrupted her work productivity, she says. She was leery of harsh medications so she decided to try a natural approach first.
After reading about the link between eating inflammatory foods and inflammatory autoimmune illnesses, like some types of psoriasis, she decided to try eating a paleo diet. “After eliminating all grains and dairy from my diet, I finally experienced almost total healing from my once inflamed, itchy, and sometimes oozy scalp,” she explains. Four years later she’s still going strong and is now a wellness expert helping others use diet to reduce symptoms from inflammatory illnesses. “I still occasionally experience small flare-ups, usually due to stress, but blue tansy oil is enough to calm the irritated spots,” she adds. In addition, make sure you’re avoiding these seven foods that may worsen psoriasis.

What to know about alternative treatments
From oils to diet modification to massage, there are many non-medical and all-natural treatment options for psoriatic diseases. For mild cases, these may be enough to resolve the symptoms, like Benson was able to do with her diet. If they don’t provide enough relief on their own you can use them in conjunction with medical treatments but it’s important to discuss everything you are doing and taking—including supplements—with your doctor, Dr. Eberting says. You may also want to work your doctor and an integrative physician or naturopath to help you sort through the options.
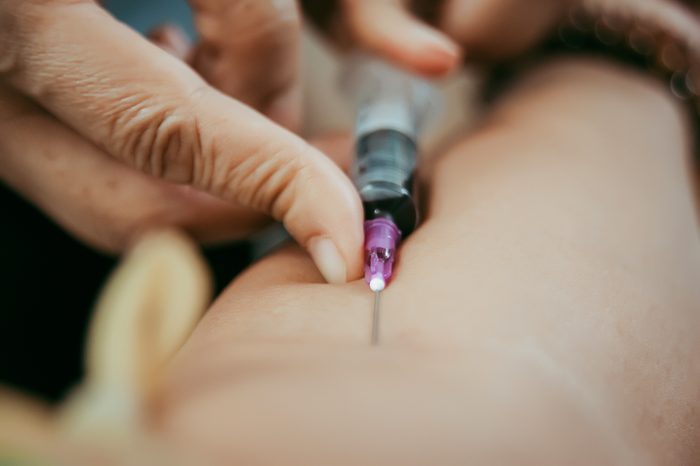
“I’m part of a drug trial for a new psoriasis medication”
At first, Ross Sundberg chalked up the red patches of dry, flaky skin to wearing a baseball hat and being in the sun too much while coaching his son’s baseball team. But when other people started commenting on his skin, he realized it was more serious. The 45-year-old dad from Minneapolis, Minnesota headed to a dermatologist who diagnosed him with psoriasis. He tried several different common medications, including methotrexate and Otezla, to treat it, but not only did they fail to ease his condition, but he also experienced terrible side effects. Then his doctor told him about a new drug currently being tested called Skyrizi (it’s now FDA-approved). His doctor was able to get him into the drug trial.
The drug worked wonders: Sundberg gets two injections of Skyrizi every three months and has seen remarkable improvements with few side effects. “Everything is so easy, they ship it right to my home or office, and giving myself the shots is easier than I thought it would be,” he says. “It only takes a few minutes every three months.” If you’re afraid of needles you can go to the doctor’s office to get the injections, he adds. “This was definitely the right drug for my psoriasis,” he says.
What to know about systemic treatments
The class of prescription drugs known as systemic medications can be either oral or injected; they work throughout the body. They are intended for people with moderate to severe psoriasis, particularly those who didn’t respond well to topical medications or UV light therapy, according to the National Psoriasis Foundation.
“If the body surface area affected is too large, it becomes rather difficult and unrealistic to treat psoriasis topically, so we turn to medications that work on the whole body,” Dr. Eberting explains. “The most common ones are methotrexate, acitretin, and prednisone; however, all of the systemic medications come with risks and side effects so talk to your doctor to decide if these are right for you.”
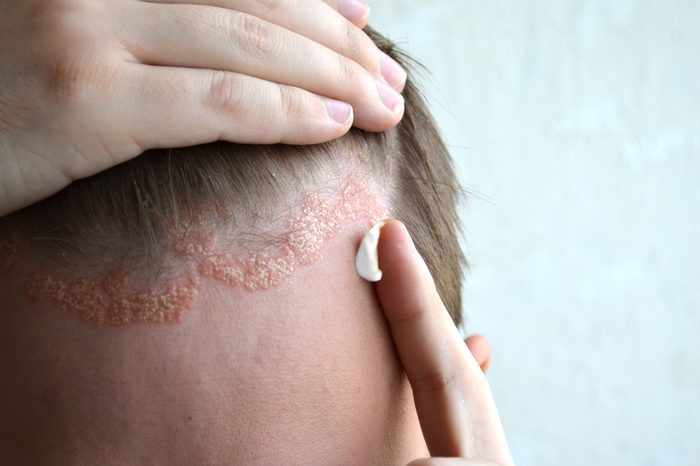
“I replaced a pricey brand-name drug with two affordable generics”
Scalp psoriasis has plagued Leslie Kasperowicz since childhood. Childhood scalp psoriasis is more common than most people realize and is often written off as dandruff or even lice—just a couple of the things dermatologists wish you knew about scalp psoriasis. So the Minnesota mother of two and managing editor at Expert Insurance Reviews has had years to try every remedy on the market. She found one drug, Taclonex, that helped manage her symptoms well but had to give it up due to the steep price tag of the brand-name prescription. Fortunately, she says she was able to find two generic ingredients that work just as well for a fraction of the cost.
“The best treatment I have found is a combination of clobetasol propionate (0.05%) and calcipotriene (0.05%) topical solutions,” she says. “Since they’re in an alcohol solution, they can sting a bit if the skin is irritated, but they aren’t at all greasy which is a bonus since I’m applying it to the scalp in my hair.” Here are the best shampoos for scalp psoriasis relief.

What to know about generic drugs
Dr. Eberting likes the strategy of using two different medications, adding that with some types you can alternate them to avoid losing effectiveness and maximizing the treatment while lengthening the time between flare-ups.
While generics can be a great option, she says, sometimes you will need the real deal. “I have noticed that the name-brand Dovonex seems to be more effective than the generic version that came out more recently,” she says. Pay attention to how your body responds to each new medication, including switching from a name-brand to a generic, and call your doctor immediately if something seems off. If you must have a name-brand drug but cannot afford it, your doctor or pharmacist may know of a program to help you get a discount or coupons.

