4 Types of Toenail Fungus and How to Treat Them
Updated: Aug. 05, 2022
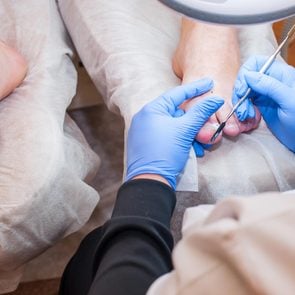
Those yellowish and thickened toenails could mean you have an infection with a toenail fungus. Here are the types, symptoms, and how to treat fungal infections of the toenail.
Toenail fungal infections
If your toenail becomes discolored with white or yellow spots, it could signify the beginning of toenail fungus, or onychomycosis, as doctors call it. These pesky fungi are to blame for about 50 percent of nail problems. Toenails are affected four to 10 times more frequently than fingernails.
A toenail fungus doesn’t pose a danger to your overall health unless it goes untreated. If the fungus has free rein, it can cause even more discoloration and the nail to become thick and brittle. The nail may even fall off, and it could spread to the other nails in your foot.
“Fungal infections of the foot and toenails rarely, if ever, resolve on their own. They almost always require prescription management for resolution,” says Joseph Zahn, MD, a dermatologist at George Washington University Medical Faculty Associates, Washington, D.C.
Here’s what you should know about the types, symptoms, risks of toenail fungal infections and how to treat them.
Who gets toenail fungal infections?
A fungus can invade the toenails of anyone at any age, but it is far more common in older adults. Once you hit 60, your chances of getting a toenail fungus increase to about 75 percent. The odds are higher because blood flow is reduced as we get older, which slows nail growth. Nails become more dry and brittle, causing them to crack.
A fungus can enter through a break in the skin or under or beside the toenail. And quite frankly, toenails just get more difficult to reach and trim as our flexibility declines.
“Longer nails are more prone to trauma, so older adults who may have trouble trimming their nails are at risk for trauma and subsequent infection,” says dermatologist Shari Lipner, MD, associate professor of clinical dermatology at Weill Cornell Medicine, New York.
(Here’s what to know about ingrown toenails.)
Risk factors for toenail fungal infections
Besides age, here’s some other risk factors:
Athlete’s foot
Athlete’s foot is one of the reasons fungal infections are more prevalent in toenails than fingernails. It’s a fungus that thrives in warm, moist places.
“It’s the most important risk factor for fungal nail infections. The exceptions are people that are immunosuppressed,” says Dr. Lipner, who also serves as director of the Nail Division at Weill Cornell Medicine.
“People with fingernail fungal infections almost always have toenail nail infections as well.”
(Here are some home remedies for athlete’s foot to keep on hand.)
Shoe choice
Wearing tight, closed-toe shoes and sweating creates the ideal breeding ground for fungus.
Walking barefoot
Be careful about walking barefoot in areas where fungus flourishes around swimming pools, locker rooms, gyms, or other public showers such as college or campgrounds. Opt for flip-flops instead. It’s also risky to walk barefoot in the same house where another person has athlete’s foot.
Health conditions
Certain health issues can make you more likely to develop a fungal infection in a nail. Having skin or nail injuries or a skin condition like psoriasis (a skin conditions that causes red, scaly patches) can allow fungus to enter the nail bed.
Diabetes and other circulation problems that affect nail health and the immune response
Types of toenail fungus and symptoms
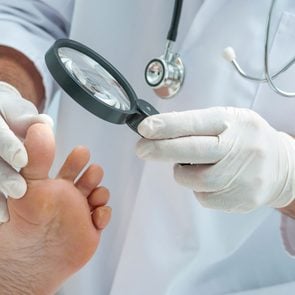
“The symptoms of most fungal toenail infections are similar,” says Dr. Zahn. The hallmark symptoms include nail discoloration, nail separation, brittleness, thickening of the nail, and sometimes pain.
Yet, those symptoms are present in other conditions like psoriasis or from banging your toenail. With the symptoms so similar, it’s difficult to identify the type of fungal infection on your own.
Your doctor or dermatologist may take a small sample of the debris beneath the nail, trim the nail, or scrape a tiny bit of skin to pinpoint the type of fungus.
Distal subungual onychomycosis
This type of toenail fungus is the most common subtype of onychomycosis, which may not be encouraging if you have it, but it is good news when it comes to treating it.
“Since distal sublingual onychomycosis is the most common subtype, we have the most information about how to treat the infection effectively,” says Dr. Lipner. In this type, the fungus invades the nail bed underneath the nail.
Signs and symptoms
- More common in the big toenail than other toenails
- Thickening of nails usually yellowish-white to yellowish-brown in color or may appear as yellow streaks in the center of the toenail
- Nail may be jagged and chipped or come apart from the nail bed
- Pain and mild inflammation in the toenail area
White superficial onychomycosis
White superficial onychomycosis is less common than distal subungual onychomycosis and presents differently.
“The infection is on the top layers of the hard part of the nail, not deep under the nail, so it’s generally easier to treat,” says Dr. Lipner. Unlike other fungal infections, which can affect fingernails and toenails, white superficial onychomycosis affects only the toenails.
Signs and symptoms
- Small, white, speckled “islands” randomly appear on the surface of the nail plate
- Nail becomes rough, soft, and crumbles easily
(Here are other possible causes of white toenails.)
Candida infection
“Candida is a yeast that is found in the environment, and sometimes just lives on the skin as a part of our normal skin flora,” says Dr. Zahn. It actually attacks the soft tissue around the toenail first, then penetrates the toenail.
It’s difficult to tell the difference between Candida toenail fungus from another fungus without taking a sample and having it tested. And it typically is found in fingernails more than toenails, especially if hands are routinely in water.
Signs and symptoms
- Skin around toenail is reddish
- Nail has white, brown, or yellow discoloration
- Nails may become brittle and split, causing partial or total destruction of the nail
Proximal subungual onychomycosis
The rare toenail infection begins when the fungus invades from the proximal skin—where the nail meets the toe, behind the toe’s cuticle, and progresses distally across the nail. As it spreads, it penetrates the newly forming nail.
“Proximal toenail infections, especially those that progress quickly, have been associated with immunosuppression, including HIV/AIDS, but it can be seen in otherwise healthy people, albeit uncommonly,” says Dr. Zahn.
Signs and symptoms
- Starts as a diffuse white patch in the center of the cuticle
- As the toenail grows out, white spots move outward
- Toenail separates from the nail bed, destroying the toenail
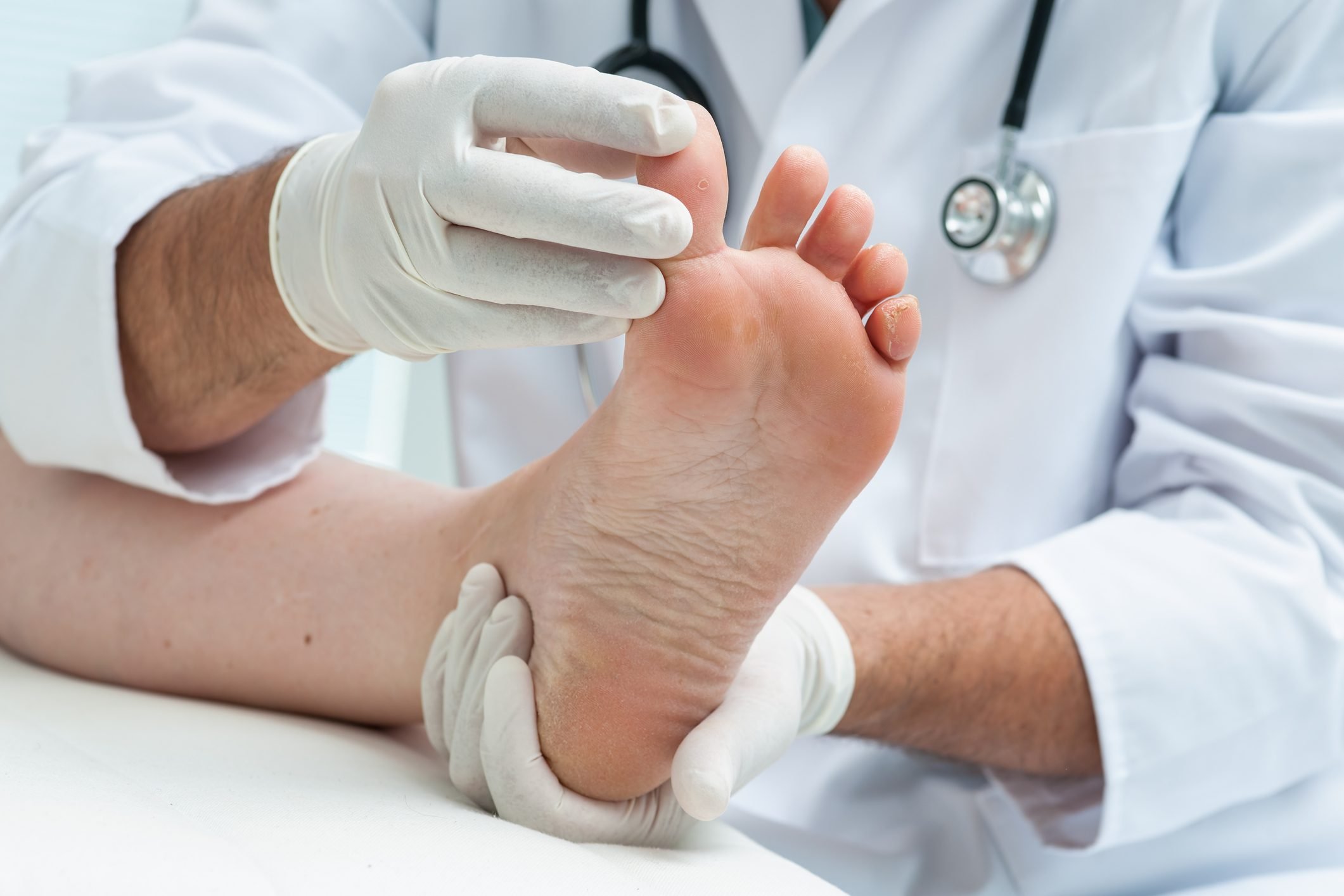
When to see a doctor
A tiny white or yellowish spot on your toenail without any bothersome symptoms may not point to a toenail fungus infection. But if your toenail changes in appearance or you have pain, it might be a sign of a full-blown toenail fungus infection that needs medical treatment.
Call your doctor if you see these symptoms:
- Nails that become powdery, thick, brittle, or split
- Nailbed shape changes
- Mild or foul odor emitting from the toenail
- Any systemic symptoms such as fever, chills, night sweats, or weight loss
Toenail fungus infection treatment
As a rule, toenail fungal infections require medical treatment. Over-the-counter products might help some of the symptoms, but it’s a temporary fix. To completely eradicate the fungus and keep it from spreading to other nails—or people—prescription medicine is necessary.
Fair warning—this isn’t a “one and done” kind of treatment. “It’s a one year for cure with both orals and topicals, says Dr. Lipner. “Orals are taken for three months, and topicals are taken for one year.” One topical treatment Dr. Lipner often prescribes to her patients is JUBLIA, a solution that penetrates the nail plate to reach the nail bed, inhibiting existing fungi from growing and reproducing right at the source.
Toenails grow on average about one millimeter per month, and it takes a least a year for an entirely new, healthy toenail to grow. Treatments vary depending on the type and severity, but typically antifungal medicines are applied to the toenail daily or weekly, while you also take antifungal medicine pills.
It’s rare, but when medication doesn’t resolve the problem, the toenail is surgically removed or non-surgically with a chemical applied to the nail. The nail can grow back, but if the fungus is persistent, a dermatologist can treat the nail so it doesn’t grow back.
(Do you have ridges in your fingernails? This is what it could mean.)
Prevention tactics
Now that you know treating toenail fungus infections is a lengthy process, you might be more invested in avoiding one or getting a repeat infection.
Here’s how to keep fungus at bay:
- Keep your feet clean and dry.
- Wear flip-flops or sandals when you’re in warm, moist areas, such as public showers, pools, and locker rooms.
- Put on a clean pair of socks every day, or change socks often if your feet get sweaty.
- Don’t wear tight-fitting shoes or shoes with non-breathing material.
- Allow wet and damp shoes to dry out, or place them on a shoe dryer. Or sprinkle anti-fungal foot power inside the shoe.
- Keep your toenails shorter than the end of your toes, and cut them straight across to avoid sharp angles.
- Moisturize dry skin, so fungus can’t sneak in the dry cracks.
- Sanitize your nail clippers with soap and water, followed by alcohol.
- Choose nail salons that disinfect their tools after each client.
- Ditch any footwear you wore before you were infected or use an ultraviolet shoe sanitizer to keep fungus from returning.
Living with a toenail fungus infection
A toenail fungus might not seem like a big deal compared to other health conditions, but it can affect daily life activities and function to some degree.
(To soothe your symptoms, try a foot soak for toenail fungus.)
“Some patients experience pain, difficulty doing everyday activities, and fitting shoes. There is also a stigma surrounding nail fungus so many people are embarrassed that they have this,” says Dr. Lipner.
Treatment is a lengthy process. It can be daunting to keep up with the treatment schedule when the results are slow coming.
If you’re feeling depressed, embarrassed, and tired of dealing with pain and staying on top of your treatment, reach out to your doctor or mental health professional to chat about your concerns.
Next, these are the common foot problems and podiatrists’ solutions.