What to Do if You Have Genital Psoriasis
Updated: Jul. 06, 2021
Genital psoriasis can be difficult to manage, but there are treatments that can help.
What is genital psoriasis?
Psoriasis is a challenging skin condition for many reasons, but it can cause symptoms in one area of the body people may not want to talk about that often—the genitals.
But that doesn’t mean genital psoriasis is uncommon. Or that, if you have it, you’re alone.
In fact, the opposite is true.
As many as two-thirds of people with psoriasis will experience symptoms such as itching and raised red patches in their genital area at some point.
The symptoms can be difficult, causing itching and pain, but genital psoriasis can also have an impact on your sex life, relationships, and other aspects of life.
“Genital psoriasis can have a significant impact on patients’ psychosocial function due to intrusive physical symptoms, such as genital itch and pain, and a negative impact on sexual health/intimacy,” says Saakshi Khattri, MD, an assistant professor of dermatology, rheumatology, and internal medicine at Icahn School of Medicine at Mount Sinai in New York City.
Keep reading to find out how to spot genital psoriasis, ways to treat it, and how to live with the condition.
What is psoriasis?
Psoriasis is an inflammatory skin disease that occurs when your immune system revs up its production of skin cells.
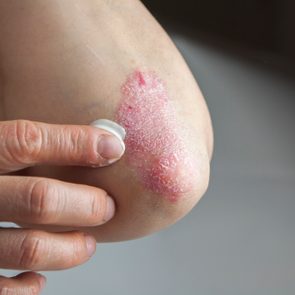
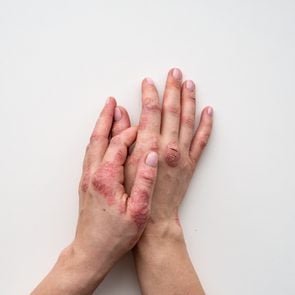
Instead of shedding, these cells build up on your skin, forming raised, reddened plaques that may be covered with silvery scales.
More than just a skin condition, psoriasis—and the underlying inflammation associated with it—can increase your risk of heart disease, type 2 diabetes, and depression.
Any type of psoriasis can take its toll on your self-esteem. But genital psoriasis, in particular, can make you self-conscious, both in and out of the bedroom.
Who’s most likely to get genital psoriasis?
In a study published in 2015 in the Journal of the American Academy of Dermatology, researchers set out to determine what factors led to the development of genital psoriasis. They found a few primary risk factors:
- Younger age of development of psoriasis
- Male sex
- More severe psoriasis
- Psoriasis of the scalp and nails
Where does genital psoriasis occur?
You may develop genital symptoms on the crease between your thigh and genital areas, your inner or upper thigh, your vagina, your penis, or your scrotum.
It may also appear on the skin above your genitals and/or in the crease between your buttocks.
When symptoms occur in skin folds such as your armpits, under your breasts, and in the genital area, it’s called inverse, or intertriginous, psoriasis, explains Bruce Strober, MD, a clinical professor of dermatology at Yale University and founder of Central Connecticut Dermatology Research in Cromwell, Connecticut.
Genital psoriasis symptoms
Symptoms may include red skin, discomfort, pain, severe itching, and splitting of the skin. Your symptoms may get worse when you sweat or if the area becomes irritated from rubbing.
There is rarely scaling with inverse psoriasis, as friction between skin surfaces can rub these scales off.
That said, silvery scales may occur when genital psoriasis plaques occur on the outer parts of your genitals, explains Dr. Strober, who is also the editor in chief of the Journal of Psoriasis and Psoriatic Arthritis.
Genital psoriasis and your sex life
People with psoriasis in their genital area have a higher odds of depression and report less-frequent sex, worse sexual function, and a diminished quality of life compared with those whose psoriasis doesn’t affect their genitals, according to the Journal of the American Academy of Dermatology study.
The study revealed other insights on how genital psoriasis can affect your sex life.
Nearly a third of participants said that their genital psoriasis symptoms got worse after intercourse, and 43 percent said sex was painful.
“Patients are often embarrassed by their genital psoriasis and do not mention it to their doctor, but it is very important to seek treatment of genital psoriasis,” says study author Caitriona Ryan, MD, an associate clinical professor at the University College Dublin in Ireland.

Genital psoriasis treatment
Genital psoriasis can be a challenge to treat because the skin in these areas tends to be thin and sensitive. The good news: relief usually comes quickly with the right topical treatment—sometimes in 48 to 72 hours, Dr. Strober says.
Steroids
Your doctor will usually start with a topical treatment, such as mild steroids—”mild” being the operative word. Higher-dose steroid can cause side effects like skin thinning, says Dr. Khattri.
Steroid-free topicals
Steroid creams and ointments aren’t your only options.
Steroid-free topicals include immune modulators (like pimecrolimus cream and tacrolimus ointment), which reduce inflammation and itch. Topical forms of vitamin D (like calcitriol or calcipotriene) can help slow down skin cell growth.
On the plus side, these are not steroids, so they won’t thin your skin, Dr. Khattri says. The downside? They may cause burning and stinging down there.
Antifungal and antibacterial treatments
When the psoriasis is in your skin folds, it provides a breeding ground for yeast, fungus, and bacteria, says Dr. Khattri.
Your doctor may supplement your psoriasis medication with a prescription for an antifungal or antibiotic drug, he adds.
Systemic therapies
When topicals don’t do the trick, your doctor may suggest bringing out the big guns, namely systemic therapies such as biologics or older disease-modifying drugs like cyclosporine or methotrexate.
Biologics work by blocking key proteins involved in the inflammation cascade.
Cyclosporine and methotrexate also target the overactive immune system in psoriasis.
How not to treat genital psoriasis
Some common psoriasis treatments should not be used on or near the genitals, the American Academy of Dermatology (AAD) warns.
This includes any type of phototherapy or UV light treatments. They up the risk for genital cancer.
Strong coal tar-based products can be highly irritating when used around the genitals, so skip them as well.
Another psoriasis medication, Tazarotene, works by slowing skin cell overgrowth, but it may also irritate the area, making genital psoriasis worse.
Living with genital psoriasis
In addition to taking your medication as directed, there are other things that can help reduce psoriasis flares—including those that affect your genitals.
Avoid psoriasis triggers
As much as you’re able, try to avoid common psoriasis triggers, like stress, illness, and injury.
Eating a healthy diet, getting regular physical activity, sleeping well, and engaging in some type of relaxation exercise every day can help boost your immune system’s function and lower stress levels.
Don’t irritate the area
Use only mild, fragrance-free soaps in your genital area. These are least likely to cause irritation, which can sometimes trigger a flare.
Moisturize regularly
Using a fragrance-free moisturizer after bathing or when the area feels dry can also help stave off irritation.
Don’t skimp on toilet paper
It’s worth it to pay extra for high-quality toilet paper because it’ll be less likely to irritate the already delicate genital area.
Be extra clean when wiping. If urine or feces comes into contact with genital psoriasis, you may flare.
Wear loose-fitting underwear and clothing
Choose your underwear and pants wisely. Loose-fitting styles will help you avoid friction.
That’s important because when psoriasis plaques rub against fabric, your symptoms can worsen.
Sex safety tips
You can have sex if you have genital psoriasis. It is not contagious or sexually transmitted.
Still, if your skin is inflamed and raw, consider postponing sexual activity, the AAD suggests.
It’s a good idea to clean the area with mild soap before having sex. This important step can remove any medication so it won’t rub off on your partner.
After sex, gently wash the area. This helps reduce irritation and can prevent a flare or worsening of any symptoms.
Men may want to use a lubricated condom, which lessens the risk of irritating the inflamed area, says Dr. Ryan, who is also a dermatologist at the Institute of Dermatologists and Blackrock Clinic in Dublin.
“I also recommend the use of lubricant for sexual activity to reduce friction,” she says.
Of course, it’s not an easy conversation to have with a new (or newish) partner, but it is an important one.
A partner may worry you have a sexually transmitted infection, says Dr. Ryan. So you may need to explain the condition and that you just have psoriasis, but that it’s not contagious and is manageable.
Next, learn about the most-promising psoriasis treatments.