
To learn you have diabetes or pre-diabetes might feel disappointing and worrisome, with a lot of questions and uncertainty about how to manage. But before you feel despair, consider this: you have an empowered choice in how you respond to this health condition. With the Centers for Disease Control and Prevention (CDC) estimating that nearly 40 million Americans have diabetes, so many advancements have been made to help you effectively manage diabetes or pre-diabetes—or, with some knowledge and support from the right clinical professionals, it may be possible for you to reverse diabetes completely.
To celebrate the release of the latest edition of the Reader’s Digest perennially popular Reverse Diabetes book, The Healthy @Reader’s Digest spoke with doctors, dietitians, and other diabetes specialists to create a list of a few helpful items it might be worthwhile for you to consider try. If any of these seem beyond your budget or your health insurance falls short of covering them, consider asking your healthcare provider about them anyway. Some hospital systems, health clinics, or other healthcare organizations may offer a few of these products at no cost or at a discounted rate for patients who qualify.
For daily health and wellness updates, sign up for The Healthy @Reader’s Digest newsletter
Blood glucose meter
A blood glucose meter is a portable device that quickly measures the amount of sugar in your blood. “Some meters have extra features, such as a linked smartphone app,” says Jacqueline Lonier, MD, an endocrinologist at Naomi Berrie Diabetes Center of Columbia University Medical Center. Still, she says that these features don’t affect a meter’s basic functionality. “All blood glucose meters must meet the same accuracy requirements specified by the [United States Food and Drug Administration (FDA)].”
So, she advises you check with your insurance to see which options are covered. Also, says diabetes specialist and doctor of pharmacy Stephanie Redmond, PharmD, CDCES, BC-ADM, don’t lose heart. “If you’re battling insurance to cover your supplies or have a high deductible, try less expensive options.” Dr. Redmond points to the ReliOn Blood Glucose Monitoring System as a quality, cost-effective model. “This product is very easy to understand and use,” writes user Michael K. Le Monier. “It prompts you and then quickly gives you information,” while requiring very small blood samples.
Other top-rated glucometers recommended by the American Diabetes Association include:
-
The Contour Next One, a super compact device with a built-in test strip light and Bluetooth capability for easy data storage. “I’ve tried other meters, and this is by far the easiest to use,” writes user KH. “The amount of blood required is about a third of other meters, and if you don’t have enough on the first try, you have upwards of 30 seconds to add more without an error and a wasted strip.”
-
The DARIO Monitor Kit, a user-friendly smart device that compiles trend reports right on your phone. “I am so impressed by this little device,” writes user SammiP. “I love that it goes to my phone and is recorded in an app where I can show my doctor what my blood sugars have been running—super convenient!”

Continuous Glucose Monitoring (CGM) System
“I am huge on having patients try these,” Dr. Redmond says. “It shows you in real-time what your blood sugars are doing based on different foods, exercise, how you react to stress, and good or bad sleep.” For example, how your blood sugar responds to certain foods is likely to be totally different than the way a friend’s blood sugar would respond to the same snack. Therefore, Dr. Redmond says, a continuous glucose monitoring system “truly is the best tool in learning your own body.”
Best of all? Continuous glucose monitoring systems require no finger pricking. Jonda Dawson, RN, CDCES (Certified Diabetes Care and Education Specialist), explains that the technology aims to reduce time spent in hypoglycemia and improve overall glycemic management. “Each reading is displayed within an app on a person’s smartphone that can be reviewed with a quick glance,” Dawson says.

Athletic shoes
People with diabetes are at a higher risk of developing foot problems like ulcers, infection or nerve damage—and choosing the right footwear can help keep your feet in great shape. Larissa Rolim, a board-certified podiatrist in Dallas-Fort Worth, says there are three main factors to consider when shopping for athletic shoes:
Width: “Narrow shoes can cause blisters or calluses that can lead to ulcerations,” she says. “I always recommend trying new shoes on later in the day when the foot can tend to be a bit more swollen to make sure they are buying the correct width.”
Shoe material: “Choose a flexible top material like neoprene, soft leather, or knit,” she says. “These will avoid placing undue pressure on [your bones] that can lead to a breakdown of the skin.”
Support: “For walking shoes, look for a shoe with a shock absorbing outsole to help reduce pressure to the joints of the foot,” she says.
Every foot is different, so you’ll need to try shoes on to make sure they’re the right fit. And for people with diabetic neuropathy, she advises you wear new shoes at home for 30 minutes and then check for any signs of pressure points or redness.
As a starting point, Dr. Romlin points to her favorite athletic sneakers for patients with diabetes:
- New Balance 990 Series—Thousands of reviewers rave about this New Balance shoe, including user James Gouveia. “I am diabetic and these shoes are great for that and so much more,” he writes.
-
ASICS Gel-Excite—These shoes are so supportive, they’re a favorite of people who spend long hours on their feet at work. “They are so comfortable and supportive for me being on my feet for 12-hour shifts,” writes hospital worker Emma. “And have even relieved some of my [pregnancy] back and knee pain!”
-
Hoka One One Bondi—According to Amazon reviewers, this shoe is great for a wide range of food problems, like plantar fasciitis, bunions, and swelling. “I have swelling in my toes and the balls of my feet due to rheumatoid arthritus and have been unable to wear any of my normal shoes for the last year, writes user Norahs yarn. “This is the first time in a year I have been able to wear a pair of any shoes for longer than an hour.”

Diabetic socks
Socks designed for people with diabetes help promote circulation and prevent irritation. They’re typically seamless and made from breathable material that keeps your feet dry and friction-free, reducing the risk of issues like blisters and infection.
Bruce Pinker, DPM, a board-certified podiatrist and foot/ankle surgeon in New York, recommends these diabetic socks to keep your feet healthy:
- Dr. Comfort Diabetic Socks, which come with a padded heel and toe to prevent foot injuries—and “comfortable, stretchy, and soft while still providing some compression,” according to user Sandra.
- Jobst Diabetic Socks for sensitive feet, with mild, non-restricting compression—”not a strong amount of compression, but enough to make a difference,” which makes them easy to put on, says reviewer Pam Edmoundson.
- Orthofeet Padded Diabetic Socks made with anti-blister natural bamboo fibers—a material so soft it’s barely there. “I like the feeling (or non-feeling) of these socks,” writes user RC. “I say ‘non-feeling’ because you don’t even know you’re wearing them. Perfectly comfortable.”
Your feet should be supported and protected at home, too. Podiatrists say these are the best diabetic slippers for men.

Compression socks
“Compression socks or sleeves are great for reducing diabetic foot swelling,” explains Jeffrey Hurless, MD, a board-certified podiatrist and foot/ankle surgeon. Because diabetes can affect your blood circulation, this can cause fluid to build up in your foot or ankle. If left untreated, swelling can increase your risk of infection and, over time, diabetic neuropathy.
Dr. Hurless says that the Darco DCS Plantar Fasciitis Sleeve is a good option because it offers a snug fit with a breathable, stretchable and machine-washable material. “This makes a world of difference for my food,” writes user S. Kachelmeyer. “It helps relieve the pain when it flares up and keeps my foot in good shape when walking,” while being comfortable enough to wear all day.
But Dr. Hurless urges: “Always be sure to consult with your doctor before using compression wear, as it’s not suited for all diabetic patients.”
15 Things Diabetes Doctors Do to Keep Their Own Blood Sugar Under Control

Skin cream
People with diabetes are very prone to skin dryness—which can be exacerbated by certain medications, says Cybele Fishman, MD, a board-certified dermatologist with Advanced Dermatology PC.
She says that a cream or ointment is typically better than a lotion when it comes to moisturizing. “CeraVe came out with a line of diabetic skin care, which I like as it has both ceramides and urea.” Ceramides are fats found naturally in our skin, which work to maintain a strong, healthy skin barrier. Our skin also contains urea—and when it’s added to skincare products, it’s shown to relieve dryness and irritation, improve absorption of other moisturizing ingredients, and act as an antimicrobial, according to research published in Dermatology and Therapy. “My wife has diabetes and has tried more lotions and creams than I can imagine,” writes reviewer Z. Kluza. “Finally, she came upon CeraVe and it does what it claims—it’s excellent for your legs and feet and it does not leave a greasy residue.”
Dr. Fishman also recommends Vanicream and the La Roche Posay Lipikar line for people with diabetes.

Foot powder
People with diabetes also have a higher risk of skin candida (yeast), fungal, and bacterial infections on their feet, Dr. Fishman says. These issues aren’t just uncomfortable, either. If the skin breaks—like with a cut, abrasion, or open blister—this becomes a portal of entry for bacteria to go into the soft tissue, which can cause cellulitis.
“In general, wash your feet daily and dry them well, especially between the toes,” she says. “Moisture makes it easier for fungus and yeast to grow.” She recommends keeping Zeasorb AF Powder on hand, which contains an antifungal agent as well as ingredients to absorb moisture. “This is a good thing to sprinkle in your shoes and use on your feet if you get yeast or fungal infections.” User Cheri W. Astrahan backs this up, saying that as a diabetic, she’s prone to fungal infections. “[It] wasn’t controlled by the usual cream,” she writes. “A dermatologist recommended Zeasorb and it really has helped control a chronic condition.
But Dr. Fishman emphasizes that someone with diabetes who has foot or toenail issues should let their doctor know, as it could indicate that you’re at risk for other health conditions.
A Woman in Her 20s Shares What It’s Like to Have Diabetic Foot Problems
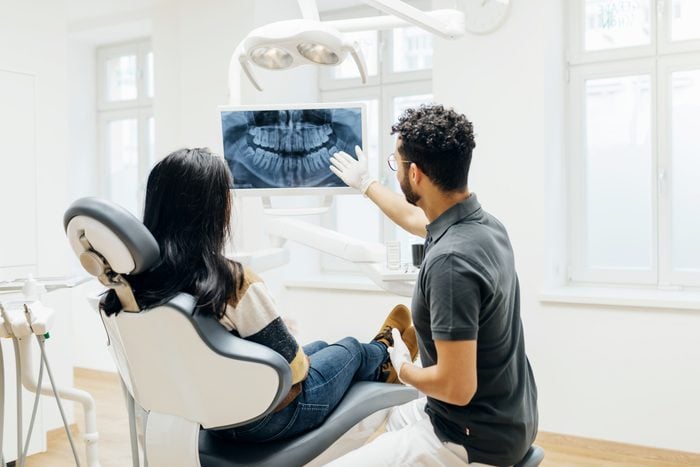
Dental care
According to research published in the British Dental Journal, people with diabetes are two to three times more likely to develop periodontal (AKA gum) disease. “Oral hygiene is essential for anyone living with diabetes or prediabetes, especially considering the increased susceptibility to infections and delayed wound healing that occurs with diabetes,” says Jordan Weber, DDS, a general dentist in Kansas.
He recommends:
-
Oral-B iO Series 9 Electric Toothbrush, a top-of-the-line “smart” toothbrush that accounts for brushing pressure and equal coverage—”Hands down the best toothbrush on the planet,” writes user JWeis. “I straight up feel like I just left the dentist.”
-
Oral-B Pro 3000 Electric Toothbrush, a more affordable model with built-in timers and app-compatibility—”My teeth have never felt better, and I felt like it whitened my teeth after just one use,” writes user Rachel Kolodziej.
-
Waterpik Ultra Water Flosser, which Dr. Weber says is a great way to clean between the teeth and the gum line—”areas that are the most important to keep clean for anyone concerned about gum disease.” Plus, this model gives you an extremely thorough clean, according to user Sheldon R. “I have been using a Waterpik for years but this one has so many different nozzles for getting into hard to clear spots.”
-
Under the Gums Irrigant Concentrate, a solution Dr. Weber says can be used with a water flosser and is often more effective than using water alone. “This stopped my periodontal disease,” writes user Daniela, who usis it frequently throughout the week alongisde regular flossing.

Sugar alternative
People with diabetes can generally indulge a sweet tooth in moderation (though always defer to your doctor’s dietary guidance.) But for people trying to lower their blood sugar, cutting the sweet stuff as much as possible can go a long way (just look at the impact quitting sugar had for this diabetes patient).
“Purecane [sweetener] is a great option in place of traditional sugar because it does not have any effect on blood sugar levels,” says registered dietitian Megan Roosevelt. Amazon reviewers like Jennifer Danni Elle say it actually tastes like sugar and “doesn’t leave an aftertaste like some alternative sugars do.” And, for you bakers and chefs out there, Purecane blends smoothly and can be used 1:1 for sugar in recipes, making it an easy-to-use substitute, according to user Addie K. Ziegler.
For more, check out these 11 other healthier sugar substitutes.

Supplements
A diet rich in natural, unprocessed foods goes a long way in helping people manage prediabetes and type 2 diabetes, says Sudeep Singh, MD at Apprize Medical in Miami. (And here are 50 blood sugar-friendly foods registered dieticians recommend.) But fiber is a magic bullet, nutritionally. That’s because “fiber works with insulin to decrease blood sugar spikes,” he explains, and can also work well with prebiotic foods like bananas, oats, and garlic to decrease blood sugar levels by improving your gut flora.
While the best nutrition comes from your diet, supplements can play a role in helping to fill any gaps. For his patients with diabetes, Dr. Singh recommends mixing Renew Life’s Organic Prebiotic Powder and Organic Psyllium Husk in water as a shake. “Garden of Life’s Beyond Fiber Super Seed is also an excellent source of sprouted seeds, which most people lack in their diet,” he says. “It’s my best help against indigestion and sluggish bowel,” writes user David Neuenschwander. “I feel better when I use it.” But a reminder: always talk to your doctor before adding any supplements to your diet.
6 of the Best Dietary Supplements for a Diabetic Diet—and 3 You Should Avoid

Activity tracker
Exercise is consistently proven to help control diabetes (and here are 13 other major benefits.) One of the largest randomized controlled trials to date showed that people who are active at least 175 minutes a week had fewer diabetes complications. Past research has also found that aerobic exercise like walking helps to slow the development of neuropathy, or nerve damage.
“A fitness tracker is an objective measure that helps you to set step count goals and track them, which are key motivators for increasing physical activity,” says Justine Chan, MHSc, RD, CDE, Registered Dietitian and Certified Diabetes Educator based in Toronto. She points to a study published in the Journal of Diabetes & Metaobolic Disorders that found using a fitness tracker helps people with diabetes stick to their exercise routine, improving their quality of life.
Chan recommends Fitbit trackers for monitoring activity because through the app, they also track other important measures like sleep, heart rate, and blood sugar trends. “I’m amazed at the quality of the output summaries for exercise, sleeping, food tracking, calories, nutrients, and macros which are very good and user-friendly,” user Rich B writes of the Fitbit Charge 5 Advanced model. As a personal trainer, he says “I’ve found this to be one of the most useful products out there and probably the best value for money.”
Here’s how long you should walk to lower your blood sugar levels, according to research.
For more wellness updates, follow The Healthy on Facebook, Instagram, and Twitter. Learn more about the latest in diabetes management:
