9 Tips for Treating Psoriasis on Your Feet
Updated: Jul. 06, 2021
Psoriasis, an inflammatory skin condition, can damage feet. Here's what to know about foot psoriasis and how to treat it.
Psoriasis is common
If you have psoriasis on your feet, you know all too well that it can take a dramatic toll on your quality of life.
More than eight million people in the United States have psoriasis, according to the National Psoriasis Foundation. Of these, 40 percent have it on the soles of their feet or on their hands. Together, they make up a condition known as palmoplantar psoriasis.
Psoriasis occurs when your overactive immune system speeds up skin cell growth. As a result, skin cells start to pile up on the surface of your skin.
Normally, skin cells grow and shed in the span of a month. But with psoriasis, skin cells grow every few days and don’t shed, resulting in raised plaques and scales that may itch, burn, and sting.
A growing body of evidence shows that psoriasis goes more than skin deep. It tends to travel with an increased risk for heart disease, depression, and type 2 diabetes.
When plaques occur on visible parts of your body, psoriasis can mar your self-esteem and self-confidence.
And when these plaques develop on the soles of your feet, they can affect your ability to walk and move around.
Understanding psoriasis on your feet
The amount of skin affected by palmoplantar psoriasis differs from person to person.
“Sometimes you can have psoriasis on your feet and hands, just your hands or just your feet, and nowhere else on your body,” notes Bruce Strober, MD, clinical professor of dermatology at Yale University and founder of Central Connecticut Dermatology Research in Cromwell, Connecticut.
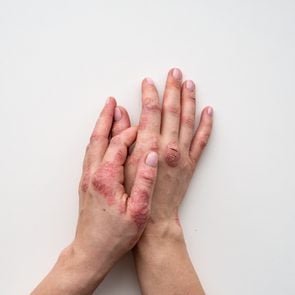
When your hands and feet are involved, your nails are likely affected, too, he says. Symptoms of nail psoriasis include white, brown, or yellow nails; denting or pitting in the nails; and crumbling.
Though foot psoriasis may not cover a whole lot of your body—at least compared with other forms of psoriasis—it can be more debilitating.
People with foot psoriasis are almost twice as likely to report problems with mobility as those with moderate to severe plaque psoriasis, according to a 2018 study in the Journal of the American Academy of Dermatology. They’re also almost 2.5 times more likely to say they had trouble completing daily activities.
What’s more, these folks fare worse on quality-of-life measures, even though they typically have less affected body surface area than people with psoriasis on other parts of their body, the study showed.
Foot psoriasis symptoms
If you have foot psoriasis, your feet may itch and/or develop scaling and reddened skin plaques on their soles, says Dr. Strober, who is also the editor and chief of the Journal of Psoriasis and Psoriatic Arthritis
Small, pus-filled blisters may develop on the affected areas, which can cause painful cracks. This is called palmoplantar pustular disease, or pustulosis.
As many as one in three people with psoriasis may also develop psoriatic arthritis, which is marked by swelling, stiffness, and pain in the joints.
If you have that condition along with foot psoriasis, you may develop swollen, sausage-like toes (dactylitis).
With psoriatic arthritis, you might also experience enthesitis, a painful swelling that occurs in the connective tissue that attaches your ligaments and tendons to your bones. It often strikes the sole of the foot and the back of the heel.
Foot psoriasis vs. athlete’s foot
Other conditions may look a little like foot psoriasis, such as athlete’s foot and eczema. That’s why it’s smart to check in with your doctor.
Athlete’s foot is caused by a fungus, and symptoms like scaling or peeling skin, inflammation, or swelling usually occur between your toes. It may spread to the soles of your feet and to your toenails.
Treatments for these various conditions differ, so getting an accurate diagnosis is the first step toward relief.

Treating psoriasis on feet
There are some unique challenges when it comes to treating foot psoriasis. Here’s what doctors most often recommend.
Topical therapy
Topical therapies are the go-to course of action. Usually, you’ll apply the treatment and then place a sock over your foot to make sure the cream does its job, Dr. Strober says.
The choices in topical therapy typically include steroid creams or calcipotriene, a form of vitamin D that slows down skin cell growth.
But topicals don’t always do the trick, says Saakshi Khattri, MD, assistant professor of dermatology, rheumatology, and internal medicine at the Icahn School of Medicine at Mount Sinai in New York City.
“The key reason for the failure of topical agents to work is the thick stratum corneum [outer layer of skin] on the soles and palms, which acts as a barrier to the effective penetration of topicals,” she says.
Topical treatments like emollients (non-cosmetic moisturizers), steroids, and coal tar foams are available over the counter. Prescription-strength versions are available if you require a stronger formula.
Light therapy
Light therapy is another way to treat psoriasis. Also known as phototherapy, light therapy will expose you to ultraviolet light, which helps target itchiness, redness, and other symptoms.
While at-home light therapy is an option, typically the treatment occurs under a doctor’s supervision at a hospital or clinic.
For this to be effective, it can take between two to three treatments a week. Your doctor will want to gauge your sensitivity to UV light and monitor your progress.
Before you do this, talk to your doctor about the benefits and risks, including the increased risk for skin cancer.
Systemic treatments
If topicals and light therapy don’t work, your doctor may opt to try a systemic treatment such as a biologic drug (infliximab or adalimumab).
These medications block specific proteins, such as tumor necrosis factor (TNF), which can amp up inflammation in psoriasis.
Some other examples of systemic treatments include immunosuppressants (methotrexate or cyclosporine), steroids, phosphodiesterase-4 inhibitors, and retinoids.
Lifestyle changes for foot psoriasis
Taking good care of your feet can go a long way toward improving symptoms and preventing psoriasis flares. Here’s how to modify your lifestyle for your condition.
Avoid injuries
Accidents happen—no one won’t be able to stay completely unscathed. But try to be extra careful to avoid injuries.
Even a tiny scrape or scratch can cause a Koebner phenomenon, the medical name for a psoriasis flare that occurs in response to injury.
Moisturize
Keeping your skin well moisturized will help relieve some of the symptoms of psoriasis on feet, such as itching and flaking.
(This is the best skin care routine for psoriasis, according to top dermatologists.)
Pick comfy shoes
Always wear comfortable shoes. This may mean putting function before fashion.
Make sure your toes have wiggle room, and just say no to high heels. They put too much pressure on nails and joints, which can increase pain.
“Choose any footwear that minimizes trauma and allows great comfort,” Dr. Strober says. “Basically, psoriasis relies on trauma in many patients, and you want to minimize that effect.”
Still, he notes, “good footwear won’t replace good medical therapy.”
Follow a psoriasis-friendly diet
It’s important to watch what you eat, as some foods may increase your risk of a psoriasis flare. Chili peppers, tomatoes, and dairy products are common culprits.
Reduce stress
Psoriasis can worsen when you’re stressed. Do your best to reduce stress. If that’s inevitable at work or home, find ways to de-stress, such as learning how to meditate and making meditation a daily practice.
Make an appointment with your doc
If you have foot psoriasis, check in with your doctor to make sure you are doing everything you can to minimize flares and take back your life and lifestyle.